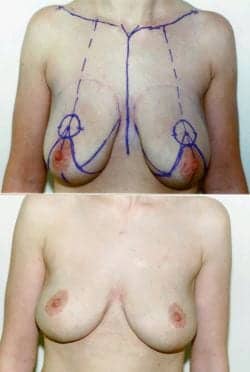
Figure 1. This 33-year-old woman is shown after a loss of 90 pounds due to a Lap-Band procedure; she has been reduced from a 36DD to a 36C.
On a regular basis, women with macromastia present in our office seeking reduction mammoplasty. These patients frequently complain of pain and strain in the neck and back, along with shoulder notching due to the enormous weight of pendulous breasts in a bra. Many also present with secondary complaints of intertriginous rashes and dermatitis along the inframammary folds.
Some teenagers present with severe gigantomastia or severe bilateral breast hypertrophy. We have performed reduction mammoplasty on patients as young as 16.
On a personal level, these women suffer additionally from psychological torment due to crude remarks from tactless boys and men, from an inability to find a bra that contains and supports the entire breast, and from a general lack of apparel that fits both their upper and lower bodies. Many have difficulty sleeping and maintaining a healthy posture while awake.
With the recent popularity of various bariatric procedures, including the Lap-Band device, many women have become Massive Weight Loss (MWL) patients, losing 100, 150, or more pounds and thus requiring surgical body-shaping procedures to remove excess, flapping skin. These MWL patients often present with extreme ptosis—including severe hypertrophy—that typically leaves radically emptied breast envelopes hanging to the umbilicus.
According to statistics compiled by the American Society for Aesthetic Plastic Surgery (ASAPS), 138,152 women and teens1 underwent breast-reduction surgery in 2010, the most recent year for which statistics exist.
In the United States, insurance frequently covers the cost of the procedure, not because of the physical discomfort alone or to gain the cosmetic appeal of more youthful, perky breasts. Insurance is often granted because the excessive weight of oversized mammary glands causes chronic pain and co-morbidities like poor circulation, impaired breathing, and other health woes that would result in costs and fees greater than the cost of a breast-reduction procedure.
THE PATH TO REDUCTION
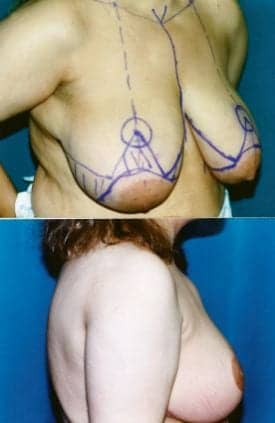
Figure 2. This 43-year-old patient is shown 6 months after breast reduction, at a 40D from a size 40 EE.
Reduction mammoplasty can be considered an intermingling of reconstructive and cosmetic plastic surgery in the purest form. The confluence of the two goals—reduction and a more pleasing shape—not only alleviate the symptoms enormous breasts have upon a woman’s mind and body but also reshapes, molds, and improves the aesthetic appearance of the breasts and creates proportionality in the female form.
Contraindications may include women and teens who hope to breast-feed, women of childbearing age, and dark-skinned women who may develop severe hyperpigmentation of scars or even hypopigmentation of the nipple areolar complex.
According to at least one author, the first breast reduction was performed in 1886 by a physician named Thomas.2 Reduction mammoplasty started being performed on many more patients about 20 years ago, and the number has increased significantly in the last 5 or 6 years.
In my office, patients first give a complete medical history; undergo mammogram screening and/or ultrasounds to determine a baseline image of the breasts prior to surgery; and have a complete physical, including pediatric clearance for teen patients and full sets of labs, including CBC, coag panels, and beta hCGs. I also want to determine if any microcalcification or breast mass is present.
During the presurgical phrase, we not only inform patients of the possible, but rare, complications but give them permission forms to sign more fully explaining the usual, typical, and common complications that can accompany breast reduction.
SEVERAL TECHNIQUES
Bilateral breast reduction can now be performed in a multitude of techniques. In the past, such techniques have included the vertical bipedicle technique first described by McKissock in 1972.2 That procedure reduces the central breast by a vertically oriented bipedical flap, which is necessary to maintain blood supply to the nipple-areolar complex.
The Inverted-T technique can be associated with any pedicle, including the superior vertical bipedicle, central pedicle, inferior pedicle, or central mound technique.

Figure 3. A 16-year-old congenital breast deformity patient is shown 8 weeks after breast-reconstruction surgery. A 140-cc saline breast implant was added to the left breast concurrent with a left breast lift.
Also referred to as the Wise-pattern technique, the inferior pedicle technique is currently the most commonly used in the United States.
The central Mound technique is based on the central chest wall and is not associated with any specific skin boundary, and has no specific directional base.
Skin and glandular tissue along with fat are removed along the medial and lateral portions of the breast as well as superior to the inferior pedicle, in which the medial and lateral flaps are brought to midline while the inferior pedicle is superiorly retro-positioned with the nipple-areolar complex and then inset into its new donor site.
The vertical mammoplasty, usually referred to as the Lejour Technique, can be combined with liposuction of the breast (see Sidebar, page 20).
No inframammary incision is used because this is a vertical lift only, with a scar created around the nipple complex vertically. It is considered a safe procedure.
Generally, enormous gigantomastia breasts may require a breast amputation with a free nipple graft.
Finally, liposuction alone of the breasts may be useful and is becoming an alternative in 2011. I have not offered reduction mammoplasty via suction lipoplasty because the procedure does not address skin laxity or ptosis. Moreover, most patients desire their breasts to be lifted as well as reduced in total volume.
COMPLICATIONS
Complications associated with surgical bilateral reduction mammoplasty and mastopexies can include hematoma, infection, nipple loss, fat necrosis, severe scarring, nipple-areola malposition, under- or over-resection of breast tissue, wound dehiscence, pain, cellulitis, pulmonary embolus, and death.
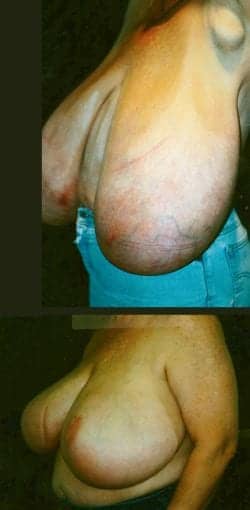
Figure 4. A 40-year-old gigantomastia patient 4 months after breast-reduction surgery (size 48HHH to 46 EE).
Clinically, hematomas are the most common complications of all surgery. In our practice, drains are placed for 24 hours to reduce fluid buildup around the pedicle. Infection may occur along the skin associated with cellulitis and, less likely, as an abscess for deeply seated Staphylococcus aureus, Streptococcus, or Pseudomonas aeruginosa.
Incidents of nipple loss or partial nipple necrosis can be associated with inadequate blood supply through the pedicle. In my practice, we maintain the inferior pedicle 8 to 10 cm to the chest wall to maintain vascularity to the nipple-areolar complex.
Maintaining excellent blood supply through the pedicle is essential. Fat necrosis can be associated most commonly with wound breakdown at the intersection of the inverted T. In addition, maintaining blood supply in this area is vital. Inappropriate wound tension or ischemia can also be associated with fat necrosis.
Removing sutures early in these areas may reduce tension and stress while reducing necrosis size. Hematomas or seromas that are not drained immediately may also increase tension pressure and increase flap and tissue necrosis.
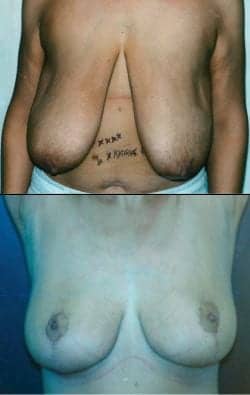
Figure 5. A 39-year-old patient who dropped 120 pounds by gastric bypass surgery is shown 1 year after breast reduction from a 38F to a 38DD.
Drain for 24 hours on all significantly sized breast-reduction procedures. Scarring may be one of the most common long-term results and complications associated with the bilateral reduction mammoplasty. Such scarring can include hypertrophic scarring, keloids, widespread scarring, hyperpigmentation, hypopigmentation, or a variety of the above. Using subcuticular closure sutures and removing sutures within the 13th postop day may reduce scarring significantly.
After sutures are removed, use silicone gel spray twice a day for 3 months to reduce scarring. Injection with Kenalog or other intralesional steroids may also be useful soon after sutures are removed, to prevent hypertrophic and keloid scarring.
Malposition of the nipple-areolar complex may be associated with bottoming out of the breast over time. Normally, you can set the nipple-areolar complex, suturing 5 cm to 5.5 cm from the base at the six o’clock position of the areolar up to the inframammary fold, realizing over time that the nipple-areolar complex will rise and the breast will settle.
Breast amputation with free nipple graft indications can be indicated for patients, including those with severe gigantomastic women who have more than 1,000 grams per breast to be removed. That technique may be useful for patients who are high risk, including those with diabetes, systemic lupus, and rheumatoid arthritis (severe vascular diseases). Other high-risk patients include those who are severely obese, cigarette smokers, or those with systemic medical conditions.
Immediately after surgery, we instruct patients to avoid any water exposure to the breasts, including showering or bathing, for 7 to 10 days.
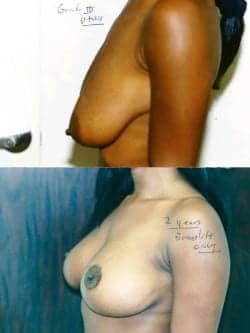
Figure 6. This 31-year-old patient who underwent a breast lift is shown 1 year after surgery. The breast size after lifting is 34D.
BEING PATIENT
I see patients the morning after the procedure when removing the 7-mm or 10-mm JP drains, which had been placed in the lower inframammary fold, when the fluid levels are less than 24 cc and there is no significant portion of blood. Leave drain holes open, remove the Bias dressing, and place a postoperative compression garment—usually a Dr. Linder bra™.
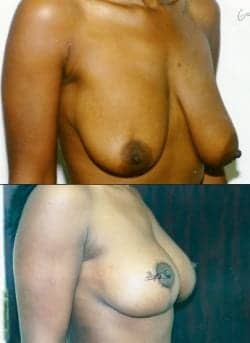
Figure 7. Another view of the patient in Figure 6 at the 2-year postoperative point.
After replacing all the dressings and new 4×4 gauze dressing, we ask the patient to continue ice compression for the next 48 hours in the upper pole of the breast. Refrain from lifting for the next 3 weeks. The bra is left in place until postop day 14, when I change the bra and the dressings, and check for bleeding and/or infections.
In the second week, patients are asked to remove their 4×4 dressings twice daily. Additional checks are done at postoperative day 14 to remove the 5-0 Proline sutures, which were previously run during the procedure in a subcuticular fashion or postoperative day 21 if all the sutures have not been previously removed.
Unless there is evidence of wound dehiscence or significant scabbing, patients are asked to continue with the bra, are cleared to shower, and may return to normal functional activities and exercise routines after 5 or 6 weeks.
Additional checks are then done at 6 weeks, 3 months, and 1 year. Postop/after pictures are taken at 3 months and again at 1 year.
Overall results include a patient-satisfaction rate of more than 90%, obtained through anonymous patient self-assessment reports, and an overall complication rate (mostly infections) of 1/10 of 1%.
Stuart A. Linder, MD, FACS, is a board-certified plastic surgeon, book author, and media commentator on plastic surgery. With offices in Beverly Hills and Las Vegas, he has performed around 14,000 breast procedures since opening his practice in 1998. He can be reached at drlinder.com or (310) 275-4513.
REFERENCES
- www.surgery.org/sites/default/files/Stats2010_1.pdf. Cosmetic Surgery National Data Bank Statistics. 2010. Accessed November 1, 2011.
- McKissock P. Reduction mammaplasty with a vertical dermal flap. Plast Reconstr Surg. 1972;49(3):245-252.
- Spears S. Surgery of the Breast: Principles and Art. 3rd ed. Chicago, Illinois: Lippincott, Williams & Wilkins; 2011.
BREAST REDUCTION BY LIPOSUCTION
In the current economic climate, direct liposuction of the breast without surgical scars and only minimal entry sites for small cannulae is becoming increasingly popular. Performed under IV sedation or general anesthesia, the best candidates are patients with a larger percentage of fatty tissue within the breast and minimal glandular tissue.
Yet, another appropriate use of breast-reduction liposuction is for patients who require shorter times under anesthesia and those who may have systemic diseases, including high blood pressure, diabetes, and asthma, and cannot or should not undergo general anesthesia.
Because liposuction does nothing to address breast ptosis and skin laxity, I have not offered the procedure in my practice. Patients with grade 3 ptosis or more usually do not see a significant improvement of the ptosis.
A lion’s share of our patients request a breast lift along with breast reduction, which requires skin removal along with elevations of the nipple-areolar complex.
However, patients who accept the postoperative skin laxity and ptosis may find the procedure useful for halting neck and back pains typically associated with pendulous breasts.
Moreover, glandular tissue is very difficult to sculpt, as can be seen in gynecomastic male breast tissue. However, actual adipose tissue within the breast sculpts nicely and can be done quite evenly in the majority of cases.
Another indication for liposculpture of the breast includes cases of significant breast asymmetry. Indeed, liposuction breast reduction can allow for sculpting of one breast in order to even it and gain symmetry with the contralateral side.
Another contraindication of breast-reduction liposuction includes patients with gigantomastia or breast hypertrophy associated with the prominence of glandular hypertrophy rather than fatty tissue.
Surgical performance of breast-reduction liposuction usually includes one incision made toward the lateral anterior axillary line, approximately 1 cm above the inframammary fold. The breast(s) then undergo(es) tumescent fluid infiltration followed by liposuction with 4 mm to 6 mm cannulae, depending on the amount of fat to be removed. Multiple authors have shown minimal contour irregularities after breast liposuction when the contouring is done in all directions.
In general, liposculpture of the breast should be more aggressively performed than in other areas, such as the abdomen or thighs. Due to the excellent lymphatic systems of the breast and the axilla, seroma formation in these locations is very, very rare. But provocations of breast-reduction liposuction include a 1% to 2% incidence of hematoma. That can be treated by expressing the blood through the incision site and, secondly, seroma.
Other rare complications may include skin necrosis, infection, and loss of nipple sensitivity. Not surprisingly, the most common complication is under-resection of the breast, because no skin or glandular tissue has been removed.
Studies have indicated a more than 90% satisfaction rate of breast-reduction liposuction patients, with resolution of pain associated with back and neck strain. More than 96% of patients have shown reduced intertriginous rashes with an 88% resolution of grooving along the shoulder blades.
Other studies have indicated that mammograms after liposuction breast reduction do not create calcifications in the breast that could be misinterpreted as breast carcinoma. Those studies also found that scarring from liposuction of the breast did not make it more difficult for one to establish a diagnosis of cancers.
—SL


