|
Chemical peels have been around for centuries. It is believed even Cleopatra used them when she bathed in sour goat’s milk—though she probably didn’t realize the lactic acid was giving her skin a rejuvenating peel.
Currently, chemoexfoliation is one of the most powerful tools available to a cosmetic surgeon. According to the American Society of Plastic Surgeons, more than a million chemical peels were performed in 2006.
PSP discussed the procedure with James R. Shire, MD, FACS, a facial plastic surgeon based in Chattanooga, Tenn, who has performed more than 500 chemical peels, of which 100 are the new modified peels.
What are the different options for skin resurfacing?
Shire: The three medical techniques used for resurfacing are dermabrasion, lasers, and chemical peels. It doesn’t make a difference about the mode that you use to do the resurfacing. The rules are always the same.
When you resurface, you are taking the top layer of skin off so your body can replace it with brand-new skin that doesn’t have the problems that the skin that you removed has in it. The two things we use it for are lines and wrinkles and pigmentation problems.
There are two problems associated with resurfacing. One is making sure the peeled skin is replaced with brand-new skin, not scar tissue. Scar tissue will form if you go past the reticular dermis. So you need to stay above that level to get skin formation. You are limited to depth on any resurfacing.
Pigmentation is the second problem. Most of the pigment cells are scattered around in one layer. If you don’t go below that layer, you won’t lose the base coloring of the skin. If you go into it, you will remove the majority of the pigmentation and you will be left with that chalky-white, alabaster complexion. These facts of resurfacing we can’t change.
I don’t use dermabrasion anymore. I initially was trained on it, but I consider it not as precise. The aerosolized particles increase the risks to the health care personnel.
Lasers, I believe, have an innate problem. They set the penetration above the layers we just talked about, but unfortunately, lasers generate heat. Heat penetration, or thermal damage, around the area will cause scarring and hypopigmentation. The other problem is the heat that is generated denatures the elastin in the skin. Initially, it tightens the skin and it looks nice and tight, but 2 to 3 years down the road, that denatured elastin is gone and the patient turns crepe papery. That is why I don’t like lasers.
The third medical skin resurfacing technique is the chemical peel.
What are the different types?
There are three classifications of chemical peels, and they are distinct per class, they are not interchangeable, and they are not compoundable. If you need one type of peel and you want to do the lower type of peel, you can’t do eight or nine of them to get to the next level. It just won’t happen.
There are light peels, intermediate peels, and deep peels. Light peels are glycolic acids, the alpha hydroxies, the resourcinols, and kojic acid types. They are basically exfoliants. They aren’t going to get rid of a line or a wrinkle; I don’t care how many of these peels you do.
The next level is intermediate-based peels—TCA, or trichloroacetic acid. These go to through the epidermis to the first dermal layer. These are good for fine lines and can remove very superficial hyperpigmentation from sun damage. But if you have anything that is a deep line or a medium-sized wrinkle or any darker pigmentation, it’s not going to touch it.
Intermediate peels can be repeated if you need to. In fact, they most likely need to be repeated because the repair is so superficial that [patients are] just going to come back to the way they were before.
Usually, intermediate peels are for younger people—people who have abused the sun. I don’t even do many intermediate peels anymore because I have an IPL (intense pulsed light). I have been replacing most of those intermediate peels with the IPL because there is no downtime with it. With an intermediate peel, a patient’s downtime is going to be 7 to 10 days.
 |
 |
| Figure 1. Middle-aged female patient number one at 3 weeks (left) and at 4 months postop. | |
Anything else will require a deep peel. Deep peels can be controlled to be superficial deep to deep deep. Deep peels are the real workhorses when we talk about resurfacing peels.
How does a chemical peel differ from a laser peel?
Pretty significantly from the patient’s standpoint. Number one, when you use a laser, you are burning the top layer off and it’s gone completely, leaving a raw surface there, with exposed nerves and exposed tissue. Therefore, lasers hurt and they can cause infection.
 |
| Figure 2. Deep peels are the workhorses of resurfacing. |
With a chemical peel, all you are doing is applying a chemical that penetrates to a certain level of the skin. At that point, it causes layer separation. When the layers separate, new skin can actually grow in-between the layers. When that new skin is completely re-epithelialized, that top layer will then slough off or peel away. Therefore, you don’t ever have an exposed surface, and therefore, peels don’t hurt. They’re not painful at all. And they rarely get infected because they’re not exposed to infection. All of those things mean that you are going to not be as red, and that you will heal faster and recover much easier.
Lasers are high-tech, and people believe high-tech means better, which isn’t necessarily true. One of the reasons lasers became popular is because they’re easy to learn. Chemical peels are not as easy to learn—there is a learning curve, and only trained and experienced specialists should do them.
What is the history of chemical peels?
Chemical peels have been around for a few hundred years; at least since the late 1800s. They were mostly done by laypeople who had secret formulas. Until the 1930s and ’40s, the laypeople doing them didn’t want to have anything to do with the medical profession at all. However, a few physicians got in good with some of these “laypeelers,” got a hold of their formulas, and started to do some clinical trials and tests.
The most popular deep peel is the Baker-Gordon Peel, which was first publicized in the early 1960s. It’s a combination of phenol and croton oil, septisol, and distilled water. Different forms and variations have been used, but this mixture has really been the hallmark of chemical peels for years. There were many techniques and ways of doing it—taped/occluded peels or unoccluded peels.
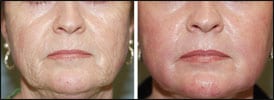 |
| Figure 3. Middle-age female patient number two at 1 year (left) and 4 years (right) postop. |
What are some of the myths and truths about phenol and croton oil?
It was the taped peels that gave the Baker-Gordon Peel a somewhat bad name in the past—with patients ending up with an alabaster white skin. What they were doing was allowing the chemical to penetrate too deeply, and they were getting scarring and loss of pigmentation.
With years and years of doing Baker-Gordon Peels, doctors have figured out ways of doing it so you could eliminate those problems and get better results with it.
In the late 1990s, two doctors—Phillip Stone and Gregory Hetter—did extensive work on modified phenol and croton oil peels, which had varying mixtures and amounts of ingredients. They really changed a lot of the thinking of how chemical peels should be done.
Prior to that, when Baker and Gordon formulated their peel, there were many absolute dogmas associated with it. The absolute dogmas of phenol were that it was the phenol that was the active ingredient doing the peeling and that it was an all-or-none effect. And the peels got deeper with a lower phenol concentration. Their thinking was that a high concentration prevented deep penetration by denaturing the keratin and lowering the concentration, allowing it to penetrate deeper and get a deeper burn. Also, they thought that the loss of pigmentation was caused by the phenol itself. It was thought to also be extremely toxic to the heart and that toxicity was thought at one time to be uncontrollable.
The other thing they thought was that the soap [that was used in the peel] lowered the surface tension and also increased the penetration of the phenol.
The last dogma was that the croton oil was an irritant. After all these studies with Hetter and Stone, they figured out that all those old beliefs were only myths and that the truth was completely different. One of those truths is that phenol greater than 50% will peel deeper with increasing concentration. It’s the complete opposite of what they thought before.
Also, unoccluded phenol less than 35% doesn’t do anything at all. It’s not even as strong as an intermediate peel. The phenol does not have an all-or-nothing effect; it is the croton oil that is a very powerful cytotoxin resin that is the key to the peel. Minute amounts of croton oil will cause a skin burn in and of itself. By adding croton oil to the phenol and by varying the percentages, you can vary the depth of peel. The depth of the peel will increase with an increased concentration of croton oil. If you tape a peel, you are going to increase the depth of the peel.
 |
 |
| Figure 4. Application of the peel solution intraop. | Figure 5. Mixing the peel solution intraop. |
Describe the process of mixing the formula and the application technique.
In my practice, I do what I call a multilevel phenol croton oil peel. We use a basic Baker-Gordon formula but modify the amount of croton oil.
The Baker-Gordon Peel has 3 mL of phenol, 2 mL of distilled water, eight drops of septisol, and three drops of croton oil. Instead of putting in three drops, I put in two drops of croton oil. And I will do another batch with only one drop of croton oil. I now have a three-drop, a two-drop, and a one-drop formula.
In addition, I can use straight phenol that will peel even less. I have four formulas of this phenol-based peel that I can use. If there are deeper lines in an area, I can use a stronger formula. If a person’s skin is thicker, I can use a stronger formula.
When I examine the patient, I actually mark out the areas and which formulas are going to go in which part of the face. So, I may use two or three different formulas on the same face to get the same peel depth and an even result afterward.
I know that [patients with] very thin skin should not get a heavy peel because you are going to risk going too deep. The doctor should mix the formulas immediately prior to the procedure. You should never let an assistant or an associate do it. It is critical that it is mixed correctly, and you have to have the confidence that what you are using is the right combination.
I divide the face into four zones. My zone one is the perioral area, chin, and lower nose. Zone two is the cheeks and upper nose; zone three is the forehead; and zone four is the eyelids, the periorbital areas, and extending into the temples and the little strip in the preauricular area in front of the ear. Zones one through four go from the thickest skin on the face to the thinnest.
I do one area at a time and wait about 5 minutes between them, because when you put the solution on, it frosts immediately. When the frost starts to dissipate, I start the next area. I do the whole face in about an hour and 10 to 20 minutes.
It only costs about $110 for chemicals that can be used for many deep peel cases. I charge about what my competitors charge for a laser resurfacing. I charge that because of the intense follow-up I do. Across the country, chemical peels probably average about $3,000 to $5,000 per case.
 |
 |
 |
 |
 |
| Figure 4. The progression of a peel patient, left to right: Postop day 1, day 9, at 2 weeks, at 6 weeks, and at 4 months. | ||||
Who is the ideal candidate for peels?
Patients presenting with facial wrinkles and lines—rhitidosis, weathered skin, hyperpigmentation, and brown spots—are the really good candidates. Patients with smoker’s lines and deep lines around the eyes are also good candidates.
Peels are good for people of any age. It’s not the age as much as the condition. I have never seen anyone who needed to repeat a deep peel. If it is done properly the first time, it rarely needs to be repeated. That’s the beauty of it. Occasionally, you may have to touch up an area many years down the road, but it’s a rarity. As long as you get them on good skin care and good skin protection and hydration, this [treatment] maintains itself beautifully. Some of my happiest patients are my peel patients.
Resurfacing procedures do not get rid of scarring, like acne scars. What they do is try to camouflage the scarring by lessening the depth of the scar, making it smoother and flatter. It evens the complexion out and lowers the highs and lows of the scarring.
You have to be careful because any resurfacing procedure can actually make the pores look larger. It’s not going to work with all acne scarring.
What can a patient expect in the way of preop and postop care, pain, and downtime?
Preop considerations include getting a good family history and physical, and finding out about any existing medical conditions that could interfere with the healing process.
You also want to make sure there is no history of facial radiation or a thyroid cancer, because that irradiated tissue will not heal. You have to make sure they haven’t been on Accutane for a minimum of 1 year, but I prefer one-and-a-half to 2 years. Get a history of herpetic outbreaks. You don’t want them to have had any previous peels or be on Retin A, or have any exfoliating procedures prior to the peel.
Smokers are discouraged. Smoking breaks down the collagen and elastin in your skin, so you’re kind of defeating the whole purpose of going through this. Plus, you don’t want people to be coughing.
We do the procedure under conscious sedation. Patients are monitored for EKG and pulse oximeter. We cleanse the skin with septisol to make sure it’s really clean. Then, the face is degreased two or three times with acetone to ensure the peel goes on evenly. Any oils in the skin can alter the amount of penetration.
I also use Marcaine nerve blocks in the infraorbital, supraorbital, and mental nerves, which increases the comfort of the patient. The Marcaine will last about 6 or 7 hours, which is how long the patient should experience discomfort anyway. The pain is like a very bad sunburn—it waxes and wanes for about 8 to 10 hours. After that, it goes away and there is no more pain. My patients don’t take pain medication after this; it is not that painful.
When the procedure is finished, I put Eucerin cream all over the face, and that will stay on until they are done peeling. In the first 24 hours, their face will swell to twice the size of normal. Then, the fluid between the layers begins to leak out. I tell my patients that you’ll have on the white cream while the drippy, clear fluid is leaking and your face is swollen, and you’re going to look awful, but not hurt.
The swelling is usually down by 5 to 6 days; the dripping is done in about 5 days as well. Then they start peeling, but it’s all done under the white cream so the patient is unaware of the peeling.
I have my patients come in every single day, postpeel, to be checked. I do this for reassurance because the patients look strange and they need to know that what they see is what it is supposed to be. You can also catch mistakes they may be making. For the next 4 to 5 days I see them every other day; then every 3 to 4 days. Usually, a person will have to take off from work for about 2 weeks.
In addition to using the Eucerin cream, I also have them shower their faces with a fine mist or with a sprayer five to six times a day. This isn’t to wash off the cream; it is to add moisture. The water hitting the face also stimulates the skin. It usually takes between 8 and 12 days for a person to peel.
When they are done, they are going to have a bright pink skin, which is the new skin their bodies have made to replace the skin we’ve just taken off. After about 24 to 48 hours of [final] peeling, they are allowed to use makeup to cover the pinkness.
They are going to have to keep their faces moisturized, so they’re going to have to use a lot of regular moisturizer. The skin will absorb the cream like a sponge. The faster it is rehydrated the better it is going to look. I also don’t let them use sunscreen until day 20 or 21 because most sunscreens will burn the skin.
How popular is this procedure?
In the early 1990s, peels were very popular. Then in the late ’90s and early 2000s, it was dead. No one wanted to have them done, mainly due to the backlash of poor laser results. Now it’s picking up again.
What are the potential complications?
To cut down on potential complications, you have to choose your patients carefully. The best candidate is someone with fair or light skin, light-colored eyes, and light hair.
With patients with an olive complexion or solar damage with a lot of freckling in their skin or darker pigmentation, you have to be a little more careful but you can still peel them.
Dark-skinned people or Asians are not good candidates at all. They have an increased chance for uneven complexion, hyperpigmentation, and hypopigmentation.
If you take someone who has extensive sun damage and you just peel their face, you will see a line of demarcation.
Patient selection is critical. You also want to educate the patient prior to the procedure, including showing them photos of how they will look right after, as well as throughout the days and weeks after the procedure. I also let them talk to other patients who have had peels.
You don’t want to do regional peels just around the mouth or eyes—you want to do the entire face. Complications can occur when the surgeon does not prepare his or her own solutions. You want to stay away from people with lax lids who have scleral show.
All of my patients are given Valtrex to prevent herpetic outbreaks; they also get antibiotics. The biggest complication after this treatment is sun exposure, because that will cause hyperpigmentation. Our complication rate is less than one percent. These peels can be done any time of the year.
Why is the chemical peel the gold standard?
It is what everyone bases their results on, and it was the initial resurfacing procedure. Done properly and correctly, it gives the best results. Laser companies always compare to chemical peels.
James R. Shire, MD, FACS, is a facial plastic surgeon specializing in aesthetic surgery of the face. He been performing chemical peels for nearly a quarter century. He is board certified by the American Board of Facial Plastic and Reconstructive Surgery and the American Board of Otolaryngology.
Amy DiLeo is a contributing writer for PSP. She can be reached at [email protected].