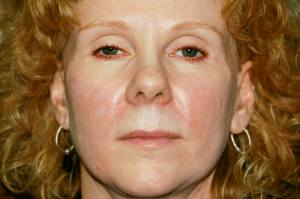
Female patient prior to receiving two syringes of Juvéderm. Note the slightly sagging jawline.”
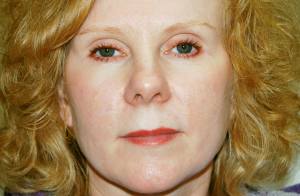
The treatment makes a big difference in her temple area after injecting a little Juvéderm under her eye, a little in the upper lip, and in the nasolabials.
With the current boom in noninvasive and minimally invasive cosmetic procedures, many practitioners are learning to use dermal fillers. Novice practitioners will commonly focus more on the lines or “simple-appearing” problem areas in which the patient desires improvement. This common mistake can lead to a less-than-desirable result and unhappy patient if the “problem” isn’t properly addressed.
In this article, I will discuss the following three issues:
- How to determine the “problem behind the problem” (namely, the true cause of the problem the patient wants improved) by assessing facial anatomy and anatomical proportions;
- How to use this information in your attempt to revolumize the face; and,
- How to incorporate fillers when you plan a cosmetic laser procedure.
DETERMINE THE PROBLEM BEHIND THE PROBLEM
This is the first and most important step in a dermal filler procedure. For example, a patient may complain of heavy nasolabial folds, and the novice practitioner may only inject that area. In this situation, the practitioner might not see that the problem is actually an age-related fall of the cheeks in an anteromedial direction—the patient has begun to lose the upside-down triangle of youth. Patients in their 20s and 30s usually have high voluminous cheeks that peek just inferolateral to the lateral canthal folds. As one ages, one typically loses cheek height and volume. The face will also lose bone density, which will in turn affect the appearance of the cheek.
With age, a patient’s upside-down and proportional triangle of the cheeks to the chin will start to square off. This can lead to a heavy mid- to lower face that eventually will be beyond correction without invasive surgery.
Therefore, in this example, the cheeks (and likely the tear trough and temple) need to be augmented with filler before even injecting the nasolabial folds. This will lift the cheek and somewhat take the heavy pressure off of the nasolabial fold. Less filler is usually required in the nasolabial folds with this technique. If you inject only the nasolabial fold, undercorrection often occurs because the cheek is still “heavy.”
Become familiar with the Phi proportions of the face. Although detailed information about Phi proportions is beyond the scope of this article, these measurable proportions will allow you to determine the cause of problems, as well as where certain parts of the face need to be augmented to give it a more youthful look.
Obviously, another very important part of a filler procedure is to set reasonable expectations for your patient. If someone comes for a consult in my office and gives me the “surgery sign” by using their hands to pull their face back toward their ears, they may not be a good candidate for dermal fillers or even cosmetic laser procedures. I commonly turn down patients for dermal fillers because what they really want is a surgical result.
Regardless of the chief complaint or requested procedure, my patients receive a full consult discussing injectables, laser procedures, and surgery before I perform any treatment. Hence, I very rarely take on a patient who does not obtain the desired result. On the other hand, we all have had that type of patient who is unrealistic and never satisfied no matter what we do.
THE BEST MEASUREMENTS

After resurfacing and Juvéderm injection of the nasolabial folds and cheeks (the patient is not wearing any makeup).

Female patient prior to CO2 facial resurfacing.
Using the Phi proportions of the face, you can determine where each part of the face “should be located” in a youthful-appearing face. Measurements are used to determine brow height and length, height of the radix of the nose (filler can be used to soften the “nose hump”), peek of the cheek, size and shape of the lip, lip and chin length on lateral profile, and other features. You can actually purchase a Phi caliper when learning these measurements, but you will likely be able to mentally measure these areas with experience. I will briefly describe the use of these measurements in three areas: the cheek, the nose, and the lips.
Four Phi measurements can be used to determine where the peak of the cheek should be:
- A line from the lateral canthal fold to the oral commissure (medial border of the cheek);
- A line from the oral commissure to the mid tragus (posterior border);
- A line from the lateral edge of the brow through the lateral canthal fold, toward the jawline; and,
- A line from two-thirds down the nose to the upper tragus of the ear.
The area that is centrally created (in the middle of the lines) is where the cheek prominence should peak. Typically, this is lateral and slightly inferior to the later canthal folds, and a small amount of filler—not usually more than 1/2 to 3/4 cc—can make a very nice difference. This will then take the pressure off the nasolabial folds and help to recreate the upside-down facial triangle, which gives the face a more youthful look. Patients will commonly worry about looking “fat” in their face, but, if performed correctly, this will not be an issue. My patients are typically amazed at the improvement achieved with this technique.
Regarding the nose, if a patient has a bony or cartilage prominence in the middle of the nose, then they will not have an even slope of the nose. The beginning of that slope on lateral profile view will be to low/anterior. The beginning of the slope of the nose (radix) should, by Phi proportions, begin where the upper eyelash appears in lateral profile view. A very small amount of hyaluronic acid filler (usually only about 1/8 cc) will move the start of the slope higher and soften the nasal hump.
Again, patients will be concerned that the nose will look bigger, but it will actually help to make the nose look smaller because youthful proportions have been somewhat restored. This really provides an amazing result, and patients are surprised how much a little filler helps. You must be very careful to avoid vascular compromise and skin/tip necrosis. I do not use lidocaine or epinephrine to anesthetize the nasal area, and I am very careful to inject anterograde, which will decrease the risk of intravascular injection.
Knock on wood—I have never had a complication with this technique in almost 4 years of experience. Nitro paste and aspirin will help if you do see postprocedure blanching of the skin, although it is rare to ever have to use this.
DON’T GIVE THEM TOO MUCH LIP
My third example discusses lip augmentation, a procedure that many patients worry about for various reasons, or have experienced a poor treatment elsewhere. For example, patients are often afraid of having “duck lips” because of what they have heard, seen, or even unfortunately experienced.
In assessing the lips, you must realize that with age the upper lip appears to fade in volume quicker than the lower lip. However, this is often not due or not only due to volume loss. In time, the upper lip starts to roll or invert from lateral to medial. Thus, patients usually see smaller later lip margins before the medial lip fades. This patient will commonly have enough volume in the pulp of the lip and just needs more “show” of the lip pulp.
To accomplish a proper augmentation in this patient, you should inject a small amount of hyaluronic acid filler in the vermilion border to achieve eversion of the upper lip and more show of the lip volume. This will provide a nice visual augmentation without turning the lip into a rubber tire.
In addition, although filling the lip for the purpose of decreasing lines on the lip itself and the philtrum can be done well, you should not inject so much filler as to completely take away lip pulp lines, which will give an overvolumized look.
If the patient really has lost volume (or simply wants much bigger lips), then injection of the filler can be added to the pulp of the lip. You must know the filler well enough so as to not over- or undercorrect the volume. I am always very conservative with the amount of filler I inject. This allows me to learn how the individual patient’s tissue reacts to the filler, as more can always be injected.
An underfilled patient can be refilled, but an overfilled patient will no longer be your patient. Remember, the cosmetic physician’s motto should always include that the enemy of good is better.
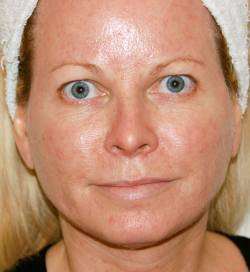
Female patient prior to fractional CO2 facial resurfacing, and liquid facelift with Juvéderm.

Post-treatment. Note the augmentation of the temple, cheeks, tear trough, nasolabial folds, marionette lines, upper lip, oral commissure, and jawline.
WATCH FOR THE GOTCHA
There are a number of pitfalls—leading to unhappy patients—to be aware of and avoid when injecting dermal fillers. It is most important to know the anatomy and anatomical proportions as previously described, so you inject the proper area and not just the area the patient requests to be injected. Dermal filler procedures are commonly thought of as a simple matter of knowing how to use a needle and syringe, but there is obviously a lot more to it.
You must also be extremely familiar with each product and understand its properties, including the type of product; how it fills (by volume of the actual filler, by absorption, by inflammatory reaction, etc); where it should be used; and what are the associated benefits, risks, complications, and contraindications. Too much filler or filler in the wrong area will cause many more problems than underfilling (when more can always be injected later).
However, you do not want to underfill an area and have an unhappy patient in the following situations. If a patient really needs surgery or another procedure, do not let them convince you to “try this first to see if it works.” It won’t. Setting patient expectations and full consult/consent are often overlooked if you are more concerned about not turning down a paying patient.
In addition, if the patient really needs multiple areas injected and/or multiple syringes to improve the issue, he or she will certainly not be happy if undertreated. Never fall for the common patient request, “Try to see if one syringe is enough, then I will do more.” This approach will underfill and undertreat the patient, they will not be happy, and they will certainly not want to spend money on another syringe if the first one “didn’t work.”
One final training tip concerns timing of dermal filler injections when planning cosmetic laser procedures in the same area. The procedure to be done first is always the one that produces the most long-lasting, “skin-changing” results before the less aggressive, simpler, and temporary procedures are performed.
If the patient has surgery scheduled in the relatively near future, that procedure should always be done first over laser and injectable procedures. Cosmetic laser procedures should come later. For example, if you use a fractionated laser (ablative, fractional, or nonablative) to resurface and tighten/smooth the skin, a dermal filler can be used to further augment areas of tissue and volume loss. I will typically wait at least a month after a laser procedure to inject filler.
Depending on the type and depth of laser treatment and the filler to be used, you must be very careful about performing a laser treatment after a filler treatment. Ideally, you will know that a surgery or laser procedure is to be done first, unless the patient receives filler first and then decides he or she really wants to do another procedure.
Typically, I wait a few months after a hyaluronic acid filler procedure to perform moderate or aggressive laser resurfacing. I wait even longer if someone else did the filler. You never know where the filler was placed and for sure what type of filler was used. Be cautious treating someone having recently received a cosmetic procedure from another practitioner.
A WORD ABOUT RF AND LASERS
Although previously I was not a proponent of early radiofrequency (RF) technology for skin tightening, recent improvements in this technology are now utilized in my practice on select patients as part of their facial-tightening regimen.
A very thorough consult and consent is necessary to assess and meet patient expectations. In addition, when utilizing cosmetic lasers you must be aware of the limits of each procedure in producing results. Keep in mind the phrase “jack of all trades and master of none”—or, if all you have is a hammer, then everything looks like a nail.
Laser procedures, if performed correctly on good candidates, can significantly expand your practice and help you offer more options to help patients. However, unfortunately, not all practitioners obtain proper understanding of laser theory and physics, know which laser to use for each condition, and even know how to actually perform the procedures properly.
CONCLUSION
Dermal fillers can be a wonderful part of a patient’s treatment plan. You must know the type of product, how it works, how and where to inject, and what to expect regarding results. You can add these procedures to a regimen that includes surgery and cosmetic laser procedures if you know how to properly order the procedures and which are best for the patient.
Experience is key, but you have to obtain experience somehow. So, my best advice is to completely learn all of the things I have discussed and conservatively treat to gain experience.
Warren B. Seiler III, MD, is a cosmetic surgeon in private practice in Birmingham, Ala. He can be reached at (205) 870-0204.