By Constance M. Chen, MD, FACS
Once upon a time, when a woman underwent mastectomy, her options for breast reconstruction were limited. Not only was access to a plastic surgeon who could perform breast reconstruction limited, but the expected outcomes for the woman and the plastic surgeon were not always aligned. The goal of the plastic surgeon was to place an implant to create a breast mound.
Techniques were developed to avoid infection, prevent extrusion through radiated skin, and improve symmetry with the other breast in clothes. The woman was supposed to be happy that she did not have to stuff a sock into her bra to avoid questions from her friends. For the woman, however, a hard, numb breast mound could be depressing every time she took a shower or got dressed in the morning. Sexual intimacy and relationships took a direct hit. While the plastic surgeon may have been satisfied that her breast reconstruction was intact, not infected, and did not lead to stares from strangers, the woman still did not feel like she had breasts.
Breast reconstruction has come a long way since the early days of plastic surgery. Breast surgeons can do nipple-sparing mastectomies, which preserve the entire skin envelope of the breast—thus preserving the actual breast shape. Natural tissue breast reconstruction can recreate a soft, warm, living breast that looks and feels like a normal breast—at least to another person.
For a woman, however, the ultimate breast reconstruction will be a soft, warm, living breast that looks and feels like a normal breast to her. When she holds her baby, she can feel it. When she hugs her friends, she can feel it. When she makes love with her partner, she can feel it. For plastic surgeons, the challenge today is to restore shape and sensation to a woman’s breasts.
How Sensory Restoration Works
Peripheral nerve repair has been described as far back as Galen of Pergamon (131-201 AD) and was first documented by Paulus Aegineta, a military surgeon in the 7th century. In modern times, peripheral neurorrhaphy has been extensively studied and practiced in fields such as hand surgery and oromaxillofacial surgery. Today, however, sensory restoration is a reality in reconstructive breast surgery. Neurotizing flaps by primary coaptation, autograft, allograft, or nerve conduit in autologous breast reconstruction has made it possible to restore breast sensation. While neurotization during breast reconstruction is simple and quick, there are ways to make it even simpler and quicker.
Resensation is a technique to restore sensation to autologous flaps during natural tissue breast reconstruction. In order to restore sensation to the new breast, a donor nerve from the donor flap must be identified and dissected, and a corresponding recipient nerve on the chest wall needs to be identified and dissected. One of the limiting factors in sensory restoration is the length and quality of the nerve. A short donor or recipient nerve will not reach the corresponding recipient or donor nerve.
Furthermore, dissecting a long length of nerve that is adequate for direct coaptation is not only time-consuming, but it also denervates the part of the body that the nerve comes from, which can be counterproductive. Likewise, dissecting and harvesting a nerve autograft from another area of the body is even more time-consuming and denervates an entirely separate area of the body, in addition to potentially creating more wounds to heal and visible scars to see.
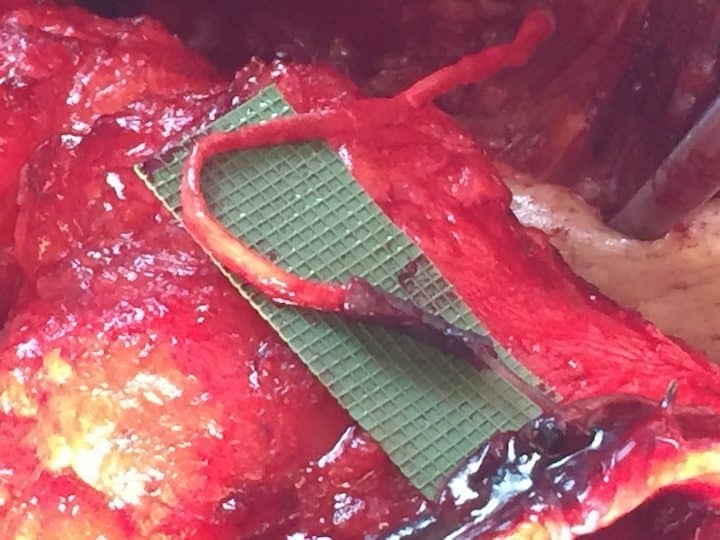
To overcome limitations of peripheral nerve repair in breast reconstruction, Resensation uses a biologically active processed human nerve allograft to surgically connect the donor nerve to the recipient nerve. The patient’s nerves can be very short to minimize dissection time and denervation. Instead of suturing individual fascicles in an end-to-end fashion, which is also time-consuming and vulnerable to error, a nerve conduit is used between the patient’s nerves and each side of the nerve allograft to efficiently allow the axonal regrowth to occur in the proper orientation. Resensation uses a nerve allograft and nerve conduits to restore breast sensation as simply and quickly as possible, while minimizing morbidity and maximizing outcome. (Figure 1).
Resensation Leads to Happier Patients
Ten years ago, a breast cancer patient referred to me for breast reconstruction insisted that she wanted a lumpectomy instead of a mastectomy despite her breast surgeon’s recommendation. She showed me a New York Times article she had just read that said her breasts would be numb after mastectomy. I explained to her that she was BRCA-positive with invasive disease, and that we could do natural tissue breast reconstruction with sensory restoration.
The patient was skeptical, but after consulting with multiple breast surgeons she realized that she was going to need bilateral mastectomies to improve her survival. The patient underwent a bilateral nipple-sparing mastectomy with immediate DIEP flap breast reconstruction and bilateral neurorraphies.
Long after her breast reconstruction was completed, I reminded her of her preoperative fears. She laughed. She was wearing a sundress, and she said she looked and felt better than she had prior to her mastectomies. Soon thereafter, she got married. Sensory restoration after mastectomy brings breast reconstruction patients hope for a fuller and more normal life. Restoring soft, warm, natural breasts with sensation brings the interests of patients and plastic surgeons into alignment. Once upon a time, breast reconstruction was limited. Resensation allows both the patient and the surgeon to live happily ever after.
Constance Chen, MD, FACS, is a leader in microsurgical breast reconstruction. She specializes in DIEP, SIEA, PAP, TDAP, ALNT techniques and runs a private practice in New York City. Visit constancechenmd.com for more information.