The History and the Controversy
Using autologous fat to enhance or reconstruct the breast dates back to 1895, when breast augmentation was performed using fatty tissue harvested from a lipoma in the patient’s lumbar area.
It has taken more than a century for the idea of fat grafting to the breast to come to the forefront of aesthetic and reconstructive surgery.
The development of liposuction in the early 1980s led to an efficient method of harvesting fat cells—cells that could be infiltrated into the subcutaneous tissues to correct facial and body contours. The breast was one of the first areas utilized by aesthetic surgeons for the reinjection of fat harvested by liposuction.
As with many new techniques, the use of autologous transplanted fat in the breast was controversial. By the mid 1980s, the American Society of Plastic Surgeons voiced concerns about the procedure. These concerns revolved around the idea that transplanted fat might die, creating scarring and calcification, and thereby interfere with breast cancer detection.
Surgeons speculated that fat grafting caused calcifications of the breast, and contemporary studies clearly proved them correct. Brown et al presented a retrospective study showing that calcifications were present in 50% of mammographies done 2 years post breast-reduction surgery.1 The authors also felt confident about differentiating between benign postoperative changes and those representing carcinoma of the breast.
In actuality, any breast surgery (augmentation via implants, breast biopsy, reduction mammaplasty, breast biopsy, traditional breast reconstruction with flaps, etc) can result in scarring and calcification.
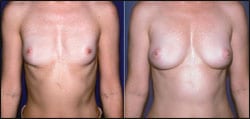 |
| Figure 1. Breast augmentation via fat grafting can produce natural-looking results for patients who require reconstruction or augmentation. |
Though surgeons knew that all of the procedures could result in calcification and scarring, they continued performing them and did not buy into the widespread negativity that was associated with fat grafting to the breasts.
A double standard developed, in which fat grafting to the breast was judged by a completely different standard than all other breast procedures.
In recent years, though, advanced radiologic screening techniques have made it easier for radiologists to distinguish between the changes associated with benign necrosis of breast tissue and changes associated with cancer.
Numerous other studies support the idea that radiologists have a high level of confidence in differentiating between fat necrosis calcifications after breast surgery and those related to breast cancers.2,3
IDENTIFYING THE RIGHT PATIENT
As with any procedure, one must weigh the benefits and potential risks of fat grafting to the breast versus more traditional surgeries and alternative procedures—breast reduction, lumpectomy, breast implants, transverse rectus abdominis musculocutaneous flaps, and radiation.
Breast augmentation via fat grafting not only includes a more natural result for patients who require reconstruction or augmentation, but also can help improve deformities such as tuberous breast deformity, inadequate soft tissue coverage over the implant, capsular contractions, and wrinkling as a result of implants.
The outcome of breast augmentation through fat grafting is related to the surgeon’s level of expertise and technique used.
The technique must include all precautions to ensure that the maximum survival of fat tissue occurs. This can be achieved by reducing the possibility of trauma to the harvested site, demonstrating correct refinement of the tissue, as well as the appropriate placement of small aliquots instead of large portions.
When the cannula is inserted, the amount of fat grafted should be minimized to increase the contact surface area between the grafted fat and the recipient tissue. Furthermore, the grafted fat should be placed in proximity to the patient’s blood supply. This will increase fat survival rates and reduce both the implication of fat necrosis and calcification risk.
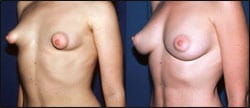 |
| Figure 2. The procedure can help repair tuberous breast deformity, inadequate soft tissue coverage over an implant, capsular contractions, or wrinkling as a result of implants. |
This procedure requires a significant amount of time. For example, a review of my recent breast patients revealed that the procedure required 2 hours to place the initial 100 cc and approximately 45 minutes for each additional 100 cc. A normal breast augmentation will usually take 4 hours or more.
As with all aesthetic surgery breast procedures, there are risks. Apparently, the risks of fat grafting to the breast are similar to the risks associated with traditional breast surgery or radiation to the breast.
As fat grafting does not involve open incisions, there is less risk in terms of damage to nerves, blood vessels, and ducts than in open surgery.
As fat is harvested from other locations in the body, there is the potential for creating deformities in the donor sites. Moreover, as with any breast surgery, fat grafting carries with it the possibility of fat necrosis, and the development of calcifications, cysts, or lumps.
BREAST CANCER DETECTION
All breast surgeries pose potential problems for cancer detection. The incidence of calcification after any type of breast surgery has been reported to be as high as 50%.
Therefore, the experienced eye of a well-trained radiologist is a very important element in reliably screening any woman, regardless of surgical history, for cancer post breast surgery.
MRIs and sonograms may be necessary to aid in the evaluation. Biopsies should be done for any lesion not easily ruled out by other means. However, unnecessary biopsies are a potential risk following this and any breast procedure.
Now that we are recognizing the importance of fat grafting to the breast, we need to begin well-thought-out clinical studies to further document not only safety but also efficacy.
EFFICACY OF BREAST RECONSTRUCTION USING FAT
Currently, a large body of documentation supports the indication and successful outcome of autologous fat transplantation for breast enhancement and reconstruction, despite any controversy.
- Coleman SR, Saboeiro AP. Fat grafting to the breast revisited: safety and efficacy. Plast Reconstr Surg. 2007;119(3):775–785; discussion 786–787.
- Delay E, Delpierre J, Sinna R, Chekaroua K. How to improve breast implant reconstructions. Ann Chir Plast Esthet. 2005;50(5):582–594.
- Missana MC, Laurent I, Barreau L, Balleyguier C. Autologous fat transfer in reconstructive breast surgery: indications, technique and results. Eur J Surg Oncol. 2007;33(6):685–690.
- Pierrefeu-Lagrange AC, Delay E, Guerin N, Chekaroua K, Delaporte T. Radiological evaluation of breasts reconstructed with lipomodeling. Ann Chir Plast Esthet. 2005;51(1):18–28.
- Rigotti G, Marchi A, Galie M, et al. Clinical treatment of radiotherapy tissue damage by lipoaspirate transplant: a healing process mediated by adipose-derived adult stem cells. Plast Reconstr Surg. 2007;119(5):1409–1422; discussion 1423–1424.
- Spear SL, Wilson HB, Lockwood MD. Fat injection to correct contour deformities in the reconstructed breast. Plast Reconstr Surg. 2005;116(5):1300–1305.
- Yoshimura K, Sato K, Aoi N, Kurita M, Hirohi T, Harii K. Cell-assisted lipotransfer for cosmetic breast augmentation: supportive use of adipose-derived stem/stromal cells. Aesthetic Plast Surg. 2007 Sept 1 [epub ahead of print].
These reports document excellent outcomes in the treatment of radiation damage to the chest, in reduction of capsular contraction, and in soft tissue coverage of breast implants.
Sydney R. Coleman, MD, received his doctorate in medicine from the University of Texas, followed by an internship and general surgery residency at the Ochsner Foundation Hospital in New Orleans. His New York City practice opened in 1985. Coleman is board certified in plastic and reconstructive surgery and can be reached at (212) 571-5200.
References
- Brown FE, Sargent SK, Cohen SR, Morain WD. Mammographic changes following reduction mammaplasty. Plast Reconstr Surg. 1987;80(5):691–698.
- Kneeshaw PJ, Lowry M, Manton D, Hubbard A, Drew PJ, Turnbull LW. Differentiation of benign from malignant breast disease associated with screening detected micro calcifications using dynamic contrast enhanced MRI. Breast. 2006;15(1):29–38.
- Yunud M, Ahmed N, Masroor I, Yagoob J. Mammographic criteria for determining the diagnostic value of micro-calcifications in the detection of early breast cancer. J Pak Med Assoc. 2004;54(1):24–29.



