|
The use of intense pulsed light (IPL)—with or without radiofrequency (RF)—for facial rejuvenation has grown rapidly in popularity over the past decade to become the number one light-based skin-rejuvenation procedure performed in the world. It is estimated that, on any given day, 25,000 IPL or IPL–RF photorejuvenation procedures are performed worldwide—10,000 to 15,000 in the United States alone.
Having pioneered and codeveloped the full-face IPL and IPL-RF procedures, I have had the pleasure, through teaching workshops to more than 5,000 physician attendees, to witness firsthand the beneficial effect that FotoFacial®—as we call it—can have on the patient and the plastic surgeon’s practice.
Many devices and companies can now deliver full-face, neck, chest, hand, and body photorejuvenation treatments. The common feature of all of the procedures is the use of intense, pulsed, broadband light (BBL). Many companies call this IPL; another name is fluorescent pulsed light. But essentially, all the devices deliver a pulsed flash lamp of some description, with cutoff filters that allow a broad range of wavelengths of light to hit the skin with each pulse—as opposed to monochromatic laser systems that emit only one light wavelength.
Most systems emit light with a spectrum from 470 nm at the lowest to 980 nm at the highest. Some systems and procedures will combine RF either in the same pulse or with a different pass and applicator. Other systems combine noninvasive long-pulsed IR wavelengths (Nd:YAG—near-IR wavelengths greater than 1064 nm—or IR itself).
In general, the pulsed, BBL penetrates relatively superficially (depth is determined by the wavelength, spot size, and amount of energy) and is attracted mainly to vascular and pigment chromophores. If the wavelength of the light and the absorption coefficient of the chromophore at that wavelength are in concert, the photon of light reacts with the chromophore to produce heat, which in turn damages the chromophore target, resulting in its gradual diminishment or resolution.
Thus, the IPL or BBL acts principally to “color correct” the skin, improving red discoloration (rosacea, telangiectasias, flushing, and blushing) and brown discoloration (photodamage, melasma, and dyschromia). It also provides subtle textural improvements in pores, fine lines, and dermal irregularities.
Our FotoFacial treatments are aggressive enough to cause modest damage to the chromophore, but avoid purpura, crusting, and other sequelae of laser treatments and allow the patient to wear makeup and return to work immediately. For the best results, the treatment is performed on the entire face, neck, or chest once every 3 or 4 weeks, and for a total of five times. The program may combine microdermabrasion, skin care products, and even botulinum toxin Type A (BTTA) and soft-tissue fillers at the very end to provide a comprehensive noninvasive outcome.
Depending upon the physician and the device he or she has purchased, IR or RF may be added to each IPL treatment to improve tissue tightening and provide modest lifting effects.
Training Is Essential
It is critical that the physician or the physician’s delegate be well-trained in the operation of the system and the delivery of the procedure. The assessment begins with a thorough history and physical examination, during which time the patient’s problems and concerns, as well as his or her goals and expectations, are defined. If the patient does not have any contraindications and is a facial-photorejuvenation candidate, then informed consent is discussed.
Most photorejuvenation procedures are well-tolerated by patients and are performed with topical anesthetic cream and a topical skin-cooling system in less than 1 hour. Most patients describe the discomfort as minor in nature—a small skin “pinch.”
The patient’s skin type—light versus dark skin—to a great degree determines the amount of energy that can safely be administered; care must be taken not to be too aggressive on dark or tanned skin. Like laser skin treatments, treatment on tanned skin is usually not recommended, especially because tanning ages the skin, which counteracts the desired goal of the photorejuvenation program.
The appropriate photorejuvenation settings vary depending on the system used, the aggressiveness of the treatment plan, and the skin type of the patient. Some clients may express concerns about the effect of pulsed light or lasers on their skin and should be reassured that there are no harmful or carcinogenic effects of pulsed light because all UV light has been filtered out.
Cost can sometime be a barrier to an aesthetic-surgery patient. However, our procedure ranges from $250 to $500 per treatment and is quite affordable for most potential patients. Even when it is combined with BTTA or fillers, it is a fraction of the cost of a facelift.
Building on Photorejuvenation
Implementing a photorejuvenation program in the office of a plastic surgeon, facial plastic surgeon, cosmetic surgeon or dermatologist, or cosmetically oriented physician of any stripe is often the foundation of the comprehensive skin-rejuvenation program. Around the photorejuvenation technology, the astute aesthetic physician will offer microdermabrasion, BTTA, fillers, and skin care.
Many patients will continue to return to the offices of plastic surgeons and facial plastic surgeons for the constellation of noninvasive skin-rejuvenation treatments of the face, neck, and hands that they offer. This population of “noninvasive” patients can offer a nonsurgical stream of income, and the procedures are often delegated to an employee such as an RN, a PA, or an LPN.
While they are in the surgeon’s office, these nonsurgical photorejuvenation patients will be exposed, through intelligent cross-marketing and cross-educational experiences, to internal marketing materials—such as videos, brochures, testimonials, wall prompts, posters, and countertop displays—to the myriad of other noninvasive therapies that are available, and also to the surgical options.
Surgeries such as blepharoplasties, brow lifts, facelifts, and body-contouring surgery, which might have appeared frightening and foreign to the noninvasive-rejuvenation patient, become more acceptable and enticing after the positive experiences of the facial-photorejuvenation and other noninvasive therapies—especially if patients have been exposed to other happy surgery patients during their visits to your office.
The photorejuvenation procedure and its adjunctive therapies act as initial stepping stones for many patients in your practice, who, after good noninvasive experiences and relationship building with your team, become your surgical patients.
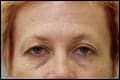 |
| Figure 1. A facial-photorejuvenation patient in her late 40s before any treatments. |
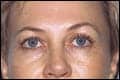 |
| Figure 2. The patient in Figure 1 after 1 year of the FotoFacial program, fillers, and botulinum toxin Type A to the crow’s feet and the frown line. |
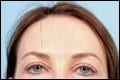 |
| Figure 3. After 7 years, the patient, now in her mid-50s, is shown 10 months after she received upper and lower blepharoplasties. |
A Photorejuvenation Case Study
A woman in her late 40s who was not yet prepared to undergo aesthetic surgery presented with complaints of tired, shallow, discolored, and generally unattractive skin. Her diagnosis was photoaging and dynamic periocular and forehead rhytide deflation, together with some descent (Figure 1). She elected to begin with a FotoFacial treatment program and botulinum toxin Type A (BTTA) to the forehead and the crow’s feet (Figure 2).
The patient was very pleased with the results of her noninvasive photorejuvenation program and began to return four times per year for FotoFacial maintenance treatments, BTTA, and fillers. At the end of 7 years, very happy with noninvasive skin-rejuvenation results, but unhappy with her ongoing descent and cervical laxity and concerns with her upper and lower eyelids, she underwent a four-lid blepharoplasty (Figure 3) and a neck lift—procedures she would never have sought 7 years earlier. The patient has continued her quarterly maintenance regimen following her surgeries.
—RSM
Photorejuvenation After Surgery
For patients who have undergone aesthetic surgery of the face, the photorejuvenation procedure becomes an essential component of postoperative care. Unattractive skin, put into a nice location through surgery, is still unattractive skin in a more youthful location and is often a tell-tale sign of aesthetic surgery.
The skin-photorejuvenation procedure will ensure that you have not only put the skin in the right place, but you have made the skin beautiful after you have put it back where it belongs. By incorporating the photorejuvenation procedure into your aesthetic facial patient’s postoperative experience, you will also be educating the patient about what is required to achieve and maintain beautiful skin and protect their investment.
 |
| See also “Seeing the Light” by Lesley Ranft in the January 2006 issue of PSP. |
Your goal is that every facelift patient will come back to your office three or four times per year for a maintenance photorejuvenation treatment with adjunctive BTTA, and perhaps fillers and skin care. These treatments protect and maintain the surgical results, and are a source of profit to you.
Ultimately, the key to a successful aesthetic practice is patient selection. Well-selected and educated photorejuvenation patients are very happy indeed. These photorejuvenation clients will receive unsolicited comments from friends and family regarding the attractive appearance of their skin. Beautiful skin is one of the most important outcomes a plastic surgeon or cosmetic physician can give a patient, especially one who is initially frightened of surgery. Offering the photorejuvenation procedure keeps these patients in your practice and has quickly become the “cornerstone” of a skin-rejuvenation program.
R. Stephen Mulholland, MD, is a double board-certified plastic surgeon and owner and director of SpaMedica in Toronto. He can be reached at (416) 922-2868 or via his Web site, www.spamedica.com.