 |
With the recent FDA approval of the drug Asclera (polidocanol), sclerotherapy—the traditional method of treating spider veins (or telangiectasias)—may become more popular again. Though the procedure has been around for some 80 years and is still considered the best course of treatment by many medical professionals, it’s been waning in popularity and appears to be becoming a lost art.
During this in-office procedure, veins are injected with a solution using small needles, which causes them to collapse and fade from view.
Typically, the procedure improves not only the cosmetic appearance but the associated symptoms. Even though more than 375,000 sclerotherapy procedures were performed in the United States in 2008, according to the American Society of Plastic Surgeons (ASPS), the number of sclerotherapy treatments has dropped nearly 60% since 2000.
Asclera is said to cause less discomfort, ulceration, and discoloration than traditional hypertonic saline and may even be a better option to the now more popular lasers.
The decline is because of new treatment options that use laser-based devices, says Heidi A. Waldorf, MD, a board-certified dermatologist in private practice in Nanuet, NY, and the director of laser and cosmetic dermatology and associate clinical professor at Mt Sinai Medical Center in New York City. During laser treatment, intense light eliminates the veins permanently. After a laser-based treatment, bruising usually occurs in the area treated and lasts for a few weeks. The cost of laser treatment for spider veins is usually higher compared with sclerotherapy.
As Waldorf explains, laser is newer, takes less time to do than sclerotherapy, and can be relegated to ancillary staff more readily. Waldorf uses both treatments, and PSP spoke with her recently about the different treatment approaches.
PSP: What is the appropriate use of sclerotherapy?
Heidi A. Waldorf, MD: Sclerotherapy is used solely for blood vessels. Although some people use sclerotherapy for the face for certain large blood vessels and hands, it is certainly not the place for a novice to start. And quite frankly, I don’t find that those are areas that I treat. I think that there are other [treat- ments] that are better for those areas. I limit my sclerotherapy practice to smaller blood vessels of the leg. Most of the vessels that I treat are anywhere from matte telangiectasias, which are quite fine—less than .1 mm—up to about 3 mm.
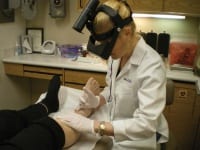 |
| Dr. Waldorf is shown doing a scleropathy procedure wearing a magnification lens with polarized light. |
PSP: Are these visible veins dangerous to a patient?
Waldorf: Spider vessels—these fine vessels that we’re talking about—are really a cosmetic concern, and they are not dangerous to the patient. If a patient, clinically, has large varicosities or other indications of deep vessel disease, a Doppler evaluation of blood flow and competency of the valves is necessary. Treatment of the small vessels won’t be successful unless the source of incompetence is treated.
The larger vessels can also have medical implications—they predispose patients to chronic swelling, stasis dermatitis, and ulcer formation. These vessels are treated with endovenous radiofrequency or laser or ambulatory phlebectomy. Fine telangiectasia is treated with either sclerotherapy or laser.
The consensus is that if you can get a needle in, sclerotherapy is the most consistently effective. Vascular-specific lasers provide an alternative for needle-phobic patients or those who have had adverse effects from past sclerotherapy.
PSP: Who gets spider veins and varicose veins, what causes them, and can they be avoided?
Waldorf: The major risk factors of getting these vessels include being a woman, hereditary factors, pregnancy, a job requiring long hours standing, and anything else that’s going to put extra stress or pressure on returning blood flow. For example, I see a lot of teachers and nurses complaining of leg veins. Crossing your legs regularly may also aggravate the condition, but it isn’t a primary etiology.
Telangiectasia and varicosities develop as the internal venous valves we rely upon to force blood flow back to the heart become incompetent and lose the ability to block backward blood flow. The vessels extend and become serpiginous. This backward flow continues through the system into the smaller vessels, which we see clinically arising along arcs of larger vessels.
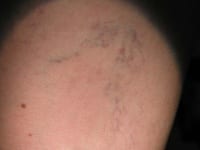 |
| Typical branched spider veins appropriate for scleropathy. |
I warn patients that vessels will recur as long as the underlying reason doesn’t change. People whose jobs require long hours standing should wear medical-grade support stockings regularly. I recommend deferring scle-rotherapy if another pregnancy is planned imminently. Keeping leg muscles in motion with exercise aids returning blood flow and improves vessel health. PSP: Sclerotherapy is an art that is very dependent on technique and proper selection of solutions. What solutions and approaches work best for you? Waldorf: I use a 30-gauge needle bent 45 degrees on a 3 cc syringe containing 2 cc’s of hypertonic saline. Using a polarized headlamp with magnification, I easily visualize and "cannulate" telangiectasia. I see the bevel of my needle underneath the skin and inject hypertonic saline with very light pressure. To reduce discomfort, I store hypertonic saline for sclerotherapy in the refrigerator, as cold saline tends to hurt less.
I use hypertonic saline rather than Sotradechol, a popular detergent scleros-ing agent, to avoid any risk for allergy. I can treat patients immediately without testing. However, hypertonic saline cannot be "foamed," which is a technique used to increase the sclerosant’s effect on larger vessels.
No matter what is injected in this area, there is a risk of ulceration if the sclerosing agent gets into the skin. Injecting slowly with excellent visualization reduces that risk—you follow the flow of the solution as it temporarily replaces blood in the vessels, so you know you’re in the right place. Note that when following the fluid through the branching vessels, there is a point that there is a limiting return because the saline will dilute out.
After injecting a given area, I massage gently both for patient comfort and to ensure that the vessel wall contact with the sclerosant. Then, I apply cold, wet gauze. The gauze absorbs injection-point blood and is soothing.
PSP: Are there side effects to treatment?
Waldorf: I warn patients the treated vessels may appear inflamed, like a bug bite or hive, or bruised after treatment for a day to 2 weeks. It can take a good month from the day of the first treatment to see results. For a patient who has a lot of vessels of varying sizes, I will bring them back for treatment as soon as 1 month. If the patient has very, very fine vessels, I might separate it by a longer interval.
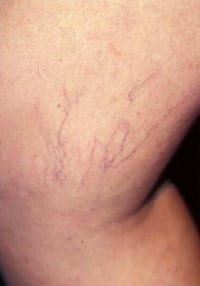 |
| Spider veins before treatment (above) and 3 months after two scleropathy sessions (below). |
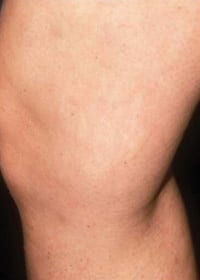 |
The most common side effect is hyperpig-mentation along the treated vessels—a hemo-siderin effect. Topical agents that target melanin, like hydroquinones, don’t help. I reassure patients the discoloration will gradually fade over 6 months to a year. On the distal legs, particularly in the presence of statis dermatitis, it will take longer.
Post-treatment support hose may reduce the development of hyperpigmen-tation, particularly in patients with larger vessels. Less common is matte telangiecta-sias, which are the fine, tiny blush of vessels that you can see after treating a larger vessel. They may be due to angiogen-ic stimulation from the force of injection, so injecting slowly may reduce its occurrence.
More severe side effects are due to inflammation from irritation from the scle-rosing agent getting into the skin surrounding the vessels. These include blistering, ulceration, and, ultimately, scarring. I advise patients to call the office if they develop a blister or wound. Starting aggressive topical care will improve the outcome.
The most uncommon side effect—but the most severe—is deep vein thrombosis, which can lead to a pulmonary embolism and death. That is much less common to happen in small-vessel sclerotherapy as opposed to large-vessel sclerotherapy. PSP: Are there any pretreat-ment or post-treatment precautions that are necessary? Waldorf: I don’t do sclerotherapy on patients with a past history of clotting diasthesis, deep vein thrombosis, or pulmonary embolism. I am particularly careful with women with a history of multiple miscarriages because that can be a sign of clotting issues.
I advise patients to avoid airplane travel for 24 hours. Support hose may be helpful to reduce the risk of hyperpigmentation and speed vessel resolution, particularly for larger vessels. Wearing support hose regularly whenever standing for long periods may reduce vessel recurrence.
Pretreatment? I have no precautions for the patients. Unlike laser therapy, for which a tan increases the risk of side effects, sun exposure is not a risk for sclerotherapy. However, most patients prefer to do this procedure in the fall or winter when they are wearing pants or opaque hose because nobody is seeing the hive-like effect or bruising after treatment. Also, since it takes at least a month to see the results, patients generally start planning treatment several months before expecting to wear leg-baring clothing.
PSP: How many treatments are necessary before a patient realizes results?
Waldorf: The number of treatments required depends on the extent of disease. Some patients will have one or two treatments, and that will give them satisfactory results. In a given session, I will do as much as the patient can tolerate and what I consider safe, generally 4 to 6 cc’s of saline. For some patients, that can be their entire anterior and posterior legs; for other patients, that may be one thigh. A given area will often require more than one treatment. I do warn patients that it can be a little like trimming circles. I can never guarantee perfection. At some point, the benefit of additional treatment of a few residual vessels must be weighed against the risk of hyperpigmentation and matte telangiectasia.
PSP: How effective is it?
Waldorf: Overall, patients are very pleased. Sclerotherapy is booked in my practice as 30-minute sessions, not because injection takes the full 30 minutes but for my staff to set up and then apply soothing dressings and/or support hose afterward.
If the patients get to the point where the sclerotherapy isn’t working, then I do a test with a pulsed-dye laser with an ellipti-calspot. Other appropriate lasers, depending on vessel size, include Nd:YAG, KTP, and diode lasers. One of the selling points for laser treatment of leg veins had been a presumed lower risk of side effects. However, post-treatment hyperpigmenta-tion and matte telangiectasia still occur. Laser therapy is also limited by skin color— parameters must be adjusted for both natural skin pigmentation and the effects of ultraviolet light exposure. Hyperpigmentation and hypopigmentation can result if not adjusted correctly. Patients also find that they have a longer period of bruising after laser than after sclero.
PSP: What do you see as future developments in this specialized area? Are any breakthroughs coming?
Waldorf: The most exciting thing happening in sclerotherapy is the recent FDA-approval of Asclera (polidocanol), for spider and reticular veins. Polidocanol is the number one sclerosing agent worldwide, has been available in Europe as Aetoxyskerol for 40 years, and has been used on ovct fivemillion patients. Like my colleagues, I’ve been anxiously awaiting its availability in the US and anticipate transferring my entire sclerotherapy practice from saline to Asclera. Happily, Bioform spent the time and money to do the testing for FDA approval; the first time a sclerosing agent has undergone that process. Polidocanol is a marvelous small-vessel sclerosing agent. It causes minimal discomfort with injection and reduced risk of injection-site necrosis, ulceration and discoloration, yet is very effective. It will be available in 0.5% and 1% concentrations for spider and reticular vessels, respectively. The availability of a safe, effective, and comfortable sclerosing agent, combined with direct-to-consumer education about sclerotherapy, will make this procedure more accessible to physicians and patients.
Amy Di Leo is a contributing writer for PSP. She can be reached at [email protected].






