 |
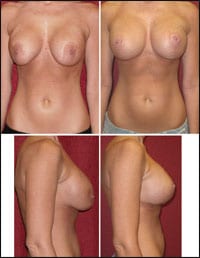
| Figure 1. A 34-year-old female 4 weeks following short scar (vertical) mastopexy along with removal of submammary saline implants and total capsulectomies. New silicone gel implants were placed in a total submuscular position. As one can see, an attempt had been made to use a donut or Benelli mastopexy, which the patient disliked because of the classic problems seen preop: the areola were stretched oblong and widened, flattening occurred on the breast mound, and redundant tissue was left hanging over the implants. The vertical mastopexy corrected all of the above and allows for a stable decrease in areolar diameter. |
Short scar techniques for lifting a breast usually refer to procedures that avoid a long inframammary fold incision that is characteristic of a Wise or inverted T pattern mastopexy.
The Lejour technique of vertical scar incision pattern popularized the idea of avoiding a horizontal scar during mastopexy (or breast reduction). Around the same time, Benelli was intensely arguing for a “round block” technique for mastopexy that uses a periareolar incision with no vertical or horizontal scar components.
Since the early 1990s, much has been written to describe a vertical or “short scar” mastopexy, and the arguments will likely continue over what is the best short scar lift.1-5
Regardless of the particular technique, cosmetic surgeons strive to create a “perfect” breast shape with minimal scarring and complications.
A patient’s view of what appears aesthetic may differ from our own, and we may alter our treatment plan accordingly. One simple short scar technique will never suffice for all patients, and it is critical to understand all major mastopexy techniques if we are going to try to satisfy all of our patients.6-10
For example, large breast reductions (more than 600 grams) can be done with a vertical scar technique. However, the bunching created initially at the base of the incision may be more offensive to some patients than adding a short horizontal scar.
DEALING WITH SCARS
Typically, a short scar in the midportion of the inframammary fold is not offensive to most patients, but extending the horizontal incision within 3 cm of the sternal midline or laterally along the thorax often results in objectionable scars.
These extended inframammary fold scars are potentially visible when the patient wears a small bathing suit or low-cut dress. As such, the use of long inframammary incisions should be avoided if at all possible, including during extremely large breast reductions.
Liposuction of the excess lateral breast fullness is a good tool to help contour the final breast shape and shorten the lateral incision.
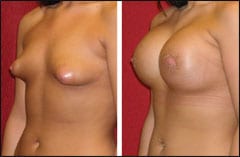 |
| Figure 2. A 22-year-old female 4 weeks after a periareolar (Benelli Type) mastopexy, parenchyma release, and placement of subpectoral saline implants. A thin layer of Scarguard® gel can be seen on the incision line to help the final aesthetic result. Typically, this ultrashort scar technique should be avoided if lifting breast parenchyma is required, since the periareolar lift does little to truly “lift” a breast. However, the patient seen here had constricted, tubular breasts that greatly benefitted from the flattening effect of a donut-type mastopexy. |
 |
| Figure 3. A 32-year-old female 5 months following a mastopexy only. The procedure was planned for a vertical lift and was converted during surgery to a short scar mastopexy with a 4-cm scar at the fold. Performing the majority of the procedure using vertical mastopexy principles helped maintain adequate project and allowed for only a very small amount of additional skin excision at the fold. Therefore, minimal extension is made horizontally, yet bunching of inferior tissue is avoided. |
Patients seeking the ideal breast shape and size are not always perfect candidates for a simple mastopexy or augmentation alone. Yet, many lose their enthusiasm about the procedure they may have wanted for years when they realize that a breast lift is needed for the best results, and that permanent breast scars are part of this procedure.
Cosmetic surgery of the ptotic breast often involves treatment of breast hypoplasia as well as ptosis. Therefore, many women, because of genetic factors or following childbirth and weight loss, have a combination of breast problems that mandates mastopexy and augmentation.
MASTOPEXY PLUS IMPLANTS
An isolated mastopexy or basic augmentation can be relatively straightforward in select patients. However, combining mastopexy with breast implants during the same surgery can be a menacing and risky task for even the most experienced surgeon (Figure 1). Most patients, though, will choose a simultaneous procedure versus a staged one, even when informed of the added risk.
The Regnault breast ptosis classification system was developed in 1976 to demonstrate various breast shapes that help guide a surgeon’s decision-making process with regard to augmentation and mastopexy.
Unfortunately, the grade of ptosis is only one small aspect of determining the ideal procedure for each patient.
A simple or strict dogmatic method for simultaneous mastopexy and augmentation does not exist (Figure 2). Cosmetic surgery of the ptotic breast must bring out the artist in the surgeon.
A prudent surgeon must always weigh the risk versus the benefit of performing a simultaneous augmentation and lift compared to staging the procedure (Figure 3). In many cases, the added volume of an implant may benefit the patient not only with increased upper-pole fullness, but also with shorter scars because less skin excision is required. Of course, the method itself is more challenging than a staged procedure of lift followed by augmentation a few months later.
The simultaneous augmentation and mastopexy potentially can provide shorter scars, but at the cost of more tension on the incision sites. This could lead to wider scars and increased risk of wound dehiscence.
PEARLS TO CONSIDER
Think about the following when determining mastopexy with or without implants:
Major ptosis with a nipple to inframammary fold distance greater than 10 cm will be a challenge to treat without a horizontal incision, unless the surgeon is extremely experienced in a Lejour mastopexy or using a very large implant. Ultimately, controlling the fold position and nipple-to-fold distance is more essential than trying to shorten a scar, particularly in the severely ptotic breast.
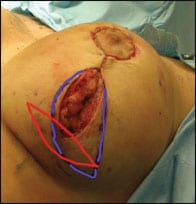 |
| Figure 4. Many conversion options exist if the nipple-to-fold distance appears unlikely to be maintained adequately with a standard vertical mastopexy. In this example, the purple lines demonstrate an “L” or oblique tissue excision to help control scar length versus the red lines, which demonstrate a simple horizontal extension of the scar. In the case of a standard vertical scar or oblique incision, characteristic fullness at the apex often develops and can be avoided by excising subcutaneous tissue inferiorly to thin the flap the last 3 centimeters. |
When excessive bunching occurs when using the short scar technique, adding a short horizontal incision or lateral curve at the base of a vertical mastopexy can help improve results (Figure 4).
In many ptosis cases, an isolated periareolar mastopexy cannot produce any noteworthy parenchymal breast lifting and often leads to an unaesthetic shape.
Dense, heavy breasts are more difficult to treat with short scars because of the tendency to leave excess inferior pole tissue. This can lead to recurrent ptosis if not removed or redistributed adequately.
Early in one’s cosmetic breast surgery career, one may at times be overly conservative about the incision choice. Also, inadequate excision of breast parenchyma and fat during simultaneous mastopexy and augmentation may lead to less-than-ideal results.
This can be particularly true for the type 2 or 3 ptosis patient who is a natural C or D cup and desires to be “about the same size, just more rounded and perky.” These patients can be very difficult to please because they want the appearance of breasts obtained from implants that have augmented their once flat-chested friend. They hope for the shortest and best-looking scars possible when they are informed that a lift is required.
A vertical mastopexy can often be used in this situation to perform a breast reduction and “reaugmentation” with implants, in order to achieve the aesthetic result the patient desires. Basically, the more percentage of natural breast tissue, the more natural the breast.
Often, more ptotic relapse will occur in women with naturally large, dense breasts compared to large implants in lighter-weight breasts. Reducing natural breast tissue weight in exchange for implant volume will help decrease that chance for recurrent ptosis. However, this approach can be more risky to perform.
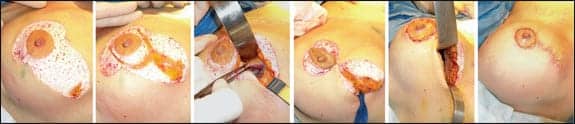 |
| Figure 5. Sequential steps in a classic short scar (vertical) mastopexy are demonstrated with A and B immediately following deepithelialization of the initial cut to create a superior-medial pedicle and vertical incision for plication of breast pillars or implant placement. (C) demonstrates early elevation of a submuscular pocket; (D) preliminary closure seen here at the trifurcation and 12-o’clock position helps with symmetry and general orientation; (E) retraction for implant placement is demonstrated; and (F) final closure seen requires some pleating or minor bunching at the inferior extent of the incision in order to maintain a proper nipple-to-fold distance and to avoid placement of a horizontal scar. |
ADDITIONAL ADVANTAGES
The short scar vertical mastopexy has other advantages in addition to scar size, particularly compared to a periareolar incision only.
Patients who have large areolas and want a smaller diameter during augmentation and mastopexy will benefit from the addition of a short vertical incision. The addition of the vertical limb helps control tension away from the periareolar scar and allows the surgeon to maintain a smaller areolar diameter.
Conversely, using a traditional donut mastopexy during simultaneous augmentation carries a high chance of areolar diameter and scar widening even months after the surgery.
|
See also “A New Breast,” by George John Bitar, MD, and Vinod K. Chopra, in the December 2007 issue of PSP. |
The vertical mastopexy technique varies with most surgeons (Figure 5). However, one can take steps to avoid unnecessary problems. The vertical mastopexy can potentially create a nipple position that appears high compared to an inverted T technique.
Preoperative planning with marks and measurements are best kept conservative when first getting comfortable with this method. The inferior apex of the planned excision should be made at least 1.5 cm above the planned new inframammary fold, to avoid the vertical incision being visible below the fold at final closure.
Additional skin and tissue can always be removed later in the surgery as required, but it is hard to put it back if you remove too much from the beginning.
As with any surgical technique, you should use whatever will give the best result with the least risk. The short scar vertical mastopexy can be a very rewarding procedure for both patient and surgeon, and can be used in many circumstances depending on the surgeon’s comfort level and experience.
Angelo Cuzalina, MD, DDS, is in private practice in Tulsa, Okla, and is the director of a Cosmetic Surgery Fellowship program accredited by the American Academy of Cosmetic Surgery. He can be reached at [email protected].
Regnault Classification of Breast Ptosis
Pseudoptosis
Nipple is above the fold, and loose breast parenchyma hangs below the IMF
Grade 1 Ptosis
Nipple is at the fold
Grade 2 Ptosis
Nipple is 1 to 3 cm below the fold, but above the lowest contour of the breast
Grade 3 Ptosis
Nipple is located at the lowest contour of the breast more than 3 cm below the fold
Other Treatment Planning Considerations
Breast density—Pillar plication is limited with fatty breast
Tightness of tissue at the inframammary fold—To avoid a “double bubble” deformity
The patient’s vision of the ideal breast—Especially related to roundness or natural contours
The amount of size change required—Care must be taken not to over-resect skin as implant size increases
Areolar diameter—Desired areolar width
Breast dimensions—In particular, nipple-to-fold distance and base width
REFERENCES
- Lejour M. Evaluation of fat in breast tissue removed by vertical mammoplasty. Plast Reconstr Surg. 1997;99:386.
- Lejour M, Abboud M. Vertical mammoplasty without inframammary scar and breast liposuction. Perspect Plast Surg. 1990;4:67.
- Benelli LA. New periareolar mammoplasty: Round block technique. Aesth Plast Surg. 1990;14:93.
- Lassus C. Breast reduction: Evolution of a technique: A vertical single scar. Aesth Plast Surg. 1989;11:107.
- Felicio Y. Periareolar reduction mammoplasty. Plast Reconstr Surg. 1991;88:789-798.
- Courtiss EH. Reduction mammoplasty by suction alone. Plast Reconstr Surg. 1993:1276.
- Goes JCS. Ultrasound-assisted lipoplasty (UAL) in breast surgery. Aesth Plast Surg. 2002;26:1-9.
- De Longis E. mammoplasty with an L-shaped limited scar and retropectoral dermopexy. Aesth Plast Surg. 1986;10:171-175.
- Matarasso A, Courtiss EH: Suction mammoplasty: The use of suction lipectomy to reduce large breasts. Plast Reconstr Surg. 1991;87:709.
- Marchac D, De Olarte G. Reduction mammoplasty and correction of ptosis with a short inframammory scar. Plast Reconstr Surg. 1982;69:45.



