|
Acne vulgaris is one of the most frequent dermatological conditions that patients present with, and it affects a vast majority of the population at some stage in their life.1
The pathogenesis of acne is multifactorial and can be associated with four contributors: follicular plugging, excess sebum, inflammation, and the presence of Propionibacterium acnes (P. acnes). Acne characteristically affects the back, upper chest area, and face due to the density of sebaceous glands in these areas.
A treatment plan should first consider the pathological cause of the patient’s acne, as well as the severity. This article highlights the most advanced treatments that address each cause of acne, and discusses how to establish an individually tailored treatment strategy to achieve long-term management of acne. In addition, the latest light- and laser-based therapies will be reviewed, and the efficacy of these options for various lesions will be examined.
COMEDONES AND MICROCOMEDONES
Plugged follicles, commonly known as blocked pores, are often the first recognized manifestation of acne, and they present as either open comedones (blackheads) or closed comedones (whiteheads).
Dead skin and sebaceous materials collect, forming a plug in the opening of the hair follicle. Closed comedones are a result of impacted material that has distended upward toward the follicle opening. An open comedone may form if the follicle opening dilates to accommodate the entrapped material. In addition, cells of the follicle wall can abnormally collect, forming microcomedones that cause further blockage.
Combination topical therapy consisting of an antibiotic, a retinoid, and benzoyl peroxide is a widely used starting regimen that can treat mild acne and comedones.
Prescription topical retinoids function to prevent plug formation in the pores. Antibiotics, such as clindamycin or erythromycin, help to inhibit bacterial growth and decrease inflammation. To avoid eventual bacterial resistance, benzoyl peroxide should be used in conjunction with an antibiotic.2 An effective routine is to apply an antibiotic in the morning and alternate between a retinoid and benzoyl peroxide in the evening.
Adequate cleansing of the pores is an essential step in the long-term management of acne. This can be readily accomplished via medical cleanses when used on a regular basis. A new device that has gained considerable recent clinical use is Clarisonic Pro, a deep-cleansing system that features dual sonic oscillating brushes.3 Many clinicians have started using this device to deep cleanse the skin for office-based procedures.
A modified version of the Clarisonic is also available over the counter, enabling patients to deep cleanse at home prior to application of moisturizer or other products.
As dead skin is one of the main contributors to blocked pores and comedone formation, it is also essential to remove excess dead skin from the affected area.
Microdermabrasion is one procedure that has proven to be beneficial in decreasing surface skin cell debris and unblocking pores. Through a combination of mild abrasion with aluminum oxide crystals and suction, a depth of 10 to 15 microns of the stratum corneum is removed.4
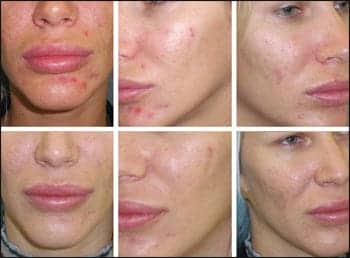 |
| This patient received treatments using a Fraxel laser system, which was used to minimize her active acne and to reduce her acne scarring. At the time these photos were taken, she had only the first of two Fraxel treatments, which showed a marked improvement in her acne after just one treatment. |
The latest devices employ nonabrasive mechanisms, such as cavitated water or vibration. Although studies evaluating the use of microdermabrasion alone for the treatment of acne have demonstrated marginally successful results,5 it has been shown to be beneficial as an adjunctive procedure to laser- and light-based therapy.6,7
Chemical peels serve as excellent keratolytic agents, as they decrease surface skin cell debris and reduce inflammation.8,9 Superficial chemical peeling is indicated for acne treatment, as this lighter peel removes only the stratum corneum and does not damage the dermis.10
Numerous types of agents can be used to perform peels specifically for acne treatment: for example, alpha hydroxyl acids, beta hydroxyl acids, polyhydroxy acids, and Jessner’s solution. Peels are most effective when they are tailored to meet the needs of each patient’s acne severity.
Alpha hydroxyl acids (AHAs)that are most commonly used for acne treatment include glycolic acid and, to a lesser extent, lactic acid. Glycolic acid is used in concentrations of 30% to 70% for chemical peels, with lower concentrations producing the desired superficial peel.
AHAs have demonstrated the best outcomes when several treatments are performed in a series. A study by Kessler et al11 compared alpha and beta peels for acne vulgaris of the face, performed in a sequence of six treatments spaced 2 weeks apart. The use of a 30% concentration of the AHA glycolic acid showed significant improvement by the second treatment, with outcomes improving in each subsequent treatment.11
In the same study, salicylic acid, the primary beta hydroxyl acid (BHA), was also administered at a concentration of 30% in six successive treatments.11 Salicylic acid demonstrated equal efficacy to glycolic acid, but was associated with fewer adverse events than glycolic acid.11
One of the noted advantages of salicylic acid is its strong lipophilicity, which enables rapid penetration of both open and closed comedones.10,12 Due to its lipophilic properties, many practitioners consider it to be the preferred peel for comedonal acne.9,10
An emerging type of chemical peel features polyhydroxy acids (PHAs)—specifically, gluconolactone and lactobionic acid. Studies evaluating PHAs have shown benefits over alpha and beta hydroxyls, including decreased sensory irritation responses and enhancement of the stratum corneum barrier function.13
Last, Jessner’s solution is a combination acid that has extensive use in the removal of comedones and the reduction of inflammation. Used primarily for superficial chemical peels, the solution includes a mixture of resorcinol (14 g), salicylic acid (14 g), 85% lactic acid (14 g), and 95% ethanol (100 mL).10
As is the case with all the superficial chemical peel agents, advantages include only mild stinging and burning during application, as well as a brief recovery time.
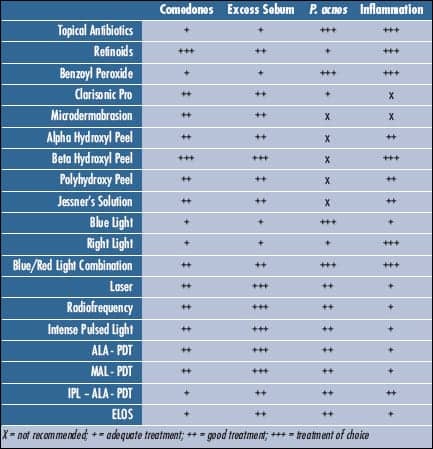 |
| TABLE 1. SUMMARY OF TREATMENT OPTIONS FOR PRIMARY ACNE VULGARIS PATHOGENESIS |
TREATMENT STRATEGIES: EXCESS SEBUM
Patients presenting with both comedones and excess sebum formation are ideal candidates for a series of superficial chemical peels.
Peels serve as an excellent cornerstone for the treatment of mild to moderate acne. For patients who suffer from excess oil production, several novel technologies in addition to peels have demonstrated efficacy in decreasing sebum production and gland size.
These treatments include laser, radiofrequency (RF), intense pulsed light (IPL), and photodynamic therapy (PDT). Similar to chemical peels, laser- and light-based therapies are most effective when several treatments are progressively administered.
Various laser wavelengths have been studied for the treatment of acne vulgaris, including the 532-nm potassium titanyl phosphate laser, the 585-nm pulsed dye laser, the 1320-nm diode laser, the 1450-nm diode laser, and the 1540-nm Er:glass laser.15-17
The 1450-nm diode laser is one of the newest and most effectual tools for explicitly targeting the sebaceous glands. It has shown tremendous success in thermally altering sebaceous glands to decrease their size and to suppress activity.18,19
The 1450-nm laser employs a prelaser cooling phase, followed by a laser phase using a pulse consisting of four bursts of infrared laser irradiation, interspersed with bursts of a cryogen cooling spray.19 The cryogen spray functions to minimize side effects and damage to the epidermis. Several studies have described acne reduction in more than 90% of patients, including a study by Paithankar et al20 in which 93% of treated patients reportedly had no visible acne lesions at 6 months postprocedure.
RF energy is a relatively new modality for the treatment of acne vulgaris. Similar to infrared lasers, RF energy is thought to inhibit sebaceous gland activity in response to RF-produced heat.21 During the procedure, potential damage from heat is offset by a concomitant spray of cryogen to spare the epidermis.21
RF is most commonly used in combination with light therapy for a multifaceted approach, which will be discussed under treatments for inflammation and P. acnes.
IPL varies from the laser modality in that it produces a multiwavelength output of 560 nm to 1,200 nm.22 Instead of targeting one wavelength, as laser-based treatments do, IPL produces thermal injury by targeting a broad range of therapeutic wavelengths.
Delivered in a variable manner, this infrared technology is also especially useful in targeting and controlling the sebaceous glands. Current trends in IPL use for acne treatment involve the combination of IPL with PDT, which has demonstrated greater efficacy than IPL alone.23,24
PDT utilizes a photochemical interaction to target endogenous P. acnes porphyrins, resulting in partial destruction of the sebaceous glands.19,25 Porphyrins are produced by P. acnes during growth and development, and are regarded as a primary instigator in the transformation of a lesion from noninflammatory to inflammatory.25
A topical precursor, such as 5-aminolevulinic acid (ALA) or methyl aminolaevulinate (MAL), is applied prior to administering PDT in order to enhance the photochemical interaction. These precursors selectively accumulate in the sebaceous glands, and are subsequently converted into protoporphyrin IX, a type of porphyrin.26,27 Both the endogenous and converted porphyrins become activated by the application of a PDT light source, resulting in destruction and shrinkage of the sebaceous gland.26,27
P. ACNES AND INFLAMMATION
P. acnes is a naturally occurring bacterium that is present on the skin as well as within pores and sebaceous glands. When dead skin and sebum become trapped and block the pores, P. acnes rapidly multiply, causing follicle damage and inflammation. Once inflammation develops, the degree of acne evolves, forming papules, pustules, nodules, and cysts.28
Early and prophylactic treatment to prevent the overgrowth of P. acnes is critical to the overall success of acne management. As discussed above, topical antibiotics should be used as a first-line defense to prevent bacteria from flourishing. However, bacterial resistance in antibiotic therapy is extensively documented.2,29
The other component of this initial method is simultaneous treatment for inflammation with a systemic retinoid, which has an unfavorable side-effect profile and often leads to patient compliancy issues.
Inadequate response and regimen failure to this traditional treatment approach has led to the development of several novel, alternative therapies to eradicate persistent acne-causing bacteria and inflammation.
A relatively new but proven modality is LED phototherapy using blue light (415 nm), red light (633 nm), or a combination of both.30,31 Visible light capitalizes on the photosensitivity of porphyrins, destroying P. acnes cells using peak absorption between 410 nm and 630 nm.32 Shorter wavelengths (blue light) are capable of the greatest absorption that specifically target bacteria; whereas longer wavelengths (red light) produce deeper penetration into the skin, targeting inflammation.
Considering that P. acnes is rarely present without concomitant inflammation, the treatment combination of blue and red light has demonstrated considerable success in treating mild to severe acne. Recent studies have reported an overall decrease in lesions and inflammation—in the 68% to 81% range—when physicians perform a series of eight treatments.30,31,33
More severe lesions are often complex in pathogenesis, necessitating a multifaceted approach, as demonstrated with the blue and red light combination.
Another combination therapy that targets both sebum production and bacteria is the ELOS system, which merges blue light with radiofrequency. Currently, there is a paucity of data for this system. However, two recent studies reported a 38% and 50% decrease in lesions, respectively, after eight treatments.24,34
Simultaneous use of IPL for photoactivation in ALA-PDT treatments has also been used to target bacteria and inflammation.35,36 Gold et al35 reported a 71.8% decrease in active, inflammatory lesions at 12 weeks after the final treatment. Taub24 reported analogous findings with a 70% improvement in acne grade and lesion count.
CONCLUSION
Due to the high degree of variability in lesions, the best treatment approach is to select therapies based on each patient’s acne pathogenesis. Assessing each patient for the presence and severity of the four primary causes of acne vulgaris will allow proper selection of therapies to address each source.
|
See also “Microdermabrasion Suffusion: the New Kid on the Block” by David J. Goldberg, MD, JD, in the September 2008 issue of PSP. |
Mild, noninflammatory lesions respond well to an initial topical treatment of retinoids, antibiotics, and benzoyl peroxide. Adjunctive procedures to augment treatment include microdermabrasion to remove the stratum corneum and enhance light therapies, chemical peels to reduce sebum and skin debris, laser therapy to minimize sebaceous glands, and light therapy to target bacteria. Moderate, inflammatory lesions can benefit from the aforementioned treatments, but also require a supplemental modality to address inflammation. In addition to chemical peels, red-light phototherapy specifically targets inflammation. Combination red and blue light has shown efficacy in treating moderately severe lesions, as it also treats P. acnes.
For the severe inflammatory acne that exhibits nodules and cysts, a treatment plan involving numerous therapies may be necessary—possibly involving extended courses of topical treatments, chemical peels, laser-based therapy, RF, IPL, or PDT.
A final consideration is to manage patient expectations and develop a plan for the long-term management of their acne. Patient education helps to establish realistic goals, increase compliance, and produce better overall results.
Neil Sadick, MD, FAAD, FAACS, FACP, FACPh, is a renowned dermatologist and researcher who holds board certifications in dermatology, cosmetic surgery, internal medicine, and hair transplantation. He is clinical professor of dermatology at Weill Cornell Medical College, president of the Cosmetic Surgery Foundation, and member of the board of examiners for the International Society of Hair Restoration Surgery, among other titles. He can be reached at (212) 772-7242.
REFERENCES
- Webster GF. Acne vulgaris. BMJ. 2002;325:475-479.
- Cooper AJ. Systematic review of Propionibacterium acnes resistance to system antibiotics. Med J Aust. 1998;169:259-261.
- Clarisonic. technology: The sonic difference. Available at: http://www.clarisonic.com/professional/technology.php. Accessed August 22, 2008.
- Shpall R, Beddingfield F, Watson D, Lask G. Microdermabrasion: a review. Facial Plast Surg. 2004;20:47-50.
- Lloyd J. The use of microdermabrasion for acne: a pilot study. Dermatol Surg. 2001;27:329-331.
- Nestor MS, Gold MH, Kauvar AN, et al. The use of photodynamic therapy in dermatology: results of a consensus conference. J Drugs Dermatol. 2006;5:140-154.
- Goldberg DJ, Russell BA. Combination blue (415 nm) and red (633 nm) LED phototherapy in the treatment of mild to severe acne vulgaris. J Cosmet Laser Ther. 2006;8:71-75.
- Atzori L, Brundu M, Orru A, Biggio P. Glycolic acid peeling in the treatment of acne. J Eur Acad Dermatol Venereol. 1999;12:119-122.
- Lee HS, Kim IH. Salicylic acid peels for the treatment of acne vulgaris in Asian patients. Dermatol Surg. 2003;29:1196-1199.
- Campbell RM, Monheit GD. Chemical peeling. In: Goldberg DJ, ed. Facial Rejuvenation. New York: Springer; 2007.
- Kessler E, Flanagan K, Chia C, Rogers C, Glaser DA. Comparison of a- and ß-hydroxy acid chemical peels in the treatment of mild to moderately severe facial acne vulgaris. Dermatol Surg. 2008;34:45-51.
- Grimes PE. The safety and efficacy of salicylic acid chemical peels in darker racial-ethnic groups. Dermatol Surg. 1999;25:18-22.
- Grimes PE, Green BA, Wildnauer RH, Edison BL. The use of polyhydroxy acids (PHAs) in photoaged skin. Cutis. 2004;73 (2 Suppl):3-13.
- Jih MH, Friedman PM, Goldberg LH, Robles M, Glaich AS, Kimyai-Asadi A. The 1450-nm diode laser for facial inflammatory acne vulgaris: dose response and 12-month follow-up study. J Am Acad Dermatol. 2006;55(1):80-87.
- Mariwalla K, Rohrer TE. Use of lasers and light-based therapies for treatment of acne vulgaris. Lasers Surg Med. 2005;37:333-342.
- Friedman PM, Jih MH, Kimyai-Asadi A, Goldberg LH. Treatment of inflammatory facial acne vulgaris with the 1450-nm diode laser: a pilot study. Dermatol Surg. 2004;30:147-151.
- Nouri K, Ballard CJ. Laser therapy for acne. Clin Dermatol. 2006;24:26-432.
- Konishi N, Endo H, Oiso N, Kawara S, Kawada A. Acne phototherapy with a 1450-nm diode laser: an open study. Ther Clin Risk Manag. 2007;3(1):205-209.
- Goodman GJ. Lasers and lights. In: Goldberg DJ, ed. Facial Rejuvenation. New York: Springer; 2007.
- Paithankar DY, Ross EV, Saleh BA, Blair MA, Graham BS. Acne treatment with a 1,450 nm wavelength laser and cryogen spray cooling. Lasers Surg Med. 2002;31:106-114.
- Ruiz-Esparza J, Gomez J. Nonablative radiofrequency for active acne vulgaris: the use of deep dermal heat in the treatment of moderate to severe acne vulgaris (thermotherapy). A report of 22 patients. Dermatol Surg. 2003;29:333-339.
- Gold M. Photodynamic photorejuvenation. In: Goldberg DJ, ed. Facial Rejuvenation. New York: Springer; 2007.
- Santos MA, Belo VG, Santos G. Effectiveness of photodynamic therapy with topical 5-aminolevulinic acid and intense pulsed light versus intense pulsed light alone in the treatment of acne vulgaris: comparative study. Dermatol Surg. 2005;31(8 Pt 1):910-915.
- Taub AF. A comparison of intense pulsed light, combination radiofrequency and intense pulsed light, and blue light in photodynamic therapy for acne vulgaris. J Drugs Dermatol. 2007;6(10):1010-1016.
- Gold MH. Efficacy of lasers and PDT for the treatment of acne vulgaris. Skin Ther Lett. 2007;12(10):1-6,9.
- Yeung CK, Shek SY, Bjerring P, Yu CS, Kono T, Chan HH. A comparative study of intense pulsed light alone and its combination with photodynamic therapy for the treatment of facial acne in asian skin. Lasers Surg Med. 2007;39:1-6.
- Horfelt C, Funk J, Frohm-Nilsson M, Wiegleb Edstrom D, Wennberg AM. Topical methyl aminolaevulinate photodynamic therapy for treatment of facial acne vulgaris: Results of a randomized controlled study. Br J Dermatol. 2006;155(3):608-613.
- National Institute of Arthritis and Musculoskeletal and Skin Diseases (NIAMS). 2006. Acne. Available at: http://www.niams.nih.gov/Health_Info/Acne/default.asp. Accessed September 1, 2008.
- Oprica C, Emtestam L, Lapins J, Borglund E, et al. Antibiotic-resistant propionibacterium acnes on the skin of patients with moderate to severe acne in Stockholm. Anaerobe. 2004;10(3):155-164.
- Goldberg DJ, Russell BA. Combination blue (415 nm) and red (633 nm) LED phototherapy in the treatment of mild to severe acne vulgaris. J Cosmet Laser Ther. 2006;8(2):71-75.
- Sadick NS. Handheld LED array device in the treatment of acne vulgaris. J Drugs Dermatol. 2008;7(4):347-350.
- Taub AF. Photodynamic therapy in dermatology: history and horizons. J Drugs Dermatol. 2004;3(1 Suppl):S8-25.
- Lee SY, You CE, Park MY. Blue and red light combination LED phototherapy for acne vulgaris in patients with skin phototype IV. Lasers Surg Med. 2007;39(2):180-188.
- Kim S. The dual treatment of acne vulgaris using two kinds of ELOS™ (electro optical energy) system: A simultaneous split-face trial. J Cosmet Laser Ther. 2008;6:1-4.
- Gold MH, Bradshaw VL, Boring MM, Bridges TM, Biron JA, Carter LN. The use of novel intense pulsed light and heat source and ALA-PDT in the treatment of moderate to severe inflammatory acne vulgaris. J Drugs Dermatol. 2004;3(6 Suppl):S15-19.
- Gold MH, Biron JA, Boring M, Bridges TM, Bradshaw VL. Treatment of moderate to severe inflammatory acne vulgaris: photodynamic therapy with 5-aminolevulinic acid and a novel advanced fluorescence technology pulsed light source. J Drugs Dermatol. 2007;6(3):319-322.