Paul S. Cederna, MD, discussing nerve regeneration.
Paul S. Cederna, MD, has the type of job that can only be described in one word: cool. The work he is doing in his University of Michigan lab is so cool that he may actually be able to transform average human beings into superheroes who are capable of incredible feats.
And while this may sound far-fetched or at least far off, the truth is we are a lot closer than many people realize. Cederna’s groundbreaking work with nerve regeneration following nerve injury is paving the way toward modern-day prosthetic limbs that are capable of feeling sensations, providing fine motor control, and powering exoskeletons that may also allow construction workers to lift 200 lbs—without the help of a bulldozer.
Cederna, the Chief of the Section of Plastic Surgery, the Robert Oneal Professor of Plastic Surgery, and Professor of Biomedical Engineering at the University of Michigan Health System in Ann Arbor, sat and talked to PSP about what’s happening in his lab and what the work will mean for soldiers, cancer patients, and others.
PSP: Most cosmetic surgeons specialize in breasts, face, or body work. How did you get involved in nerve regeneration?
PC: I was a bioengineering student as an undergraduate. The exciting thing about bioengineering is that you can take a few facts and solve an infinite number of problems. After undergrad, I went to medical school and finished my surgical training, which was followed by a postdoctoral research fellowship in muscle and nerve regeneration. Some friends from undergraduate school had found a funding opportunity to develop interfaces for prosthetic controls. This got me back to my roots in bioengineering, allowed me to perform research with friends and investigate problems I was faced with clinically in patients with nerve and muscle injuries, cancers, or other functional deficits which lead to limb loss. Along with my close research collaborators, Melanie Urbanchek, PhD, and Nick Langhals, PhD, we have been able to make outstanding progress toward solving some of the most difficult bioengineering challenges.
PSP: When did you first realize you were on to something big?
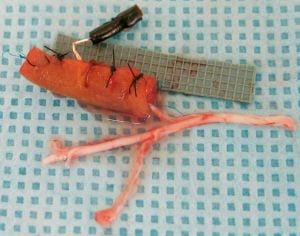
Sciatic nerve with regenerative peripheral nerve interface (RPNI) connected.

20 months after RPNI implantation.
PC: The first breakthrough occurred after our team received a $5.5 million grant from the Department of Defense Multi-Disciplinary University Research Initiative toward the creation of a totally biointegrated peripheral nerve interface that would allow closed-loop neural control of an upper-extremity prosthesis. There were a number of elements that kicked off the research and got us started on this path, and the work has really evolved since then. We have since received additional funding through DARPA (Defense Advanced Research Projects Agency) for the interface. There have been many people involved in these studies, including Greg Gerling, PhD, from the University of Virginia, David Martin, PhD, from the University of Delaware, Phillip Johnson, PhD, and Susan Mackinnon, MD, from Washington University, Daniel Aloi from Oakland University, and my close collaborators from the University of Michigan, Daryl Kipke, PhD, and Brent Gillespie, PhD. The close collaborations with many scientists from many different areas of engineering and information science have allowed us to innovate and discover in areas previously never examined.
PSP: How is your interface different from past attempts?
PC: This is a paradigm shift from what people have done in the past. Engineers had previously designed real high-tech interfaces to wrap around a nerve like a cuff or place into a nerve like a probe, but the nerve does not like things wrapped around or stuffed inside of it. As a result, there was no long-term stability for these constructs. We took a muscle and implanted it on the end of the nerve. We also cushioned the end of the nerve so there is no risk of a neuroma on the bare nerve ending. Neuromas can lead to pain and problems with control. The muscle also serves as a shock absorber between the nerve and electrical component of the interface, so there is no damage to the nerve. The interface amplifies the electrical signals by 100 to 1,000 fold, so we can pick up and carry even the tiniest impulse down wires to an implanted computer in the extremity. The computer then interprets the electrical signal, converts it to a wireless signal, and sends it to the prosthetic limb, which moves accordingly. This happens immediately and seamlessly. There is no delay. None of the predecessors ever successfully developed an interface to provide long-term stability or prevented neuromas. People need the prosthetic for 60 years; they don’t need it for 6 months. The regenerative component has allowed us to have long-term stability. The only data so far is in rats and spans 20 months.
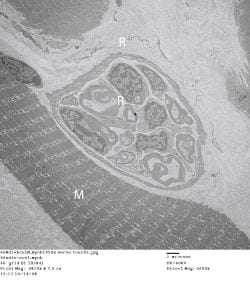
RPNI as seen on electron microscopy.
PSP: How far away is this construct from the bedside?
PC: As soon as they design prosthetics that have good sensory devices in the fingers which can pick up pressure, and deliver feedback to the implanted processor, we can stimulate the sensory nerve. This means a person will have a moving and sensing prosthetic hand. We are within a few years of seeing this happen.
PSP: What is the ultimate goal?
PC: Our goal is not to develop a hand that can open and close. We can do that already. Our goal is independent finger motion. Our goal is sensation.
Cederna in the OR.

Cederna’s neuromuscular lab team.
PSP: Who will benefit and how?
PC: As the robotic developments advance and we get independent finger motion with prosthetic devices, it will take us to the point where we will have finger and wrist motion with sensation that will allow people to play a musical instrument or perform surgery. It is very exciting.
Picture a 20-year-old man who has lost both of his arms during active duty and has a child at home. We can give him prosthetic arms, but he will never be able to feel his child’s touch with his hands. The child may be holding his hand in a busy shopping plaza, and he just wants to gently squeeze their hand so the child stays close and doesn’t run away. We are talking about that type of sensation and delicate control.
PSP: A lot of the current and future recipients of regenerative medicine efforts are members of the military. Why is that?
PC: Unlike veterans of previous wars, today’s war fighters are surviving because of improvements in body armor, but they are losing their extremities. For these reasons, the Department of Defense is funding this research. That’s not to say that civilians can’t benefit from this technology. There isn’t a summer that goes by where people don’t lose their arms or legs in vehicular accidents. People are losing limbs due to cancer – including children with sarcomas. Many older people who lose limbs due to complications from diabetes may never walk again because it takes so much power to control a leg that has no knee or ankle. All of these people may be able to walk again, which would be amazing.
PSP: How well will improved prosthetic limbs change these people’s lives?
PC: When people are missing an extremity, they can have significant body image issues. This impacts their psychological well-being, emotional health, and social lives. Today’s prosthetics don’t help them overcome any of these issues because they don’t look like a limb and they don’t feel like a limb.
PSP: So how can this research give rise to real-life superheroes?
PC: In a word, exoskeletons. For example, a construction worker may not need a bulldozer to lift really heavy objects. The exoskeleton fits over the body and interfaces with the bicep. When the bicep contracts, it signals the exoskeleton to contract and it can curl a 200-lb weight. This technology may benefit construction workers and law enforcement agents.
PSP: Like the six-million-dollar man?
PC: Yes, but we have spent more than that already. The six-billion-dollar man is more like it.
Denise Mann is the editor of Plastic Surgery Practice. She can be reached at [email protected].