According to the American Society of Plastic Surgeons (ASPS) report of the 2010 statistics, liposuction is one of the top five cosmetic procedures, following breast augmentation, nose reshaping, and eyelid surgery.1 From 2009 to 2010, liposuction procedures increased 2% among the 13.1 million cosmetic procedures performed in the United States.
It is not surprising, therefore, the huge demand for fat removal among plastic surgery patients. There is increasing public and medical awareness regarding excess body fat as a cause of health problems and dissatisfaction with body shape. More frequently, people seek procedures with excellent outcomes and less recovery time, downtime, pain, and complications. Recent advances in the technology of fat removal has allowed for safer and more effective procedures, with the ability for body contouring or shaping in ways never anticipated.
Historically, fat removal was achieved through surgical resection of fat and the overlying skin or curettage through small incisions, which led to poor outcomes and many complications.2 Later, with anticipation of fewer complications and better results, blunt-tipped instruments were developed for tunneling through fat. These were powered and contained internal blades to break up aspirated fat to facilitate its removal.3,4
At this time, general anesthesia was required, putting the patient at increased risk of complications and made postprocedure assessments quite difficult. The patient was unable to turn on the operating table without requiring major assistance, and could not be placed in a standing position at the end of the procedure to assess the effects of gravity on the reposition of fat after aspiration.
It seems the early concepts of liposuction may have been solely on fat removal, to determine the best way to rid the body of larger volumes of excess adiposity without major distress over patient comfort, physician fatigue, or contouring. By contrast, the latter characteristics appear to be of significant importance at the present time.
HOW THEY DID IT THEN
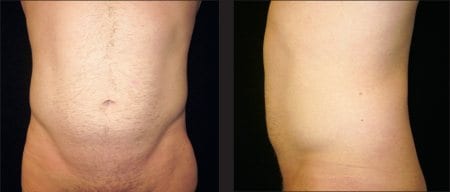
Figure 1. Front view (left) and left side view (right) of a 32-year-old male at consultation who requested a defining liposuction procedure. The patient has stubborn areas of adiposity of the abdomen and flanks that he has been unable to rid with pristine diet and exercise.
The standard method of traditional liposuction was to use large, blunt-tipped cannulas with one or two distal apertures, to ensure that a large negative pressure was generated between the subcutaneous tissue and the powered suction device in order to plainly “suction” out large volumes of fat.5
Although success was achieved and fat removal was accomplished, complications such as ecchymosis, seroma, and permanent irregularities occurred in many cases. It wasn’t until the late 1970s, when the “wet and super-wet techniques,” which implemented infiltration of various fluid cocktails of saline with substances such as hyaluronidase or epinephrine, helped to facilitate fat removal with reduced blood loss, pain, and irregularities.6
In the 1980s, the tumescent technique introduced by Jeffrey Klein, MD, allowed for large volumes of saline containing 1:100,000 epinephrine (“wet technique”) and specific concentrations of lidocaine (anesthetic) to be used in order to prepare the fat and aid in aspiration.7,8 The tumescent technique almost guarantees an easy and quality aspirate with reduced blood loss and minor associated risk.
Although lidocaine toxicity, pulmonary edema, pulmonary embolism, and necrotizing fasciitis have been reported as complications, the postoperative recovery period and pain are much less with the tumescent technique as compared with traditional dry methods.
It was never anticipated the degree to which this technique revolutionized the fields of plastic surgery and dermatology by allowing this surgical procedure to become an outpatient procedure with minimal downtime and many future applications.
As the demand for liposuction has increased, manufacturers and surgeons have sought differing cannula designs and diameter, infiltration methods, and suction techniques, anticipating increased quality of the result rather than simply focusing on the procedure itself. The most prominent scientific advances have been the use and improvement in tumescent anesthesia, smaller cannula sizes and shapes for use in specific body areas, power (vibration) and energy technologies, and the use of manual syringe suction for fine contouring and autologous fat transfer.
Despite these many advances, short-term complications, including postoperative edema, ecchymosis, pain, hyperesthesia, paresthesias, hematoma, and seroma formation, are a reality. However, typically they resolve without sequela. The advent of power- and energy-assisted liposuction devices has decreased postoperative pain and increased patient comfort during the procedure.9
Surgeon fatigue has decreased dramatically as procedures became more quick and precise. Newer technologies have shown the most benefit in areas of firm fat (such as the breast or flank), in areas of prior surgery, or in areas where smoother contours or definition is wanted.10,11 Contour irregularities are still difficult to avoid and correlate with the level of surgical experience and techniques used.
BODY SCULPTURE
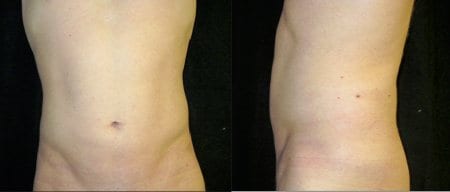
Figure 2. Front view (left) and left side view (right) of the same 32-year-old male patient 2 months after a high-definition procedure involving both the deep and superficial fat of the abdomen and flanks. Note the minimal volume reduction but significant improvement in body contours.
Traditionally, fat removal has focused on techniques that facilitate removal while limiting complications and patient dissatisfaction, but sometimes fail to achieve the aesthetic goal of creating harmonious body contours and/or muscular detail. A trend in the modern era of liposuction is the idea of “sculpting” or “etching,” which takes into consideration the body’s natural contours and the concept of what exemplifies an attractive body shape.12
Rather than focusing on localized areas of excess fat, the surgeon must now have an artistic approach to the concept of fat removal. Adequate patient results now require a surgeon with a more precise knowledge of the surface anatomy, the underlying musculature or bony architecture, and their connection to body shapes or silhouettes. As opposed to simply using large cannulas that create large tunnels for fat removal with a subsequent decrease in body size, the trend is for the modern lipo-surgeon to use differing techniques to highlight a patient’s natural features. Many times, this may require only a small volume of aspirate requiring differing cannula sizes and shapes and/or newer technologies, such as power-, ultrasound-, and laser-assisted devices.
The sculpting method requires the understanding of the structural organization of fat as both a superficial and deep layer with distinct properties and functions.13 In general, superficial lipoplasty with standard liposuction cannulas has been called out, as it has been associated with an increased risk of scarring, contour irregularities, and cutis marmorata when excessive fat removal is performed. Also, while the newer devices are advocated as complements to traditional liposuction and may be helpful in more fibrous areas, secondary liposuction cases, and where superficial liposuction is wanted, side effects such as ulceration, burns, and postinflammatory hyperpigmentation are a possible consequence.14
Nonetheless, newer technologies hold promise in detailed or “defining” cases where contouring or shaping is requested. Many practitioners support laser-assisted devices for skin tightening when used at shallow levels beneath the dermis, although the jury is out as to whether or not these claims are proven advantages over traditional liposuction.15,16
Nevertheless, in only a short time performing fat-removal procedures, I recognize a trend toward fine aesthetic aspiration of fat, requiring the surgeon to be an artist who balances the quality of creating an aesthetically pleasing body form with patient safety—rather than simply performing a volume-reducing procedure.
Patients who primarily request these procedures are focused on changing their body shape with contouring, particularly in the abdominals, arms, legs, thighs, and gluteal areas. These patients diet and exercise, but still have fat (usually love handles or saddlebags) that is resistant to activity (Figure 1).
The ideal candidate for a contouring procedure should be near ideal body weight and have isolated focal areas of fatty deposits, as well as be motivated by the procedure to continue or improve their nutrition and exercise regimens when healed.
LIPOSCULPTING
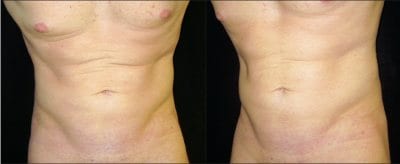
Figure 3. Front view, bending (left) and left side view, bending (right) of the same 32-year-old male patient 2 months postprocedure, demonstrating significant improvement in body contours and muscular definition. The costal margins, semilunar lines, linear alba, and anterior iliac spines are more pronounced. Definition of these areas was requested by the patient at consultation.
Liposculpting is technically more difficult and requires both deep and superficial infiltration of tumescent fluid followed by cannula aspiration. Many advocates of “abdominal etching” or liposuction for muscular enhancement use laser- or ultrasound-assisted techniques as a secondary step to debulk and emulsify prior to aspiration.17
Energy is distributed in the two layers of fat. Cumulative energy is dependent on the body location.18 In more delicate areas—such as under the neck, underarms, in the inguinal folds, and inner thigh—lower energies are carefully distributed to prevent against scarring, burns, necrosis, or postinflammatory hyperpigmentation.
Higher energies can be used in areas with greater deep fat, such as the abdomen, love handles, and outer thighs. Although the assisted liposuction techniques are less fatiguing, contouring or sculpting procedures are often more time-consuming and, therefore, can be more exhausting to the surgeon.
The risk of contour irregularities—such as wrinkling and rippling, skin tone changes such as cutis marmorata, and paresthesias or permanent nerve damage—are much higher when subdermal fat is removed. However, proper technique and training will help minimize the risk.
Traditional methods with solely deep fat aspiration and a wet technique will not accomplish the aesthetic goals requested by our modern patients. Since the standards of beauty are much higher than seen previously, we are seeing a trend of patients who we may have never previously considered for body contouring and can now offer results that were previously unattainable or nearly impossible due to strenuous diet and exercise requirements (Figure 2).
ENERGY-BASED DEVICES
Thus far, only one study has looked at high-definition liposculpture to improve body contour or to define underlying anatomy.19 A total of 306 patients were treated by two plastic surgeons with vibration amplification of sound energy at resonance (VASER) technology with deep and superficial infiltration, emulsification, debulking, and cannula extraction. Excellent results were documented by both surgeons, with consistent results showing high muscular definition in both males and females of the rectus abdominus, obliques, and pectoralis. Every patient had successful waist contouring, as well. Overall, there were no serious complications, but 20 cases of seroma, nine cases of port site burns, and five cases of prolonged swelling were reported. There were no cases of skin necrosis.
Of importance, the authors used a technique called “transitioning,” defined as the blending of the topography of the muscles to help improve the definition of the superficial anatomical landmarks and create a natural, but well-defined appearance. This was achieved via cannula extraction of fat. Overall, the surgical end point was a retained thin layer of fat at the lateral borders of each anatomical unit (1 cm in a pinch test). In some instances, a more aggressive approach may be needed where “shadowing” or sculpting is requested, such as the iliac spine, lower pubis, lateral flank, and rib margins. In these areas, less than a pinch test (< 1 cm) may be required for sculpted results, but can predispose to complications.
Some advocate the use of newer technologies such as laser- or ultrasound-assisted devices for defining procedures.20,21 Devices with multiple wavelengths, such as the SmartLipo Triplex™, from Cynosure Inc, Westford, Mass, contain three wavelengths (1064 nm, 1320 nm, and 1440 nm) to effectively damage unwanted subcutaneous fat and cause tissue coagulation for a tightening effect. These controlled energies can be used to initially treat the deeper levels of fat for emulsification, to allow for easier power-assisted removal, then followed by subdermal treatment to enhance skin retraction and contraction.
Previously, subdermal treatment with cannula extraction predisposed to rippling or irregular contours. However, laser-assisted techniques are able to deliver controlled energies that homogenously treat fat cells and may decrease instances of irregularities. However, energy-based devices can predispose to other complications, such as burns, scars, and postinflammatory hyperpigmentation. Nevertheless, newer technologies are available and seem promising for surgeons to use on these requested procedures.
In another review of people treated for moderate collection of adiposity and mild to moderate degrees of skin laxity, 75 patients were treated with dual-plane laser lipolysis (1064 nm/1320 nm) and demonstrated high rates of patient satisfaction, especially in areas of skin laxity such as the face and/or neck, brachium, abdomen, and thigh.22 Patients observed about 80% clinical improvement in 2 to 3 months with a very low incidence of side effects. Approximately 5% of patients developed nodularity within 6 weeks after surgery, mostly in the upper abdomen and periumbilical sites. Irregularities were successfully treated with ultrasound treatments. There were no instances of seroma formation, hematomas, dyschromias, scarring, permanent nerve injuries, perforation, or fracturing at the fiber tips.
The authors related a low incidence of side effects to continuous monitoring of deep, shallow, and surface skin temperatures, along with constant palpation to determine the correct surgical planes during the procedure. Further, the authors concluded that the use of multiple wavelengths specifically targeting individual structures by selective photothermolysis helped to provide controlled laser energies and possibly provided an advantage of tissue tightness and coagulation.
THE BOTTOM LINE
As with any new technology and trends, high rates of skepticism and conservatism should be maintained. The newer technologies for fat removal, such as energy-assisted and laser-based devices, appear to provide quicker recoveries, less surgical fatigue with decreased surgical time, possible skin contraction and tissue tightening, and the ability for superficial capabilities to allow sculpting or “defining” procedures.
Excellent results have been reported, especially in areas that are small and compact, areas that require superficial treatment, and in sites of previous treatment or irregularities from conventional liposuction. When removing fat above the deep layer, collateral injury to nerves and vessels as well as contour deformities are serious considerations. These complications should be circumvented as best as possible.
Questions remain. Will newer technologies replace traditional liposuction? Will patients increasingly request sculpted or body sculpting procedures for refinement in body contours, rather than solely removing fat as a volume-reduction procedure? As the image of beauty continues to change, surgeons will need to enhance their techniques and heighten their awareness to the desires of their patients, and balance this against the surgical risks and benefits.
Time will tell, but we appear to be headed toward embracing an expanding repertoire of fat-removal technologies to keep up with the social trend.
Jason J. Emer, MD, is a resident dermatologist at the Department of Dermatology at the Mount Sinai School of Medicine. He is currently involved in numerous medical and cosmetic clinical trials, as well as head of the resident education in cosmetic training in his residency program. His special areas include complicated medical dermatology (including the use of immunosuppressants in inflammatory and autoimmune conditions), cosmetic dermatology of aging skin with lasers, and body sculpting procedures. He can be reached at (212) 659-9530 or .
References
- American Society of Plastic Surgeons. 2010 Quick Facts: Cosmetic Plastic Surgery Demographic Trends. Available at: www.plasticsurgery.org/Documents/news-resources/statistics/2010-statisticss/Top-Level/2010-Fullquickfacts-cosmetic-surgery-minimally-invasive-statistic-demographics.pdf. Accessed September 6, 2011.
- Katz BE, Maiwald DC. Power liposuction. Dermatol Clin. 2005;23(3):383-91, v. Review.
- Coleman WP III. The history of liposuction and fat transplantation in America. Dermatol Clin. 1999;17(4):723-727.
- Flynn TC, Coleman WP II, Field LM, Klein JA, Hanke CW. History of liposuction. Dermatol Surg. 2000;26(6):515-520.
- Illouz YG. Body contouring by lipolysis: a 5-year experience with over 3000 cases. Plast Reconstr Surg. 1983;72(5):591-597.
- Sattler G. Advances in liposuction and fat transfer. Dermatol Nurs. 2005;17(2):133-139.
- Klein JA. Tumescent technique for regional anesthesia permits lidocaine doses of 35 mg/kg for liposuction. J Dermatol Surg Oncol. 1990;16(3):248-263. Review.
- Klein JA. Tumescent technique for local anesthesia improves safety in large-volume liposuction. Plast Reconstr Surg. 1993;92(6):1085-1098; discussion 1099-1000.
- Palm MD, Goldman MP. Laser lipolysis: current practices. Semin Cutan Med Surg. 2009;28(4):212-219.
- de Souza Pinto EB, Abdala PC, Maciel CM, dos Santos Fde P, de Souza RP. Liposuction and VASER. Clin Plast Surg. 2006;33(1):107-115, vii.
- Mann MW, Palm MD, Sengelmann RD. New advances in liposuction technology. Semin Cutan Med Surg. 2008;27(1):72-82. Review.
- Hoyos AE, Millard JA. VASER-assisted high-definition liposculpture. Aesthet Surg J. 2007 Nov-Dec;27(6):594-604.
- Mordon S, Plot E. Laser lipolysis versus traditional liposuction for fat removal. Expert Rev Med Devices. 2009;6(6):677-688.
- Katz B, McBean J. Laser-assisted lipolysis: a report on complications. J Cosmet Laser Ther. 2008;10(4):231-233.
- Parlette EC, Kaminer ME. Laser-assisted liposuction: here’s the skinny. Semin Cutan Med Surg. 2008;27(4):259-263.
- McBean JC, Katz BE. A pilot study of the efficacy of a 1,064 and 1,320 nm sequentially firing Nd:YAG laser device for lipolysis and skin tightening. Lasers Surg Med. 2009;41(10):779-784.
- Katz B, McBean J, Cheung JS. The new laser liposuction for men. Dermatol Ther. 2007;20(6):448-451.
- Mordon S, Plot E. Laser lipolysis versus traditional liposuction for fat removal. Expert Rev Med Devices. 2009;6(6):677-688.
- Hoyos AE, Millard JA. VASER-assisted high-definition liposculpture. Aesthet Surg J. 2007;27(6):594-604.
- Woodhall KE, Saluja R, Khoury J, Goldman MP. A comparison of three separate clinical studies evaluating the safety and efficacy of laser-assisted lipolysis using 1,064, 1,320 nm, and a combined 1,064/1,320 nm multiplex device. Lasers Surg Med. 2009;41(10):774-778.
- Sadick NS. Overview of ultrasound-assisted liposuction, and body contouring with cellulite reduction. Semin Cutan Med Surg. 2009;28(4):250-256.
- Sasaki GH, Tevez A. Laser-assisted liposuction for facial and body contouring and tissue tightening: a 2-year experience with 75 consecutive patients. Semin Cutan Med Surg. 2009;28(4):226-235.



