When you ask Ira D. Papel, MD, a question about facial plastic surgery, and rhinoplasty in particular, you are likely to get a thorough and informed answer. But that’s not all. You will probably get the historical precedents and the medical background that created the answer and the original question, as well.
Papel, in private practice in the Baltimore area and plying his trade since 1987, is a go-to guy if you want to know what are the latest technologies and advances in the field. Recently, PSP spoke with him about a favorite subject of his—primary and revision rhinoplasty. What are the advances made in recent years that are likely to revolutionize the field? What technologies look promising? What techniques work better than others?
Board-certified in both Facial Plastic Surgery and Otolaryngology—Head and Neck Surgery, Papel received a BA from The Johns Hopkins University and an MD from Boston University School of Medicine. After his residency at The Johns Hopkins Hospital in Otolaryngology—Head and Neck Surgery, Papel completed a fellowship in facial plastic surgery at the University of California, San Francisco.
Currently, as an associate professor at Johns Hopkins, Papel is actively involved in surgical training of medical students, residents, and fellows. In addition to serving as co-director of the Facial Plastic Fellowship at Johns Hopkins, he has been invited to serve as a visiting professor at more than 27 universities in the United States, Europe, South America, and Asia. He is the immediate past president of the American Academy of Facial Plastic and Reconstructive Surgery for 2005 through 2006.
In addition, Papel is the co-author of a well-regarded tome, Facial Plastic and Reconstructive Surgery (Thieme Medical Publishers; 2002), which he wrote with Wayne F. Larrabee, MD, G. Richard Holt, MD, and others. Known as a standard reference in the field, the book includes sections on endoscopic facial surgery, microvascular facial reconstruction, minimally invasive facial cosmetic procedures, pediatric rhinoplasty, tissue engineering, and nonablative skin resurfacing techniques.
ON RHINOPLASTY: WHERE WE STAND
Ira D. Papel, MD: Overall, rhinoplasty continues to evolve and become more sophisticated. The general trend over the last 40 years has been to be more conservative and preserve structure. It is not about how thin you could make it but the overall shape with respect to the face that is important.
In the 1960s, it used to be they took everything out they could. If they did not like it they went back and took more out, and eventually you had a bag of skin that was just kind of hanging there. We are better than that now. And we know about certain strengths and buttresses and areas of structure that need to be preserved—or we lose, not gain.
Rhinoplasty is not always about making a nose smaller but making it a shape that fits the face. It took [physicians] a long time to figure that out.
The modern era of rhinoplasty did not really start until the late 1980s—when people started putting stuff back in rather than just taking stuff out. And all that stuff at that time was just cartilage.
 |
 |
 |
 |
 |
 |
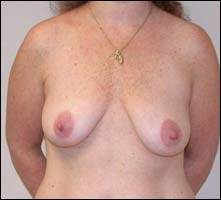
| Preop and postop images of a woman who had multiple silicone implants with loss of the lip soft tissue and cartilage. | ||
USING OUTSIDE MATERIALS
Papel: Throughout rhinoplasty history, it always has been a big temptation for physicians to use outside materials. And if you go back in history, even to the 18th century and before, surgeons found ways to either reconstruct or change the shape of noses using foreign things.
In the late 19th century, Jacques Josephs, who was very famous and is known as one of the original plastic surgeons, used ivory that he got from a Steinway piano factory in Berlin for augmenting noses, especially noses which had been damaged by accidents or in war, etc. He got away with it most of the time but not all the time.
Paraffin was used frequently. It was very popular for use in the face too, although not with very good long-term success. Almost everything got infected and had to come out. Animal parts, duck breast bones, cow cartilage, etc, was used. This was in the early 20th century, as well. That kind of went away but then other things came back.
Proplast was a kind of synthetic material that was popular in the late 1970s early 1980s, but there were so many failures that the FDA took it off the market. Gore-Tex is in wide use, especially overseas. Not so much here in the US but in Asia—very, very popular. And silicone implants are still used quite a bit. And recently in the United States, Medpor has become popular.
Medpor is used in facial reconstruction quite a bit and increasingly in rhinoplasty, although we have seen some pretty disastrous failures. The problem with all these synthetic products is when they fail, they really fail big time. You get all kinds of very, very nasty loss of tissue and scar contraction; as well as loss of the nose, that kind of thing, which is devastating.
The bottom line is there’s no synthetic implant that’s really great. There’s always at least a 5% chance of long-term infection. That doesn’t sound like much, but if you are one of those 5% and you get infected and then you lose tissue and get scar contraction, it’s pretty ugly. And it’s sitting right in the middle of your face, so it can be very devastating.
PSP: Five percent is pretty high, actually, when you think of all the different rhinoplasty procedures that are performed just in the United States.
Papel: I think it’s very significant. And even with Gore-Tex, which is considered safe because it’s easy to take out, you’re looking at 3% to 4%. The others are generally higher. And those are minimum numbers, reported numbers. We don’t know about the unreported ones.
PSP: You have to figure there is going to be a tipping point there.
Papel: This topic has been an active point of discussion for a long time. Not so much in the public eye, but among surgeons. That really has divided surgeons into two camps: those who will use synthetic implants and those who won’t. There is a smaller third camp—those who will use synthetics only is special circumstances. That is the option of using the patient’s own cartilage, which is always the safest thing although it’s not always the easiest thing. It requires more skill. It requires more surgery because you have to harvest the cartilage.
If a patient has cartilage in their nose that can be used—such as in their septum—that’s the first choice. The second would be ear cartilage, and the third choice would be rib cartilage. And with the rib, it’s like having a second significant operative site—it adds time, expense, and discomfort. Using your own cartilage is pretty much always safe, but it’s not always the easiest thing to use. And my feeling is that if the patient has their own cartilage to use, we should use it. In light of all the other problems, we know it’s safe, the infection rate is close to zero, and the long-term survival of the cartilage is excellent. However, the aesthetic results may not be as good because it’s not as exactly moldable or predictable as synthetic implants.
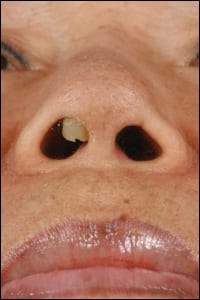 |
| In this female patient, a Medpor extrusion is plainly visible. When synthetic products fail, they can fail in very noticeable ways. |
What makes synthetic implants so attractive is they’re easy, they’re smooth, they can be preformed, and the patient has no second site for surgery. Therefore, it could even be a whole lot less expensive because you have less operating time, less surgeon time, and the implants tend to be not that expensive—a couple of hundred dollars for an implant. When you compare that to the cost of the whole surgery, it isn’t that much. You can see how it would be very attractive.
PSP: With the use of the synthetics, though, does the 5% infection figure and other problems enter?
Papel: Yes. When you use [synthetic implants] for reconstructive surgery, and the patient has had multiple operations and maybe chronic infections in the past, and so forth, the failure rate is much higher.
HARVESTING CARTILAGE
Papel: The only synthetics that are really being used now are Silicone, Gore-Tex, and Medpor. And they’re being played out against using a patient’s own cartilage, as well as something that’s come back from the past—human cartilage or, more accurately, cadaver cartilage. In the past, most people said cadaver cartilage wouldn’t hold up. Nowadays, there’s good evidence that when obtained properly and treated properly, these grafts are pretty good.
Russ Kridell recently published a paper1 with over a thousand grafts in a 20-year follow-up, and that’s put a whole new spin on the grafts issue. The patients always ask themselves, “Do I really want a dead person’s cartilage in my nose? Is there a chance for a disease transmission? Will this hold up over 30 years, if need be? Or will turn into scar tissue and go away?” Nobody really knows that. But the indications are that, at least for up to 20 years, it’s probably OK. And that’s a whole lot easier than harvesting a graft from a rib. Cutting it up and carving it and adding it could add a couple of hours to an operation.
The synthetics tend to be quite easy. You don’t have to harvest them, and they are generally easy to cut and form and put in place. Gore-Tex sheets are incredibly easy to use. You just cut the sheet where you want with the scissors and slide it in, maybe suture it in and you’re done. The nice thing about Gore-Tex is if it does get infected, which it can, it’s easy to take out before there’s a lot of damage.
Something like Medpor, in which you have a tremendous amount of tissue integration, is really hard to take out. And I’ve chased some of these things. It takes a year or two for all the little pieces to come out. That’s what I have seen really devastating results from. And yet Medpor is getting more and more popular even though it’s got, I think, the highest rate of complications.
Looking forward, have you heard about the orthopedic cases where you can harvest a piece of cartilage and then culture cartilage and reimplant it? Sooner or later, that is going to be available for rhinoplasty. This is where you can harvest a piece of septal cartilage or any piece of cartilage in the nose and then send it to a lab. They can grow a certain amount for you. It may take months, and perhaps the lab can even grow it in a mold that you know comes preformed, which you can use to replace parts of noses.
With the growing of nasal cartilage, these labs have not had great success. There was a paper 5 or 6 years ago, in which [scientists] cultured the cartilage from a mouse into the shape of an ear and then attached it to the mouse’s back. The problem was that the cartilage didn’t hold its shape—it then morphed into kind of a round ball, which is not what you want to have happen if you put it into somebody.
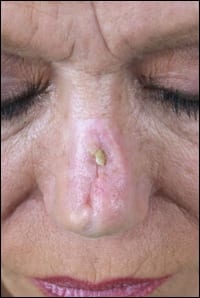 |
| An example of an infected silicone implant, which can result in scar contraction as well as loss of nose tissue. |
THE PIGSKIN PARADE
PSP: I have heard that pigs are the most similar to humans with regard to skin and cartilage.
Papel: Yes, and it’s remarkable how close they really are. That’s why you can use temporary skin grafts that come from pigskin. Evolence, the injectable, is made from porcine collagen. And you don’t have to get skin tested to use it—humans just don’t react to it.
Another model that may happen soon is a porcine dermis product for use in breast reconstruction. It works as well as human skin and with no rejection. I’m talking about producing animal cartilage, which is irradiated, and which may be very useful in human facial and nasal reconstruction. This is just a concept, but it has potential.
PSP: Have these advancements and possible advancements led to any new efficiencies in surgical techniques?
Papel: If you don’t have to harvest tissue and cartilage from other places, and if you can literally just order the [tissue and/or implants] you need to perform the rhinoplasty and have it delivered to you, you can save the patient 30% to 40% in costs due to reduced operating time. If you just have to literally open a nose and reconstruct it with pieces you already have, that’s a huge advantage. It doesn’t do all the surgery for you, but you get better tools to work with than we have now—and with less morbidity and less recovery time.
FILLERS AND OTHER CONTROVERSIES
Papel: When it comes to using filler materials for rhinoplasty, there are two camps. First, there’s the experienced surgeon who does a lot of rhinoplasties who is very skeptical about using fillers. Certain fillers, when used in small amounts for small defects, are fine. This is especially true with the hyaluronic acid products when they are used to fill in small depressions, and so forth, just to smooth things out. I think most people feel that it’s safe, it is effective, and it is helping people to avoid surgery and gets better results.
On the other hand, you have a lot of nonsurgeons who are using Radiesse, Perlane, or Juvéderm Ultra Plus—they are all pretty thick fillers to try and change the whole basic shape of a nose.
These doctors are injecting large amounts into areas they do not understand, trying to get the nose to change shape. And the best that they can ever get is 6 to 9 months of some change and then they have to repeat it. Under this arrangement, patients have to spend a couple thousand dollars every 6 to 9 months, which does not really make a whole lot of sense.
Worse still, the filler use is also causing complications. With Radiesse, especially, there have been a lot of granulations, and just chronic inflammation that is hard to get rid of. Also, they are putting so much skin under pressure that they are causing the chlorosis of the skin, which could be devastating. It means patients have permanent contraction and scarring, which you may never be able to get corrected.
The bottom line is, small changes with the hyaluronic acid, which are fairly harmless and don’t cause granulation. However, when you are using fillers to completely reshape the nose to increase projection to build up a dorsum, the results are not good and they could be dangerous.
PSP: Where is the effort coming from to use fillers versus surgical approaches?
Papel: It is not coming from the core specialists who pretty much do facial plastic surgery and plastic surgery, or the oral and maxillofacial surgeons who are at least trained surgeons. Then you have got a lot of what we call noncore people—the gynecologists who are doing cosmetic surgery, the dermatologists who are trying to expand scope of practice, etc.
And I know that I do not want to open up that whole interspecialty issue, but let’s just say that the core specialists who do rhinoplasty generally are not doing a whole lot of injectables. It is expensive, it has no real long-term lasting effects, and it could be dangerous.
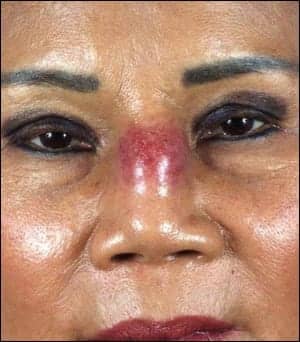 |
| Another case of an infected silicone implant. Although silicone implants are still used quite a bit, postop copmlications can be devastating. |
RHINOPLASTY IN THE WORLD STAGE
Papel: I have been in the Middle East a half a dozen times in the last 2 years so teach about rhinoplasty. The capital of rhinoplasty in the world today is Iran. They do more rhinoplasties there per capita than any place in the world. It is a haven right now for cosmetic surgery.
PSP: Is it also a place where the physicians are truly well trained?
Papel: Not necessarily, but I think they are getting better at it. I was over there last year, and I spent a week in Shiraz and Tehran. It is very hard for them to go to courses outside their country and get adequate training, but the doctors there are making a big effort to get educated. For a long time, I think they have been substandard but they are slowly improving.
Everywhere you go in Tehran, you will see people walking down the street with bandages on their noses. Some of the doctors there do seven or eight rhinoplasties a day. However, they are doing something very simple. We could not do seven or eight per day—it would kill me if I tried to do that. They are basically doing a hump removal, very minimal tip work, and osteotomies. Then they are done. And that takes them 30 to 40 minutes per patient.
Iranian physicians are coming [to the United States] and getting instruction. It is not common for Americans to go to Iran, but a few have gone there to offer instruction, as well as some very sophisticated European surgeons.
Worldwide, for rhinoplasty, the Middle East is the growth area—not just Iran but Saudi Arabia, Dubai, the Emirates, Bahrain. Wherever there is money, and there is a lot of money in the Middle East, they are going for cosmetic surgery. And it has always been popular in Pakistan and Egypt. I was in Egypt twice last year for rhinoplasty courses. Of course, Egypt is a much more open society than Iran, and there are huge practices there.
PSP: What about rhinoplasty from other countries coming to the United States. Do physicians coming here from other countries have to be “brought up to speed” on procedures and approaches, as well?
Papel: I will tell you a story of a patient we that saw a few months ago, a Korean-American woman probably in her 50s. When she was in her 20s, she had an implant done in Korea. In those days, well, nobody really knows what kind of training these doctors had. I’m not even really sure they were doctors, but these … let’s call them, ah, I don’t even want to call them surgeons.
PSP: Practitioners, maybe?
Papel: These practitioners, or whatever, would go from town to town in Korea and for a small fee they would do a dorsal implant, because a lot of the Koreans had very shallow noses and they wanted a stronger bridge. Using a local [anesthesia], on the kitchen table, they would put an implant in. It took them all of 10 or 15 minutes. It is very, very common. This Korean-American woman eventually came to the United States. She had some problems and she saw a doctor in the Washington, DC, area and had an operation. She was not sure exactly what kind of procedure she got, but she had more problems. Basically, she had a draining infection from her nose for a couple years, just pus coming out and smelly.
She got referred up to our office, and I took a look at her. It was pretty obvious she had an infected implant, but I really was not sure what was done. She gave me the name of this other physician who operated on her in Washington. I do not remember [the physician’s] name, but she was a doctor, apparently licensed in the United States but she was of Korean ancestry.
I called her up at the request of the patient and I said, “Can you send me the notes of what you did?” And she just started laughing. And I said, “Why are you laughing?” She said, “We do not do that kind of thing. We do not make operative notes. We just operate.” In the United States, not to have records of what you have done is heresy. So I asked her what kind of doctor she was and she said, “Oh, I am a general practitioner. But when I lived in Korea, I was a cosmetic doctor.” And cosmetic means she did things like implants and stuff but with no real training. So, I asked her if she remembered what she did and she said, “Not really. We do not keep records.”
Finally, I brought my patient into the operating room, opened up the nose and found the original implant, as well as another implant put on top of it in spite of a draining infection. We had to take all that out. I used rib cartilage to reconstruct her.
This is the kind of stuff that goes on in the background, all over.
PSP: Patients should always check their doctor’s credentials.
Papel: I think we have to be a little more aggressive than “buyer beware.” My patient is a sophisticated, college-educated woman, and that is the kind of practitioner she went to. Granted, there is a cultural issue here because Koreans like to go to Korean doctors. I can understand that.
Janine Ferguson is a contributing writer for PSP. She can be reached at [email protected]
REFERENCE
- Kridel RWH, Ashoori F, Liu E, Hart C. Long-term use and follow-up of irradiated homologous costal cartilage grafts in the nose. Arch Fac Plast Surg. 2009;11(6):378-394.