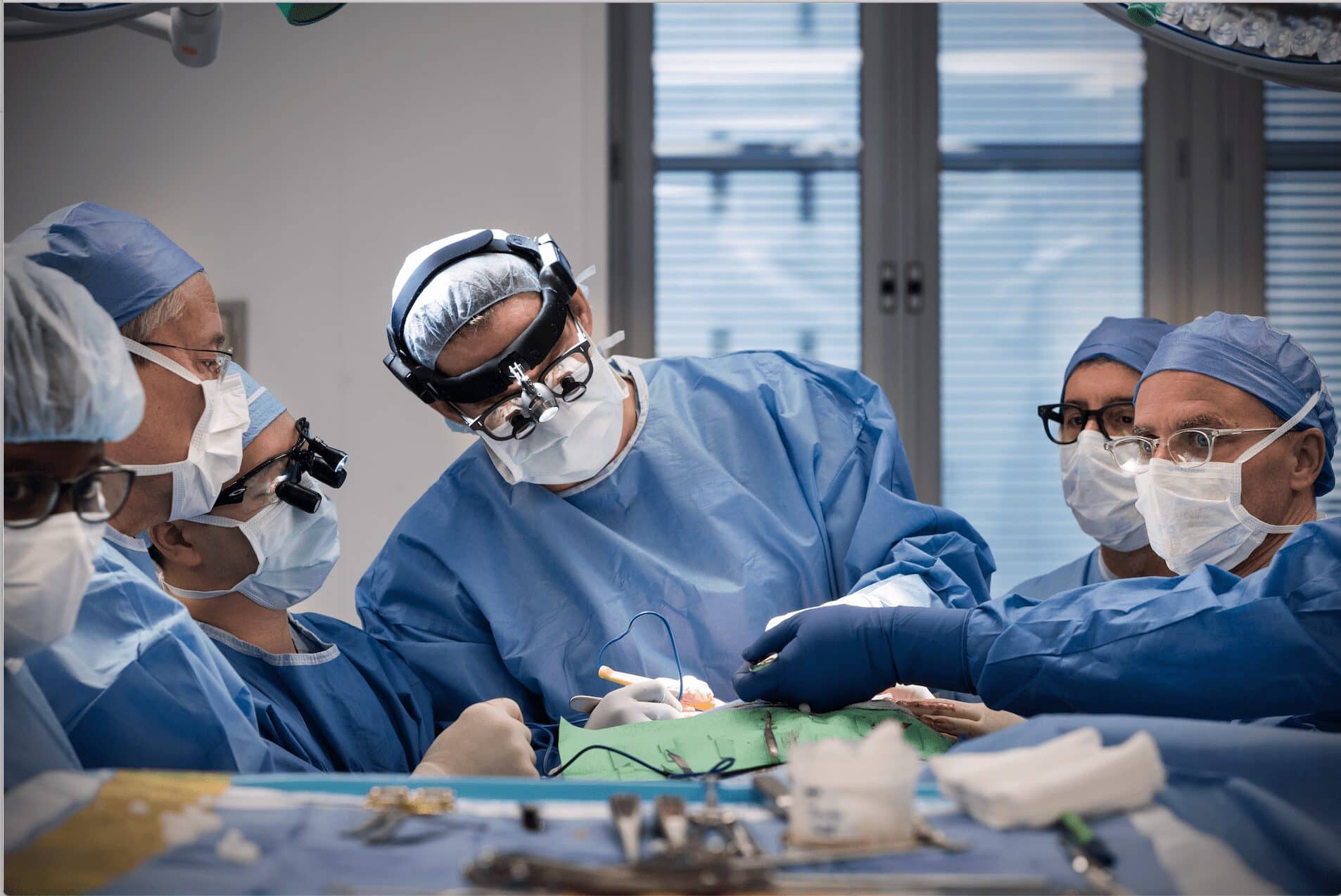
Dr. Hollier and his colleagues perform a surgery at the Texas Children’s Lester and Sue Smith Legacy Tower in 2018.
By Tonya Johnson
After years of the “fly-in” model of medical missions to provide cleft care, board-certified plastic surgeon Larry Hollier, Jr, MD, FACS, says the solution is not more missions but addressing the root causes, which is a shortage of providers and resources. He says some countries have only one pediatric surgeon serving millions of people, and two-thirds of the world’s children don’t have access to safe surgical care.
“Every three minutes, a baby is born with a cleft. In the US, people often think of cleft lip and palate as cosmetic, but it comes with physical challenges that can be life-threatening without medical intervention,” he warns. “Babies with untreated cleft lip and palate struggle to eat, to breathe, and as they get older, to speak.”
The cleft care charity Smile Train is one organization that has aided local medical professionals around the globe for more than 20 years. Recently, it teamed up with Scotland-based Kids Operating Room (KidsOR) to further healthcare access for children living in Africa. Hollier recommends that all doctors look into how they can advocate for sustainable, locally owned solutions and support them in their practice.
In addition to helping practitioners provide safe cleft surgery and ongoing cleft care, Smile Train has increased its focus on patients’ nutritional and psychological needs.
As chair of the global medical advisory board of Smile Train, Hollier works with the organization’s regional medical advisory councils and its global partners to uphold and elevate global standards for safety and quality for cleft therapies.
Hollier is the surgeon-in-chief at Texas Children’s Hospital; at Baylor College of Medicine, he serves as chief of plastic surgery and professor of plastic surgery, orthopedic surgery, and pediatrics. Specializing in pediatric facial reconstruction, Hollier has conducted thousands of procedures with a focus on cleft and craniofacial repair for the past 25 years.
When it comes to cleft care, Hollier explains that it’s crucial to have plastic surgeons, pediatricians, orthodontists, pediatric dentists, speech specialists, otolaryngologists, audiologists, genetic counselors, nurse team coordinators, and psychologists all working together. “The fact that our providers are on the ground full-time makes a real difference in the standard and the type of care we’re able to support,” he says.
Practice Surgery Practice (PSP) interviewed Hollier to learn more about his career, the Smile Train mission and partnerships, and the effects of a COVID-19 on both.
PSP: How did you become involved with Smile Train?
HOLLIER: My journey to Smile Train came from my involvement in global surgery. In the past, I have traveled to Haiti, Africa, Central America, and Southeast Asia to provide treatment for craniofacial and hand deformities.
However, that’s actually not how Smile Train approaches cleft surgery and cleft care in developing countries. For Smile Train, there’s no fly-in team and there are no “mission trips.” We partner with more than 1,100 local medical professionals around the globe, providing the funds, equipment, and training needed to provide cleft surgery and sustainable, ongoing cleft care to patients in their own communities. Our model of care and the power of our global partner network is the reason we’ve grown to be the world’s largest cleft organization, and one of the reasons we have been able to support the more than 1.5 million surgeries.
By utilizing this partnership model of care, Smile Train empowers local surgeons and cleft teams to provide a higher standard of care for patients with cleft lip and palate. Medical professionals are with patients throughout their entire journey of care, and they’re close by if the patient needs follow-up care. Cleft especially requires a lot of planned, ongoing care to ensure the best outcomes. The partnership also means that local medical professionals are leading the way in their own countries. Smile Train is investing not only in providers and patients but in the future of surgical care around the globe.
PSP: Describe Smile Train’s latest partnership with KidsOR.
HOLLIER: The new partnership with KidsOR is important and exciting. KidsOR is committed to providing every child around the world with access to safe surgery and anesthesia. In many developing countries, there aren’t dedicated pediatric operating rooms and surgeons don’t have the specialized equipment required for pediatric surgery. This means that many children don’t have access to the care that they need when they need it. KidsOR and Smile Train want to be part of changing this.
KidsOR provides these much-needed dedicated pediatric operating rooms in developing countries, ensuring that providers have the tools they need to provide safe pediatric surgery. The organization works directly with local teams, and also provides funding for local surgeons and anesthetists to become pediatric specialists.
This partnership between Smile Train and KidsOR is a collaboration between two very like-minded organizations focused on local leadership, sustainability, and training. We are very glad for the opportunity to work with them to provide these renovated, dedicated pediatric operating rooms at our partner treatment facilities because we know it will ensure that thousands of children with cleft lip and palate and other treatable surgical conditions will get the lifesaving care they so desperately need. It will change the landscape of pediatric surgery across many countries in Africa.
PSP: Why is it important to raise awareness about cleft lip and palate conditions; and the Smile Train mission?
HOLLIER: Unfortunately, families and children impacted by cleft in developing countries often don’t have access to care. Usually, there aren’t enough surgeons or anesthetists, and a trip to the nearest hospital can take multiple days of walking—not to mention the prohibitive cost of travel, surgery, and follow-up care. Smile Train is working to change this for current and future generations.
PSP: How have Smile Train and its partners changed the lives of patients and families?
HOLLIER: Families and patients express many emotions and reactions. Amazement. Disbelief. Joy. Smiles. We hear stories of children going to school for the first time, stories of parents who are overjoyed to see their shy child come out of their shell, stories of lives saved, and futures restored.
For so many of the families that our medical partners work with in developing countries, having a child with cleft lip and palate is overwhelming. Many babies with cleft palate, and to some degree cleft lip, struggle to eat. Imagine feeding your child and having them choke on the milk. Imagine seeing your newborn struggle to gain weight because they can’t latch effectively when they breastfeed.

Families often face discrimination from their community due to so many myths around cleft lip and palate. Mothers and fathers are often anxious for their children and for their future. Many people around the world don’t know that surgery and ongoing comprehensive cleft care is available, and even those who know often can’t afford the surgery and ongoing care or are too far from a hospital to receive care.
This is where Smile Train and our partners come in. Our global staff works to raise awareness of free cleft treatment opportunities. We offer funding for travel, for lodging, for food, for all the invisible barriers to care that might stand in the way of patients coming to get surgery. We support our partners to provide surgical care, and, where available, speech therapy, nutrition support, dental and orthodontic care, and psychosocial support. We want that happy story and that happy future for every child and every adult with a cleft lip and palate.
PSP: What do you enjoy most about being a craniofacial and plastic surgeon?
HOLLIER: In my field, I get to be part of incredible experiences and outcomes. Craniofacial conditions affect how a child hears, breathes, chews, swallows, and interacts with other people. It affects their identity and their experience of the world. When a child comes in with a craniofacial condition like cleft lip and palate, treatment can change their life. Treatment can save their life. It’s incredibly rewarding to be able to transform someone’s future and accompany them on that physical and mental journey.

What I’ve enjoyed most as a plastic surgeon focused on children, has been having the opportunity to watch them grow and overcome the obstacles that have been put in their way. The determination and bravery of these children is inspirational to me and the team around me. It’s hard to fully convey the impact that it has had on me personally and professionally over the years.
PSP: What has been your most difficult surgical procedure?
HOLLIER: All cases have their unique challenges. If I had to pick one type of case, it’s the separation of conjoined twins. Whether conjoined at the head or throughout the body, the effort and teamwork that goes into a successful separation is unbelievable.
PSP: What is the follow-up for a cleft-craniofacial procedure?
HOLLIER: The follow-up for cleft surgery is extensive. It is not typically just one surgery. Children typically undergo surgery on the lip at three months of age, and if the palate is involved, there is a procedure to close that closer to a year of age. Subsequent surgeries focus on speech and the dentition, alongside speech therapy and ongoing dental evaluations. Follow-up often continues for 18 years or more. That’s why having partners on the ground, building these ongoing cleft care programs, is essential to ensuring the best future for the patients we support.
PSP: What are the biggest challenges you have faced during the COVID-19 pandemic?
HOLLIER: The COVID-19 pandemic changed everything for surgical care around the globe. At the onset of the pandemic, with patient and provider safety at the forefront of our work, Smile Train advised partners to follow the recommendations of the World Health Organization, the Centers for Disease Control, and their local government officials. We monitored, and continue to monitor, our regions across the world on a daily basis.
Our teams have adapted quickly and resourcefully to constantly changing conditions. Even during the height of the pandemic, our work did not stop. We are continuing to support our international teams based on their unique needs, and many of our local medical partners are still on the ground acting as invaluable resources to their communities, particularly in vulnerable countries where access to healthcare remains a challenge. Through telemedicine, our partners have been able to continue providing care, advising families on nutrition, offering virtual speech services, providing counseling for families on how to take care of newborns with clefts, and generally just being a source of medical guidance in a very challenging time.
READ MORE: MORE CLEFT LIP SURGERIES AT AGE 8 TO 10 YEARS TIED TO LATER ANXIETY
Now that surgeries are slowly resuming, the challenge is how to ensure that providers and patients stay safe. Smile Train has invested more than $1M in the distribution of personal protective equipment, handwashing facilities and masks for partners and patients, and essential equipment to empower partners to continue cleft care while protecting themselves and their patients against COVID-19, such as pulse oximeters and non-contact infrared thermometers. Where testing is available, Smile Train is supporting our local partners with grants that will aid in the testing of patients before they undergo surgery.
We are working to share the guidance and equipment our partners need to keep themselves and their patients safe. At Texas Children’s, we remain focused on providing the safest environment possible for our patients, families, and providers amid COVID-19.
Tonya Johnson is associate editor of Plastic Surgery Practice.