The decision to have breast augmentation, mastopexy, or augmentation–mastopexy surgery may not be so straightforward after all.
When a patient seeks a mastopexy or augmentation, it is reasonable to ask what bothers her about her breasts. If it is clear that the breast size is small and there is significant ptosis of the breasts, then an augmentation–mastopexy is indicated.
In part 1 of this article (“The Axillary Approach” by George John Bitar, MD, and Vinod K. Chopra; October 2007), we described the axillary technique for breast augmentation.
In part 2, we discuss a new breast augmentation–mastopexy technique, as well as how to avoid the pitfalls of the axillary augmentation procedure.
SIMULTANEOUS PROCEDURES
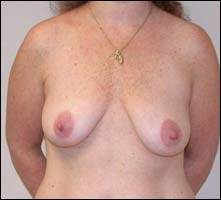
For patients wishing to have a mastopexy performed simultaneously with a breast augmentation, I have developed a simple and practical way to perform this procedure with natural results and reduced operative time (Figures 1, 2, and 3).
 |
 |
 |
 |
| Figure 1. A 45-year-old woman who received an axillary-approach breast augmentation, a Benelli mastopexy, and an abdominoplasty is shown 1 year postsurgery. | |
The idea originated while at a conference listening to a lecture about performing a lower blepharoplasty with a simultaneous subciliary incision to remove the excess skin and a subconjunctival incision to remove the fat—without disturbing the middle lamella, rather than removing the fat through the subciliary incision.
The augmentation–mastopexy is performed in the following way.
First, a breast augmentation is performed as described in part 1, up until the step in which the submuscular pocket has been created by the implant sizers through an axillary approach.
The implant sizers are left in place, and a Benelli or Wise pattern mastopexy is performed according to the surgeon’s preference. When the mastopexy is completed and the incisions are closed, the sizers are removed. Next, the permanent implants are placed through the axillary incision. The patient is placed in an upright position on the operating table for a final inspection.
When the shape and size of the breasts are satisfactory, the filling tubes are removed and the axillary incisions are closed. Finally, the dressings are placed, a bra is fitted, and the patient is awakened from the anesthesia.
PROS AND CONS
The benefits of creating two separate surgical sites for the axillary breast augmentation and mastopexy outweigh the advantages of a “single surgical site,” traditional augmentation-mastopexy with the insertion of the implants through the periareolar or anchor incision.
The pectoralis muscle is minimally manipulated, thus decreasing postoperative inflammation and pain, and preserving intact muscle coverage for the implant in case of an incisional wound infection or dehiscence.
 |
 |
 |
 |
| Figure 2. A 55-year-old woman 3 months after receiving a breast augmentation/mastopexy shows early healing results. |
The option to adjust the implant size based on tension on the NAC incision exists without difficulty; by inflating or deflating the sizer implants to achieve the desirable volume prior to committing to the final implant size.
There is no suturing in the vicinity of the implant. The suturing to create a mastopexy is performed while the sizers are in place. You can proceed more quickly without having to worry about puncturing the actual implant, thus saving precious intraoperative time.
Implant exposure and manipulation is minimized, since the pocket and mastopexy are created before the actual implant is introduced.
The major disadvantage of this approach is the placement of an axillary scar (Figure 3) in addition to the periareolar or anchor incision performed, so the patient has to consent after a thorough discussion of the available options.
The complications of our series of breast augmentations from an axillary approach—as well as breast augmentations from an axillary approach with a mastopexy—have been limited to hematomas (less than 1%), capsular contracture (1%), DVT (less than 1%), implant deflation (less than 1%), and a few patients who were unsatisfied for reasons of asymmetry.
It is important to note that, to our knowledge, there were no implant infections, “high riding” implants, “double-bubble” signs, pneumothoraces, and the loss of ability to breast-feed, permanent loss of nipple sensation, major medical complications, or mortality.
AVOIDING COMMON COMPLICATIONS
Postoperative hematoma
A small hematoma may be observed; however, if the hematoma is significant or is enlarging, then operative drainage is necessary. In 2006, Handel et al reported a hematoma rate of 1.50% to 2.89% depending on the method of augmentation used.1
 |
| Figure 3. Three months after receiving breast augmentation/mastopexy, a 55-year-old woman’s underarm scar shows early healing results. |
Prior to surgery, our patients’ own physicians evaluate them, and blood tests include an INR and a CBC. Tumescent solution is used in breast augmentations. The key is to inject the tumescent solution and wait about 7 minutes prior to beginning the operation.
This technique—along with minimal dissection, gentle handling of the muscle during the procedure, and creating the appropriate pocket size for the implant—all contribute in keeping the postoperative hematoma rate low (less than 1%).
Infection
A 2005 study reported a breast implant infection rate of 2% to 2.5%.2 The most important step in avoiding infections is to perform the surgery at a first-rate surgical facility where principles of sterility are applied regularly.
In that type of setting, patients are given the appropriate intravenous antibiotic coverage throughout the actual surgery. Gloves are changed multiple times during the operation, and only the surgeon handles the implants in the operating room, in order to ensure total sterility and avoidance of infection.
After the procedure, the physician prescribes a 1-week course of antibiotics to minimize infection. Using this technique, our patients had no implant infections.
Capsular contracture
In 2004, the FDA reported a capsular contracture (Grade III and IV) rate of 10% to 11%, at 5 years, for augmentation patients.3 Capsular contractures may be caused by a subclinical infection, by significant bleeding during the operation, or by time and collagen remodeling alone. The rate of capsular contractures in our series has been less than 2%.
Rippling
Handel et al reported the rate of breast rippling after a breast augmentation operation to be 5.7% to 14.15%, depending on the technique and type of implant used.1
Rippling can be avoided or minimized by giving the breast implant maximum coverage with breast tissue and muscle. For that specific reason, rippling is minimized by placing an implant under the pectoralis major muscle and by selecting an implant size that would be covered almost completely by the muscle.
As a result, the implant cannot be felt from the lateral edge of the breast. Because of these two guidelines, the rate of rippling among our patients has been less than 3%.
Deflation or rupture
It is difficult to quote rates of breast implant rupture or deflation because they are functions of time. The best way to minimize these risks is by paying attention to each step in the preoperative evaluation of a patient, the actual surgical procedure, and the follow-up care.
We believe that minimal manipulation of the implant itself and avoidance of suturing in the vicinity of the implant may help reduce rates of inadvertent implant injury. Our rate of deflation or rupture of breast implants has been less than 1%.
High-riding implants
The shape and look of the augmented breasts should be very natural. Critics have cited “high-riding” implants as a result of this technique.4 With use of proper surgical technique as described, good muscle dissection, and the use of a breast binder for pushing the implants down after surgery, we have not seen this problem as clinically significant.
 |
| See also “The Axillary Approach” by Goerge John Bitar, MD, and Vinod K. Chopra in the October 2007 issue of PSP. |
CONCLUSION
There are several techniques for performing an augmentation–mastopexy. The technique we have described in detail is simple, reproducible, and yields good results.
The key points, which we have discussed, should help surgeons who perform the axillary approach breast augmentation and the augmentation–mastopexy technique achieve consistently good results and a high level of patient satisfaction.
George John Bitar, MD, is a board-certified plastic surgeon who is on staff at INOVA Fairfax Hospital and Prince William Hospital in Virginia. He is the medical director of the Bitar Cosmetic Surgery Institute. He can be reached at (703) 206-0506 or .
Vinod K. Chopra received a bachelor’s of science degree in chemistry with a specialization in biochemistry from the University of Virginia. He is enrolled in medical school at George Washington University School of Medicine and Health Sciences and currently is an intern at the Bitar Cosmetic Surgery Institute.
REFERENCES
- Handel N, Cordray T, Gutierrez J, Jensen JA. A long-term study of outcomes, complications, and patient satisfaction with breast implants. Plast Reconstr Surg. 2006;117(3):757-67; discussion 768-772.
- Pittet B, Montandon D, Pittet D. Infection in breast implants. The Lancet Infectious Diseases. 2005;5(2):94-106,
- FDA Breast Implant Consumer Handbook– 2004. Available at: [removed]www.fda.gov/cdrh/breastimplants/indexbip.html[/removed]. Accessed November 2, 2007,
- Troilius C. A ten-year evaluation following corrections of implant ptosis subsequent to transaxillary subpectoral breast augmentation. Plast Reconstr Surg. 2004;114(6):1638-41; discussion 1642-1643.





