|
Dermal fillers are well-known to most of us and have had a long history of useful intervention in facial rejuvenation. From the early days of bovine collagen and no-animal-stabilized hyaluronic acid, a plethora of filling agents have become available. This immediately begs the question, which one should I use? And even more importantly, where should I use which filler?
This issue becomes more complicated if we also consider filling agents as not just dermal fillers but also facial fillers. To make things even more intriguing, we need to pose the question, can we use combinations of fillers in the same patient?
One of the difficulties in talking about fillers is that not all of them are available in every jurisdiction. Therefore, some allowances need to be made. Nevertheless, some general principles apply.
In using agents in my practice, I rely on four key elements.
Hyaluronic acid is the mainstay and workhorse of fillers. In its presentation, the degree of cross-linking will make it softer or firmer, and this will impact on its longevity and how it feels to the patient.
Some filler companies have wisely developed degrees of “vertical integration” and have a range of products to cover a number of core uses. Q-Med does this well, as does Anteis with its Mesolis, Esthelis, and Fortelis range. Allergan has Juvéderm Ultra and Juvéderm Ultra Plus, as well as some collagen products it inherited from Inamed.
I consider polyacrylamide (Aquamid) to be a good product. It is a soft gel with an effective filling life of 10 years. It is important to distinguish this product from some other so-called “permanent fillers,” which have had a poor history. These other “permanents” are particulate fillers, as opposed to Aquamid, which is a gel and looks and feels like hyaluronic acid.
Any discussion of Aquamid has to acknowledge that there have been a number of reported adverse events. Most of the problems have been more to do with poor technique or inappropriate placement—or even poor patient selection—rather than inherent product issues.
The key to Aquamid is that it must be treated more like an implant than a filler. In addition, it is not a dermal filler and it needs to be placed deeply. In my opinion, the best place for this product is adjacent to the facial skeleton and not any more superficial than the subcutaneous layer.
Radiesse fits the same profile as Aquamid but is not permanent. This is, of course, both a potential advantage and a disadvantage, depending on your long-term view. Radiesse is calcium hydroxyapatite in microspherules suspended in a gel carrier. The mode of action is such that the initial product is placed as desired, and then macrophages slowly remove the gel, and it is replaced with fibroblasts, which in turn fill the space with collagen, forming a matrix. Ultimately, the spherules also degrade. Still, there is a good 12-month correction of volume.
Contrary to some claims, Radiesse is not a “stimulator” of collagen production. It provides a matrix through which collagen can be deposited.
Poly (l-lactic) acid (Sculptra) is the fourth key element, but I do not see this as a primary filler. Surely it adds volume, but it also improves the texture and quality of the area of skin above where it has been placed. No doubt there have also been problems in the past with poly (l-lactic) acid, but only if you were using it according to the original recommendations for use. With new techniques, we have virtually eliminated problem nodules in my practice.
 |
 |
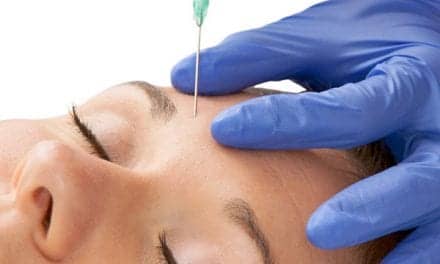
| Figure 1. In the eye trough, use a firmer hyaluronic acid filler or Radiesse placed under the obicularis oculi. The muscle is displaced forward by the filler. | |
WHERE TO USE WHAT?
In order to demonstrate the layer in which to place their product, most filler companies use a diagram showing the skin profile. We have all seen this many times. The skin is displayed in layers—epidermis and dermis—and we talk in terms of injecting superficial dermis, mid-dermis, and deep dermis.
The concept of placement in layers has been established with dermal fillers, but we need to expand this concept to facial fillers. To do this, we have to consider different layers and add in subcutaneous, submuscular, and peri-skeletal.
For a long time, we were told that injecting hyaluronic acid fillers subdermally would lead to rapid resorption and would not be effective. This is simply not true. The skin is more physiologically active than the subdermal adipose layer, and hyaluronic acid fillers will do well here. The difference, though, is one needs to use larger volumes because the “power” of the volume replacement is somewhat lessened the deeper we go.
Moderately cross-linked hyaluronic acid fillers are best layered in the dermis. Esthelis basic can be injected very superficially just like to earlier bovine collagen without the blue tindal effect of some other hyaluronic acid fillers. Highly cross-linked hyaluronic acid fillers, such as Perlane, sub Q, and Fortellis, are best subdermally or peri-skeletal.
Aquamid belongs subdermal or peri-skeletal and Radiesse similarly. However, Radiesse is flexible enough to go into the deep dermis.
Poly (l-lactic) acid is best placed subdermally, not in the dermis, and I favor its use in the soft part of the mid to lower cheek. The reason I like it here is that this part of the cheek is not really supported by underlying musculature or skeleton. The buccinator “curtain” does not really offer any support; therefore, firm fillers placed there are more readily noticeable and palpable—a real trap for the unwary.
Poly (l-lactic) acid, on the other hand, produces a thickening of the dermis due to the fibroblast stimulatory effect. When laid down as a “blanket,” it provides a good improvement in this particular area.
COMBINATIONS OF FILLERS
Clearly, there are specific applications for different products. The issue of using multiple products in the same patient needs to be addressed.
At conferences we often hear one should not mix products, and the various supply companies usually prompt this argument. If they mean do not mix them in the same syringe, then I agree. But who does that?
However, there are few impediments to using different products in the same patient. A few general rules apply:
- Separate the products either temporally or spatially;
- Do not use two particulate fillers near each other;
- A permanent particulate is not a good thing; and
- Permanent gels are generally a much better option, with few adverse events when used correctly.
 |
 |
 |
 |
| Figure 2. Fortellis subdermally overlying Aquamid adjacent to facial skeleton for malar augmentation and PLLA (Sculptra) in lower cheek area. Sculptra placed sequentially in 3 treatment sessions; Fortellis/Aquamid introduced 3 months after the Sculptra. Fringe benefit of Sculptra: it promotes improvement in texture and skin quality, as well as providing a soft volumization. | |
FACIAL PLACEMENT AND STRUCTURAL CONTOURING
One needs to consider the face as a whole. I use two basic templates for fillers. One is the Key Point Strategy, in which I focus on areas of high-value return in comparison to the volume used. Such areas are the tear trough, infraorbital rim, canine fossa, and cupids bow. There are a few more, but these are key.
Why pick these areas? When we first encounter a patient, we first engage the eyes. This gives us a first glimpse of the person and begins to set—or at least form—our expectations and perceptions.
In the next fraction of a second, we engage the mouth because we use the mouth to converse with one another. It is then that our eyes take in the basic shape and form of the face. This process takes place in fractions of a second. If we engage in an extended conversation with the patients, we have the opportunity to examine them more intently. Of course, a lot of this activity occurs at a subconscious level.
The next important template is Structure and Balance. With this template, I look at features such as the projection and fullness of the malar mound, the length and depth of the chin, the prominence of the lips, brow position, and temporal fossa.
In my method, nasolobial folds are way down the list, which may be surprising to some of you. For many practitioners, nasolabials are one of the most common areas for filler correction.
The key feature of the Structure and Balance template is to consider facial proportions and ratios, which have been published extensively elsewhere. My only point of contention with regard to “ideal” proportions is that most of us are not blessed with them. In addition, as practitioners, we do not necessarily need to achieve them, but bear in mind the overall concept of balance and harmony.
THE BLANKET COVER
Specifically, when it comes to facial contouring, think Key Point Strategy and Structure and Balance.
When it comes to using different products for specific purposes, be confident to use different fillers on the same patient. Think in three dimensions: Use deeper, longer-lasting fillers for structure and balance; and use finer, more delicate fillers superficially for the blanket cover. Use layering techniques in most circumstances.
As an example, see Figure 1. The eye trough is a versatile recipient site. Use a more firm hyaluronic acid filler or even Radiesse placed under the obicularis oculi. The filler displaces the muscle forward, and it is the muscle that provides the smooth blanket cover in order to give an even volume placement.
For malar augmentation, use Aquamid or Radiesse deeply (Perlane or Sub Q are also applicable) in a linear threading technique—the subcutaneous placement will provide a structural platform.
After that, introduce a series of small bolus injections of the same product in the peri-skeletal plane. This series of support pillars—or pearls—can then displace forward the previously created structural platform. The pearls give the volume characteristics and the projection. The structural platform is there to create the smoothness of the contour.
In selected patients, I will often use Aquamid for the pearls or pillars and then a firm hyaluronic acid filler, such as Fortellis or Perlane, as the structural platform.
The rationale is that Aquamid can provide a “permanent” scaffolding, or shape, and the temporary fillers provide a soft blanket cover. The fact that the more superficial layer is a hyaluronic acid filler means not having to worry about permanent changes in the malleable dermal layers as the patient ages. Conversely, the permanence of Aquamid to augment the facial skeleton is a great benefit.
When the patient or physician may be somewhat reserved about the permanence factor, Radiesse is a versatile alternative and can be used as both the pearls and the structural platform. Longevity for this product is a very useful and economical 12 to 18 months.
Fine wrinkles are, in reality, creases on the skin and need a fine and delicate filler placed very superficially in the dermis. To give a fine finish or a “polish,” most hyaluronic acid fillers are suitable for use with fine lines.
|
See also “Wrinkle Correction Using Fillers” by RAndrew Jacono, MD, FACS, in the April 2007 issue of PSP. |
I commonly use the Esthelis filler because it is versatile enough to use in the epidermis like the collagen of old. It is also a good choice for dermal placement. Restylane is also applicable, although it should not be used too superficially because of the “blue” effect.
CONCLUSION
If we think structurally, in the above example we have the finer, more delicate fillers in the finer, more delicate layers superficially. As we move deeper, the firmer, longer-lasting product is used in the subdermal plane and, in the deepest layer, the permanent fillers.
I’ve used filler combinations in hundreds of patients, but they are separated spatially in particular anatomical layers. Aquamid, Radiesse, and hyaluronic acid fillers can be used in the same patient with no adverse events and no indications of interactions.
John Flynn, MBBS, Dip RACOG, FRACGP, Dip.P.Derm (UK) FACCS, is a past president of the Australian College of Cosmetic Surgery and a current fellow of the College. He is a board-certified member of the American Board of Laser Surgery and a member of the International Society of Laser Cosmetic Surgeons. He can be reached at .