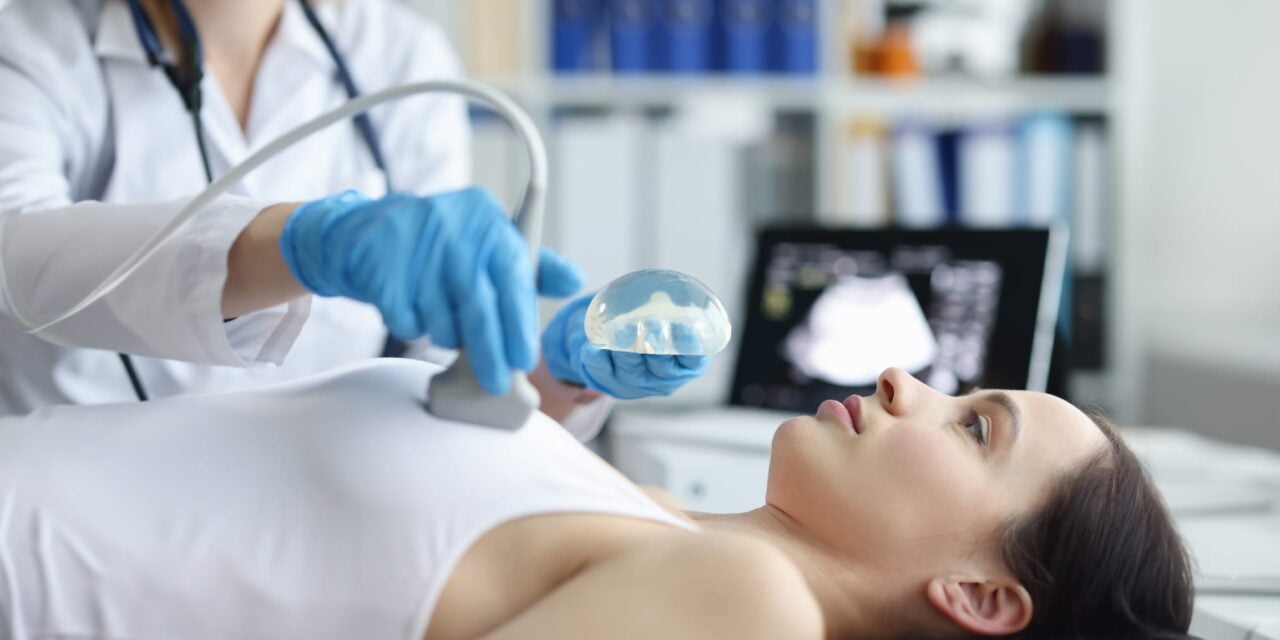
The Women and Equalities Committee’s report highlights patient safety failures tied to unregulated surgical and non-surgical cosmetic procedures, including gaps in data collection, informed consent, and clinical oversight.
The UK’s House of Commons Women and Equalities Committee published a wide-ranging report on Feb 18, 2026, calling on the government to mandate participation in the national breast implant registry, restrict high-risk non-surgical cosmetic procedures to qualified medical professionals, and commission new clinical and longitudinal research into the health impacts of breast implants—including the poorly understood condition known as breast implant illness (BII).
The report, titled Cosmetic Procedures and comprising the committee’s 11th report of Session 2024–26, examined patient safety across both surgical and non-surgical cosmetic interventions in the UK. Among its central findings: regulation has not kept pace with rapid industry growth, leaving patients—particularly women—exposed to serious harm.
Data Gaps Undermine Informed Consent
A central concern in the report is the Breast and Cosmetic Implant Registry (BCIR), established in October 2016 following the Poly Implant Prothèse (PIP) breast implant scandal. Despite its creation, the registry remains voluntary and currently captures data on approximately 80% of breast implant procedures.
According to the report, the absence of mandatory reporting and regularly published outcome data makes it impossible for surgeons to provide patients with complete risk information before surgery. Carl Heneghan, director of the Centre for Evidence-Based Medicine at the University of Oxford, told the committee that this situation effectively prevents patients from giving fully informed consent.
“There are lots of uncertainties because of our failures to collect and report an evidence base, as we do for many other implants; the national joint registry for hips and knees does a much better job monitoring the failings of metal hips,” Heneghan says in the report. “My perspective is that because this is considered a cosmetic intervention, it is not an issue that the NHS takes seriously. However, we are in a world now where the complications are increasing, and we have a duty to do something about that in terms of collating the evidence and reporting it appropriately.”
The committee recommended that the government mandate recording of all breast implant and explant procedures—including adverse outcomes—in the BCIR by the end of 2026, with outcome data published annually by implant type. It also recommended a mandatory cooling-off period of at least two weeks between initial consultation and surgery.
PIP Scandal Exposes Lasting Surveillance Failures
The report revisits the PIP scandal, in which an estimated 47,000 women in the UK received breast implants manufactured with fraudulently substituted, low-grade silicone by French company Poly Implant Prothèse. The implants were banned in 2010 after evidence emerged of significantly elevated rupture rates—approximately two to six times higher than standard implants, according to a 2012 expert group convened by the Department of Health.
A 2013 study of 676 explanted PIP implants found a rupture rate of 35%, with 144 ruptured implants removed from 119 patients.
Despite official assurances from the Medicines and Healthcare products Regulatory Agency (MHRA) that PIP implants pose no greater long-term health risk than other implants, the committee heard conflicting expert testimony. Michael Coleman, professor of toxicology at Aston University, described the agency’s position as “ludicrous,” citing evidence that silicones and siloxane compounds released from ruptured implants persist in patients’ bodies for years and may stimulate immune system activity linked to both BII and Breast Implant-Associated Anaplastic Large Cell Lymphoma (BIA-ALCL).
“Even if the implants are removed, silicones from the implants can be detected in women’s blood for years afterwards,” Coleman is cited as saying in the report. “The silicones enter the body and leave very slowly indeed. So the idea that this is not a problem is simply wrong.”
The Medicines and Healthcare products Regulatory Agency’s chief safety officer, Alison Cave, maintained the agency’s position: “We have no current evidence that PIP implants carry greater risk of either cancer or other symptoms than any other breast implant.”
The committee concluded that official assurances appear based on limited long-term research and fail to account for the mental health burden on affected women. It recommended that the new post-surveillance regime for breast implants include regular testing of approved products to detect any substitution of materials—the failure that allowed the PIP fraud to persist for years undetected.
BIA-ALCL and Emerging Malignancy Concerns
As of Dec 31, 2024, the MHRA had received 114 confirmed reports of BIA-ALCL in which breast implant surgery occurred in the UK, with an estimated incidence of 1 per 12,187 implants sold. BIA-ALCL is a rare cancer of the immune system—distinct from breast cancer—first defined as a lymphoma variant by the World Health Organization (WHO) in 2016. Globally, nearly all of the approximately 1,100 reported cases have been associated with textured implants.
Prabath Nanayakkara, professor of acute internal medicine at Amsterdam University Medical Center, cautioned the committee that BIA-ALCL is likely underreported. “The problem with BIA-ALCL is that you have to look for it to find it. When most private clinics remove the implant and remove the capsule, they do not check it under a microscope. So there is definitely an under-reporting of ALCL,” he says in the report.
The committee also noted that in March 2023, the US Food and Drug Administration (FDA) flagged the emergence of Breast Implant-Associated Squamous Cell Carcinoma, describing it as “a rare but potentially aggressive epithelial-based tumor that appears to be associated with breast implants and emanates from the breast implant capsule.” The FDA reported awareness of 19 cases at that time and called for increased awareness and reporting.
The UK has not banned textured implants, in contrast to France and Australia, citing low absolute cancer risk and clinical advantages such as reduced implant migration and lower risk of scar capsule formation. Instead, UK policy relies on informed patient consent and mandatory clinician disclosure of BIA-ALCL risk.
Breast Implant Illness: An Unrecognized but Reported Condition
The committee devoted significant attention to BII, a cluster of symptoms—including fatigue, joint pain, cognitive difficulties, hair loss, depression, and gastrointestinal problems—reported by some patients following implantation. BII is not formally recognized as a medical diagnosis by the WHO and has no validated biomarker.
The MHRA told the committee it has received approximately 1,000 reports since 2008 that could fall under the description of BII, representing roughly 0.5% of operations.
Nanayakkara described the clinical experience of affected women. “Most patients who come to us are frustrated and angry, and I understand that because they have been sick for, let us say, 10 years. These women lose their jobs, they lose their relationships, they are divorced, they are about 50 years old, and they have nothing,” Nanayakkara says in the report.
A 2022 study cited in the report found that explantation led to “significant symptom relief in approximately two-thirds of patients suspected of having BII,” though the mechanisms behind improvement remain poorly understood. Research published in January 2025, which examined FGF-19 levels following explantation in women with BII, was noted as making “potentially valuable observations” while calling for further investigation.
Coleman told the committee that women with pre-existing autoimmune conditions—including asthma—may be at elevated risk and are not being adequately warned: “Women are not properly informed of the risks of implants in terms of triggering an almost unending engagement with their own immune systems.”
The committee recommended that the government commission a mix of clinical and longitudinal research on breast implant health impacts, with particular attention to patients with pre-existing autoimmune conditions and the systemic effects of siloxane exposure. It also recommended that the Department of Health and Social Care alert primary care providers to the potential link between autoimmune conditions and breast implant symptoms, to prevent patients from being dismissed.
Non-Surgical Procedures: A Regulatory “Wild West”
Beyond surgical implants, the report addressed the largely unregulated market for non-surgical cosmetic procedures—defined as procedures not requiring incisions, such as injectable botulinum toxins, dermal fillers, laser therapy, and chemical peels. The Department of Health and Social Care estimates 900,000 botulinum toxin injections are performed in the UK annually.
The committee described the current environment as a “wild west,” with documented reports of procedures occurring in Airbnbs, hotel rooms, garden sheds, and public toilets. In June 2025, 28 individuals in northeast England were hospitalized after developing potentially fatal botulism following anti-wrinkle injections. Save Face, a government-approved register of qualified aesthetic practitioners, reported assisting more than 15,000 members of the public with adverse outcomes since 2014.
Particular concern centered on liquid Brazilian butt lifts (BBLs), a non-surgical buttock augmentation procedure in which dermal fillers are injected to augment volume. In September 2024, Alice Webb became the first person in the UK reported to have died following a liquid BBL. Save Face reported assisting more than 700 women who experienced sepsis or required corrective surgery following similar procedures.
The committee recommended the government immediately restrict liquid BBLs and liquid breast augmentations to appropriately qualified medical professionals—a move it acknowledged would function as a de facto ban given most credentialed practitioners refuse to perform them. A broader licensing system covering lower-risk “green” and “amber” category procedures should be introduced within the current Parliament, the committee stated.
Training and Certification Gaps in Surgical Practice
On the surgical side, the report highlighted that any physician on the UK medical register can legally perform highly invasive cosmetic operations—including breast augmentation, rhinoplasty, facelifts, and liposuction—in the private sector, regardless of specialty training.
Nigel Mercer, a consultant plastic surgeon and former president of both the British Association of Aesthetic Plastic Surgeons and the British Association of Plastic, Reconstructive and Aesthetic Surgeons, told the committee, “In the United Kingdom, I cannot work as a GP by law, but a GP or any doctor with minimal training in surgery is allowed to perform invasive cosmetic surgery. We would not allow a GP, or a doctor with little surgical training, to perform neuro or cardiac surgery. But the GMC (General Medical Council) and the law have double standards when it comes to cosmetic treatments, including surgery.”
The Intercollegiate Cosmetic Surgery Certification Scheme, established in January 2017 following the Keogh Review, addresses some of these gaps but remains voluntary. The committee recommended requiring all practitioners performing invasive cosmetic surgery to hold appropriate board certification for the specific procedures they undertake.
ID 296807992 © Kuprevich | Dreamstime.com