 |
There are no comprehensive reports in the medical literature that define the frequency of hair loss associated with the various facial-plastic surgical procedures.
Many plastic surgeons do not even mention these possible complications in the surgical consent form, but the problem is real and can be devastating to patients.
Thankfully, some hair-transplant surgeons—including those with plastic/aesthetic surgery training—recognize the problem.
Many have addressed the complications with hair transplantation.
The open brow lift produces four types of hair problems:
- A widened scar at the point where the open surgery was done, often measuring 3 mm to 7 mm in width;
- An elevated or uneven hairline;
- A scar at the frontal hairline that shows both the scar and pigmentation changes; and,
- Reactive hair loss at the hairline, in the corners, and/or in the temple peaks, which is sometimes irreversible.
The focus on lifting the brows can often raise the hairline to such a degree that the aesthetic proportions of facial beauty are lost.
As the frontal hairline frames the upper one-third of the face, the proper location of the hairline is critical in achieving a balanced facial symmetry.
THE GOLD STANDARD
Follicular unit (FU) grafting and transplantation is currently the gold standard hair restoration technique.1-6
Autologous donor hair is identified from the occipital area of the scalp then surgically removed via strip harvesting or follicular unit extraction (FUE).7
After the donor hair is harvested, the natural anatomical hair groupings of one to three hair FUs can be identified under magnification using stereoscopic microscopes.
Extraneous epithelium and fat tissue is dissected, and only the elemental FU is preserved for transplantation. The distribution of these FU grafts is critically important to the aesthetics of the process.
Single-hair FUs should be used exclusively in the frontal hairline and at the temple peaks.
In the early 1990s, cobblestoning or pitting of the recipient skin was commonly seen, because the grafts were often multiple FUs and extraneous tissue was transplanted in large-incision recipient sites.
To avoid this problem, carefully trimmed, naturally occurring single-hair FU grafts were placed at the leading edge of a hairline and staggered to produce a hairline indistinguishable from a normal hairline.
The recipient-site incisions must be very small and should only be as large as to permit teasing the grafts into the recipient site.
These incisions are often the size of a 20- to 21-gauge needle. These small recipient sites, along with carefully trimmed FU grafts, ensure minimal skin scarring and pitting in the recipient area.
Hairs at the temple peaks are often finer than hair found elsewhere in the scalp. Unfortunately, hair from the occipital donor area often has a slightly thicker texture than the native hair found in the temple peaks.
Thus, the artistic use of single-hair FU grafts is critical to mimicking the soft and subtle appearance of the temple peaks.
If a person has coarse hair, the hair transplant into the temple peaks can be a potential problem. When this situation occurs, the grafts can be strategically altered to make them grow finer, by dissecting a portion of the bulb.
As the hair grafts grow through the scalp at the same angle at which they were placed, angulation and direction of recipient-site incisions are a critical component in planning the transplantation.
The hairs between the left and right parts of the temple peaks should (at the hairline) be horizontal to the “ground” (pointing forward) and parallel to each.
At the part in the hair, there is a transition from forward pointing to a direction that allows for the side hair to be transitioned forward and downward to the sides.
 |
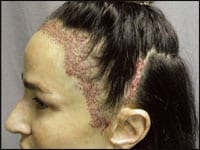 |
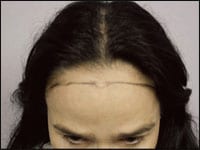
| Figure 1. A postfacelift, 43-year-old female presented a disproportionate forehead elevation and frontal hairline recession with widening of the surgical incision scar. | Figure 2. This is a classic case of the complications of hair loss and scarring, as well as the loss of ideal facial proportions. |
 |
 |
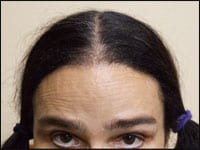
| Figure 3. The corrective repair shown in these figures took two hair transplant procedures totaling 3,508 grafts. | Figure 4. The key to adequately camouflaging the widened scars with hair transplantation is to place each graft in very close proximity to one another (dense packing). |
HARVESTING TECHNIQUES
Two harvesting techniques are used today:
- Linear strip harvesting, in which a section of scalp is removed from the “donor” area where permanent hair is found; and
- FUE, in which single follicular units are removed one at a time with a very small (0.9-mm-diameter) punch.
In both techniques, the FU’s integrity must be preserved and excess tissue must be dissected under high-power magnification.
This technique creates the most natural appearance of the hair at the recipient site, closely adhering to nature’s intended appearance.
In linear strip harvesting, the donor wound is approximated and closed under minimal tension using staples or sutures.
In FUE harvesting, the donor wound is left alone to heal by secondary intention because of its submillimeter size.
Due to the small size of each wound, there is minimal detectable scarring on the donor area when you use the FUE harvesting technique.
There is linear scarring on the donor area with the strip harvesting technique, but the scar is readily disguised with the patient’s donor hair.
CASE STUDY
The following is a case of a 43-year-old female whose facelift resulted in a disproportionate forehead elevation and frontal hairline recession with widening of the surgical incision scar.
Despite scar resection and revision performed by her plastic surgeon, the scar returned.
This is a classic case of the aforementioned complications of hair loss and scarring, as well as the loss of ideal facial proportions. A series of this patient’s before-and-after photographs are shown (Figures 1 to 4). The corrective repair shown took two hair transplant procedures totaling 3,508 grafts.
I have been treating scalp scars for many years using hair transplantation. The most common scalp scars are from brow lifts and facelifts.
|
See also “Hair Transplantation: A New Relationship,” by Jeffrey Frentzen and Jeffrey S. Epstein, MD, FACS, in the December 2007 issue of PSP. |
Neurosurgical craniotomy and shunt scars have also been treated with hair transplantation, with remarkable results. The use of hair transplants in many of these situations is ideal.
Attempts to excise scars that are not on the Langer’s lines tend to fail; and small flaps are inferior to FU hair transplants in most situations.
The key to adequately camouflaging the widened scars with hair transplantation is to place each graft in very close proximity to one another (dense packing).
Scalp scars resulting from aesthetic surgical or neurosurgical procedures respond well to modern FU hair transplant techniques.
William R. Rassman, MD, is the founder and president of the New Hair Institute Medical Group, with offices in Los Angeles and San Jose, Calif, that focus on hair transplantation. He is certified by the American Board of Surgery. He studied at the Medical College of Virginia, Richmond; the University of Minnesota, Minneapolis; Cornell Medical Center, New York City; and Dartmouth Medical School, Hanover, NH. He can be reached at .
Jae Pak, MD, has, with Rassman, pioneered hair transplant methods, automation, and instrumentation, and has been intimately involved with innovative hair transplant surgical techniques incorporating new technology. For more than 9 years, Pak has developed new surgical techniques and has invented surgical instrumentation to further advance the field of hair transplant surgery. He can be reached at (800) 639-4247.
REFERENCES
- Bernstein RM, Rassman WR. Follicular transplantation: Patient evaluation and surgical planning. Dermatol Surg. 1997;23:771-784.
- Bernstein RM, Rassman WR. The aesthetics of follicular transplantation. Dermatol Surg 1997;23:785-799.
- Bernstein RM, Rassman WR. The logic of follicular unit transplantation. Dermatol Clin. 1999;17(2):277-295.
- Rassman WR, Pomerantz, MA. The art and science of minigrafting. Int J Aesthet Rest Surg. 1993;1:27-36.
- Rassman WR, Carson S. Micrografting in extensive quantities; the ideal hair restoration procedure. Dermatol Surg. 1995;21:306-311.
- Bernstein RM, Rassman WR, Szaniawski W, Halperin A. Follicular transplantation. Int J Aesthet Rest Surg. 1995;3:119-132.
- Rassman WR, Bernstein RM, McClellan R, et al. Follicular unit extraction: Minimally invasive surgery for hair transplantation. Dermatol Surg. 2002;28(8):720-727.



