Adult Stem Cells–A Coming Revolution?
Research on adult stem cells is generating an increasing amount of attention these days. Scientists have found adult stem cells in many more types of tissues than they once thought possible. Certain adult stem cells have the ability to differentiate into several cell types, given the right conditions. If differentiation of adult stem cells can be controlled in the laboratory, these cells may become the basis of therapies for many serious injuries and diseases.
Jeremy Mao, DDS, PhD, associate professor of dental medicine at Columbia University Medical Center (New York City), and his colleagues have received a $2.5 million grant from the National Institute of Biomedical Imaging and Bioengineering (in the National Institutes of Health) to use stem cells to engineer soft tissue and develop a process that may ultimately allow scientists to use a patient’s own stem cells to generate tissue for facial reconstruction following disfigurement from war, cancer surgery, or accidents.
“Stem cells may be of benefit in facial reconstruction by either triggering damaged tissue to repair itself or by actually differentiating into the likeness of the tissue that needs to be regenerated,” says Gary Motykie, MD, a plastic surgeon in Los Angeles. “It is consistently observed that transplanted fat does not feel like isolated collections of fat but rather more like the recipient-site tissue into which it has been transplanted.”
Currently, surgeons graft from the patient’s own tissue, which creates additional wounds. Grafted cells also fail to stay alive, causing implants to shrink up to 70% and lose their volume. Attempts have been made to use fat cells left over after liposuction, but those cells have a limited life span, according to Mao.
In the study, Mao and his team showed that human adult stem cells can create long-lasting implants in mice. The implant is created by placing the stem cells into an FDA-approved scaffold that mimics the conditions needed to turn stem cells into fat cells. Because stem cells have the ability to replicate, they can regenerate the soft tissue, keeping the implant from shrinking. In mice, these cells have successfully created fat cells that could be implanted, and they retained their size and shape for at least 1 month.
“Although their true role in tissue regeneration still needs to be further studied, the role of stem cells in facial reconstruction may involve them being injected alone or integrated into facial porous implants,” Motykie says.
According to Mao, the implants can be molded and therefore may also be used for breast reconstruction—a potentially safer alternative to silicone or saline implants that can rupture and interfere with the detection of recurring cancer.
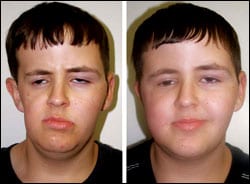 |
| This 16-year-old was diagnosed with a rhabdomyosarcoma of the right orbit in infancy and received radiation therapy, which severely affected his right-side facial growth. He was treated with 100 mL of fat, which was harvested from his abdomen and injected in his face. The patient is shown 1 month after the procedure and, although the clinical result is excellent, at 6 months about 50% of the fat was resorbed and the patient was retreated. |
Fat In, Fat Out
Researchers at Georgetown University Medical Center (Washington, DC) report that they may have discovered a natural way to fill in crows’ feet and get rid of unwanted fat in the thigh and abdominal areas by injecting neuropeptide Y (NPY), a chemical that is found in the body. They also report that blocking the NPY receptor (Y2R) can prevent the development of fat, which can revolutionize plastic surgery and the treatment of diseases that are associated with obesity.
“In the case of the neuropeptide Y blocker, having the ability to safely and predictably target and eliminate adipose deposits would be the ‘smart bomb’ of cosmetic surgery,” says Joseph P. Niamtu III, DMD, a cosmetic surgeon in Richmond, Va. “The implications of these are amazing and could possibly take the literally mechanical mechanism of liposuction out of the equation—which sounds too good to be true.”
According to Niamtu, the bane of aesthetics and reconstructive surgery is that there always seems to be too much or too little fat, and usually the opposite of what you want or need. The ability to create fat in the face and neck may solve the aesthetic filler situation as a truly natural, autogenous, permanent facial filler. Most patients would opt for their own tissue if it were a permanent solution and if it were predictable.
In the study, researchers led by Zofia Zukowska, MD, PhD, professor and chair of the department pf physiology and biophysics at Georgetown University, injected NPY into a specific area of the body of laboratory mice. They found that NPY and Y2R are activated during stress, leading to apple–shape obesity and metabolic syndrome. The weight gain and metabolic syndrome, however, were prevented by administering Y2R blocker into the abdominal fat.
 |
| See also “Adipose Stem Cells” by Richard Ellenbogen, MD, FACS, FICS, and Gary Motykie, MD, in the December 2006 issue of PSP. |
The researchers report that this is the first study to show that stress has a direct effect on fat accumulation, body weight, and metabolism. Blocking Y2R resulted in local elimination of adipose tissue.
According to Zukowska, the ability to add fat as a graft can be useful for facial rejuvenation, breast surgery, buttock and lip enhancement, and facial reconstruction. Using injections like the ones tested in the study could also make fat grafts predictable, inexpensive, biocompatible, and permanent.
“Like all futuristic ideation, one must temper the dream with reality and first provide evidenced-based proof that this new technology can in fact work safely and predictably,” Niamtu says. “Just to think about it is exciting. Surgeons live in a world of fat in most every discipline, and the ability to control it would change history and medicine.”



