 |
According to extrapolations based upon the 2000 United States Census Bureau Survey, the current population of the United States exceeds 300 million people.1 Although most surveyed identified themselves as descendants of European immigrants, more than one third of people living in the United States associated themselves with minority groups. The proportion of minorities continues to climb for a variety of reasons, and will continue to increase, as evidenced by the fact that more than 45% of American children under the age of 5 are in minority groups.
In the past, aesthetic surgery has been vastly more popular in the western world. However, the recent economic development and strength of many nonwestern countries have created concomitant rises in disposable income. This, coupled with greater cultural acceptance of aesthetic modification, has contributed to a surge in aesthetic procedures such as rhinoplasty. The globalization of economies and the ever-present images of beauty portrayed by the world media portend that aesthetic surgery will continue to enjoy widespread popularity and growth in the years to come.
All aesthetic surgery is based on refining anatomic characteristics within specific individuals. However, generalization regarding the qualities specific to particular ethnic backgrounds can help guide the surgeon toward excellent outcomes in ethnic rhinoplasty. For the purposes of this article, we will place our emphasis on three specific groups whose members comprise more than 30% of the US population: Asian, African American, and Hispanic.
A common misconception regarding ethnic rhinoplasty is the notion that nonwhite patients seek rhinoplasty to look more like whites. Research has shown this to be unfounded.
Baker and Krause reported a study in which the vast majority of nonwhite rhinoplasty patients did not seek to look “whiter” postoperatively, but instead requested nasal refinement that was harmonious with the rest of their face and did not obliterate their ethnic identities.2 Moreover, in the cultures of most Asian countries, the ideal of a high, narrow nasal bridge and base along with refined alar contours has been present long before exposure to western populations.3
This is in keeping with the notion that certain nasal characteristics are appealing cross-culturally. The nasal dorsum should be straight—not overly convex or concave—and relatively narrow; the tip should have definition and should project slightly from the nasal dorsal height; and the base should be proportional to dorsal width without being overly narrow or wide.
Most importantly, the postoperative nasal appearance should be proportional to the rest of the facial characteristics. Ethnic incongruity should be avoided.
The Anatomy of Ethnic Noses
For the sake of simplicity, we will discuss the characteristics of the “ethnic” nose using generalizations specific to African Americans, Asians, and Hispanics, while acknowledging the presence of deviations from these anatomic stereotypes. Interestingly, however, these three minority populations—although extremely diverse in their overall physical appearance—exhibit remarkable similarities with respect to nasal anatomic characteristics (Table 1).
Table 1. Nasal Anatomical Characteristics in Specific Ethnic Groups |
|||
|
Characteristic |
African American |
Asian |
Hispanic |
|
Skin |
Thick |
Moderate to thick |
Moderate to thick |
|
Tip support |
Weak |
Weak |
Weak |
|
Dorsum |
Wide, low |
Shallow, depressed |
Wide, low |
|
Tip |
Underprojected, |
Underprojected, |
Underprojected, |
|
Nasal base |
Broad |
Moderate to broad |
Moderate to broad |
|
Nasolabial angle |
Acute |
Moderate |
Moderate |
|
Columella |
Short |
Moderate retraction |
Short |
|
Alar cartilage |
Wide, weak |
Moderate |
Variable |
In general, the ethnic nose features a wide, flat dorsum with depression at the nasion. The nasal tip tends to be poorly defined and underprojected with poor structural support, and often contributes to an acute or neutral nasolabial angle.
Alar flaring and widened nasal bases may be more frequently seen in African Americans and can be prominent enough to extend beyond the confines of a vertical line drawn from the medial canthi. Also in contrast to the Caucasian nose, the ethnic nose features a thick, sebaceous skin envelope and a relative paucity of septal cartilage—a deficiency that must be accounted for if the operation calls for grafting.3–8
Preoperative Evaluation
Before & After |
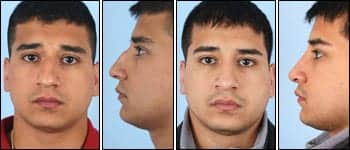 |
| Figure 1. This 29-year-old Hispanic patient is shown before and 1 year after undergoing rhinoplasty. |
During the initial consultation, the surgeon should ascertain whether the patient’s goals and expectations are realistic. A realistic goal of ethnic rhinoplasty would be to refine but not obliterate “ethnic” characteristics, so that the postoperative nose blends harmoniously with the rest of the patient’s facial features. Surgeons should be cautious with patients whose goal is to eliminate all facial features specific to their ethnicities. The prospect of postoperative dissatisfaction in these patients is extremely high.
Before considering any elective surgery, a thorough history and physical should be performed. Specifically, it is important to inquire about any previous history of nasal surgery or trauma. Because of the typical paucity of cartilage in the ethnic nose, previous septoplasty or rhinoplasty may have used most, if not all, of the possible autologous grafting material within the nose, thereby forcing the surgeon to seek other tissues (or synthetic materials) for grafting purposes. If this is the case, the ears and septum should be inspected for the presence or absence of cartilage.
A detailed internal and external inspection of the nose should be performed to establish what changes are possible with surgery. A functional assessment of the nose should not be deferred. The septum should be evaluated with respect to septal deflections, perforations, and signs of previous cartilage harvest.
Turbinate size and the internal nasal valve should also be inspected so that specific intraoperative maneuvers may be made to correct nasal obstruction. The strengths of the ala and external valve should also be assessed. In addition, a Cottle maneuver may be helpful to assess the nasal airway.
With respect to the tip, the texture of the skin envelope and the quality of the subcutaneous fibrofatty pad should be inspected visually and with palpation. To help predict the need for grafting, the size and strength of the tip’s cartilaginous support mechanism should also be evaluated. In addition, tip projection, rotation, and definition, as well as the nasolabial angle, should be assessed to predict which operative maneuvers may be necessary.
Another key element of the preoperative examination is evaluation of the dorsum. The dorsal bony and cartilaginous contributions are palpated, and the contour of the nose is carefully inspected. On the basis of this exam, the need for augmentation via grafting techniques can be evaluated.
If a large amount of grafting material will be needed, and the surgeon prefers autologous cartilage, costal cartilage grafts may be necessary. If this is the case, the use of costal cartilage and its attendant risks and benefits should be discussed with the patient. Similarly, if the surgeon prefers alloplastic materials, risks such as infection and extrusion should be discussed and included in the informed consent.
Preoperative photodocumentation should be performed in all patients before they undergo rhinoplasty. In addition, some practitioners find it helpful to perform computer modeling in order to ground patient expectations. However, it must be emphasized that computer simulations of postoperative results are only an approximation of the final result and depend heavily on the surgeon’s skill and his or her realistic use of the software.
Operative Technique
Performing rhinoplasty in ethnic patients requires facility with operative techniques that should be within the armamentarium of the well-trained facial plastic surgeon. Based on common, specific deformities in the ethnic nose, certain areas of focus deserve special mention: increasing tip projection and definition, dorsal augmentation, and alar base reduction.
Before & After |
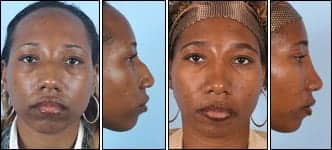 |
| Figure 2. This 30-year-old African American patient is shown before and 2 years after her rhinoplasty. |
After the topical application of 4% cocaine for nasal decongestion and placement of oxymetazoline-soaked pledgets, 1% lidocaine with 1:100,000 epinephrine is infiltrated subcutaneously for anesthesia and hemostasis. Adequate time is allowed to pass to achieve maximal vasoconstriction, at which time cartilage from the rib or concha (if necessary) can be harvested.
Once the pledgets are removed, a septoplasty through a Killian’s or hemitransfixion incision can also be performed to remove septal deflections and to obtain septal cartilage graft material. Subsequent inferior turbinate outfracture and reduction technique can be performed to increase nasal airway patency.
We prefer an open approach with ethnic rhinoplasty to accurately diagnose anatomic deformities intraoperatively and to ensure the accurate placement of grafts. Marginal incisions are made bilaterally with subsequent blunt elevation of skin envelope from the lower lateral cartilages. Then, our transcolumellar incision is made in a stairstep configuration, although the common inverted V incision exhibits similar, almost imperceptible scarring postoperatively.
Accurate closure with either incision design will yield good results. Further elevation of the skin envelope is performed over the upper lateral cartilages with superior extension in a subperiosteal manner over the nasal bones up to the nasion. Maintaining the thickest possible skin–soft tissue envelope will preserve vascular and lymphatic channels, creating a drier operative field and less postoperative edema. This dissection should provide the surgeon with maximal visualization of the nasal anatomic substructure.
Before & After |
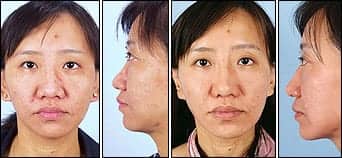 |
| Figure 3. This 27-year-old Asian patient is shown before and 1 year after undergoing rhinoplasty. |
The ethnic nasal tip often has inadequate definition, projection, and support. Therefore, several operative maneuvers are used to address these deficiencies. Tip definition can be improved by using cephalic trimming of the lower lateral crura. In addition, the use of interdomal and intradomal suturing techniques can refine the often amorphous appearance of the ethnic nasal tip.9
Because the skin of the ethnic nasal tip can feature very thick fibrofatty tissue, these maneuvers, as well as placing other types of grafts within or near the tip (such as tip grafts or lateral crural grafts), can be well camouflaged. Accordingly, in noses with an extensive amount of soft tissue, conservative reduction of the supratip and tip globular tissue can be tolerated. Support can be improved by using a columellar strut. Our preference is to use septal cartilage grafts that are placed between the medial crura and fixed with absorbable sutures.
Examples of typical successful rhinoplasties are shown in Figures 1–3.
Dorsal Augmentation Issues
Perhaps no area in rhinoplasty has generated such vociferous debate as dorsal augmentation. Because of the relative underdevelopment of the dorsum in ethnic populations, surgeons have devised several ways to “build up” the dorsum by using an array of materials. Much of the controversy centers around the use of alloplastic materials or autologous tissue.
Before & After |
 |
| Figure 4: Example of an alar wedge resection to narrow the nasal base. |
Long preferred in Asia for augmentation rhinoplasty, dorsal grafts made of silicone rubber, expanded poly(tetrafluoroethylene), and porous high-density polyethylene have been popular because of their ease of use and ability to achieve satisfactory aesthetic results. However, the use of alloplasts is burdened by the relatively high complication rate of about 9%.
Complications that require implant removal are displacement, extrusion, and infection.10 However, McCurdy contends that in his 3-decade surgical experience with augmentation rhinoplasty, no method of dorsal augmentation has proven to have better aesthetic results than the L-shaped silicone rubber implant that addresses the dorsum and the tip.3 He also argues that the reported complication rates with alloplasts are overestimated and that the early poor experience with the use of alloplasts by surgeons in the West may have been a by-product of poor technique and the unforgiving characteristics of early alloplastic materials.
Still, many prominent rhinoplasty surgeons in the West eschew the use of alloplasts, instead favoring autologous material such as costal cartilage and temporalis fascia with crushed cartilage (the so-called “Turkish delight”11), despite the associated donor-site morbidity and risks associated with graft harvest.
 |
| See also “Ethnic Rhinoplasty” by Oleh Slupchynskyj, MD, in the September 2005 issue PSP. |
The advantages of autogenous grafts are decreased incidence of extrusion or infection and the improbability of permanently harming the overlying soft tissue and skin envelope.12 Other homologous materials such as irradiated cadaveric rib cartilage and acellular dermal grafts have been used with varying success,13 but the use of these materials is not widespread because many surgeons believe that such materials have limited life spans due to possible graft resorption.
The dorsum of the ethnic nose is deficient and shallow, but not excessively wide when compared to the rest of the face. The ethnic face often features a widened intercanthal distance compared with that of Caucasians. Therefore, osteotomies to narrow the dorsum may produce an overly thin nose that is ethnically incongruous and unbalanced with the rest of the face.
Therefore, some surgeons advocate a conservative approach toward osteotomies14 and rarely use them in ethnic rhinoplasty. They believe that augmentation alone is sufficient for superior aesthetic results.
Rohrich uses a more specific surgical algorithm: He recommends osteotomies only if the width of the nose is greater than 80% of the intercanthal distance.15 Regardless of the approach, narrowing of the upper third of the nose should be approached cautiously and must be proportional to maneuvers that will affect the nasal tip and base.
Toward the conclusion of the rhinoplasty, and after nasal-tip support and projection have been established, we critically evaluate the need for maneuvers that can reduce the alar width, diminish nasal flaring, or both. This is done last because increasing nasal projection can decrease the apparent amount of tissue that must be removed with alar base resection (Figure 4). Occasionally, this obviates the need for operative manipulation of the base entirely.
Many different techniques have been advocated with respect to excision design. In all types of excisions, however, great care must be taken during closure, especially if the nostril sill is violated or telltale notching can occur with healing.
Once again, the use of these maneuvers should be cautious, because overaggressive narrowing of the base and ala has a strong chance of creating ethnic incongruity and facial disharmony, especially in African Americans. Reversing alar base excisions is very difficult; therefore, this procedure should always be approached with a conservative plan. It is much easier to excise more tissue than to try and add composite grafts later.
Ethnic rhinoplasty is an extremely challenging surgical procedure. It requires a strong understanding of ethnic nasal anatomy, familiarity with the “ideal” nasal shape, and facility with various operative maneuvers. The result of an ethnic rhinoplasty should create a nose that is well-balanced with the patient’s face while keeping ethnic identity in place.
Michael M. Kim, MD, is a fellow in the division of Facial Plastic and Reconstructive Surgery, Department of Otolaryngology– Head and Neck Surgery, The Johns Hopkins Hospital, Baltimore. He can be reached at .
Ira D. Papel, MD, FACS, is board-certified in facial plastic surgery and otolaryngology–head and neck surgery. He is in private practice in Baltimore and is an associate professor at Johns Hopkins University. He can be reached at .
References
- US Census Bureau. Available at: www.census.gov. Accessed August 14, 2007.
- Baker HL, Krause CJ. Update on the negroid nose: An anatomic and anthropometric analysis. In: Ward PH, Berman WE, eds. Plastic and Reconstructive Surgery of the Head and Neck: Proceedings of the Fourth International Symposium. St Louis, Mo: Mosby-Year Book; 1984:1.
- McCurdy JA. Asian rhinoplasty. In: McCurdy JA, Lam SM, eds. Cosmetic Surgery of the Asian Face. 2nd ed. New York: Thieme; 2005:129–145.
- Cobo R. Mestizo rhinoplasty. Facial Plast Surg. 2003;19:257–268.
- Nolst Trenite GJ. Considerations in ethnic rhinoplasty. Facial Plast Surg. 2003;19:239–245.
- Rohrich RJ, Muzaffar AR. Rhinoplasty in the African American patient. Plast Reconstr Surg. 2003;111:1322–1339; discussion 1340–1341.
- Romo T III, Abraham MT. The ethnic nose. Facial Plast Surg. 2003;19:269–278.
- Wang TD. Non-Caucasian rhinoplasty. Facial Plast Surg. 2003;19:247–256.
- Papel ID. Interlocked transdomal suture technique for the wide interdomal space in rhinoplasty. Arch Facial Plast Surg. 2005;7:414–417.
- Deva AK, Merten S, Chang L. Silicone in nasal augmentation rhinoplasty: A decade of clinical experience. Plast Reconstr Surg. 1998;102:1230–1237.
- Erol OO. The Turkish delight: A pliable graft for rhinoplasty. Plast Reconstr Surg. 2000;105:2229–2241; discussion 2242–2243.
- Toriumi DM. Autogenous grafts are worth the extra time. Arch Otolaryngol Head Neck Surg. 2000;126:562–564.
- Murakami CS, Cook TA, Guida RA. Nasal reconstruction with articulated irradiated rib cartilage. Arch Otolaryngol Head Neck Surg. 1991;117:327–330; discussion 331.
- Matory WE Jr, Falces E. Non-Caucasian rhinoplasty: A 16-year experience. Plast Reconstr Surg. 1986;77:239–252.
- Rohrich RJ. Rhinoplasty in the Black Patient. Boston: Little, Brown; 1993.




