
A “Pitcher of Health”
Without a doubt, skin hyperpigmentation remains the most common epidermal problem within the cosmetic physician’s office. Whatever it may be from, skin discoloration can also be the most difficult to treat and, in most cases, it requires a great deal of patience—not only for the patient but for the physician or staff, as well.
The task of discerning a patient’s hyperpigmentation source for healing and prevention can be daunting. Skin discoloration often goes hand in hand with an array of diseases and disorders, which range from the benign to the life-threatening. In my experience, however, unless you remove the source you will not be successful in treating hyperpigmentation for the long term.
MODERN THINKING
There is no escape from the modernization that has happened in our world. Try explaining the flipping mechanism, which stopped reel-to-reel film from jumping in a projector, to students today who happily click twice on their iPads to open a video, log on to hear a podcast, or attend their professor’s newest webinar—all while checking e-mails and firing off texts to friends and colleagues. Just as we have experienced technological advances in every aspect of our lives, so too have we experienced a myriad of new advances in skin rejuvenation.
Hyperpigmentation treatments have also experienced a paradigm shift in method. With hyperpigmentation, however, technology has somewhat taken a back seat. This movement has occurred in the wake of the changes that have happened in facial rejuvenation.
In the past, epidermal rejuvenation included the standard use of high-power, high-density, ablative CO2 laser treatments. Today, we have entered a phase of “less is more.” Along those lines, treatment for hyperpigmentation has, on the whole, become more minimally invasive, with an overriding “do-no-harm” methodology—but has also become increasingly multidisciplinary. In my practice, the collaboration among specialties, new systems, and protocols has shown to be useful.
With this in mind, I have taken a sort of “back to basics” mentality—one that focuses on intracellular water, cell membrane fortification, and cellular health.1 The melanocyte is, after all, a cell. Bleaching compounds, in general, are fairly ineffective on dermal accumulation of melanin.2
ANATOMY OF THE MELANOCYTE
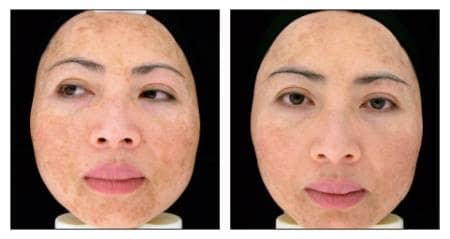
Eleven-month baseline (left) and endpoint (right) photos of a female patient undergoing the Inclusive Health approach.
Melanogenesis is a process that begins in the brain, and melanocytes are dendritic cells that make up about 3% of the cells in the epidermis. The relationship between melanocytes and keratinocytes is referred to as the epidermal-melanin unit. The melanin produced in the melanocyte is transported by melanosomes through the dendrites, which transfer the melanosomes to the keratinocytes. Melanocytes produce two types of melanin: eumelanin and pheomelanin. Eumelanin is brown to black, while pheomelanin is yellow to red.
In tanned skin, eumelanin is the pigment that has been stimulated. Interestingly, I have found that women have more pheomelanin than men, so women’s skin is generally redder than men’s. Those with red hair have high levels of pheomelanin, which imparts a pink to red hue. Pheomelanin is particularly concentrated in the lips and nipples.
The pituitary gland, in the case of melanogenesis, is responsible for creating and releasing intermedins (peptide hormones) or melanocyte-stimulating hormones (MSH). When skin is exposed to sun or experiences trauma, inflammation occurs, which sends inflammatory mediators to initiate the brain’s pituitary response with MSH. Once in the bloodstream, MSH stimulates the adrenal gland, which triggers tyrosine. Tyrosine breaks down tyrosinase, and tyrosinase is broken down further to dopamine.
Through a process of many more interactions and broken-down elements, the melanocytes pump out melanin to protect skin cells from damage. This overly simplified explanation of melanogenesis involves many factors, and several hormones and interactions, that are not completely understood.
In general, however, melanogenesis occurs because of a combination of factors including DNA damage, and these factors may vary from patient to patient.3
TWO PROCESSES AND THREE STEPS
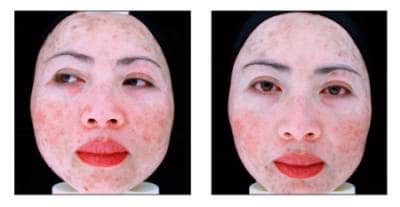
Baseline (left) through endpoint (right) redness reduction on the same patient.
In my experience, the causes of hyperpigmentation can be traced to the presentation and activity of the melanocytes. In general, the following two basic processes cause hyperpigmentation:
- An increase in melanin production; and/or,
- An increase in the number of melanocytes.
Postinflammatory hyperpigmentation (PIH), café au lait macules, melasma, Addison’s disease, sun exposure, and hemochromatosis all stimulate the increased production of melanin. Seborrheic keratosis, acanthosis nigricans (due to diabetes and obesity), lentigines, phototoxicity or photo-allergic reactions (ingestion or exposure), on the other hand, increase the proliferation of melanocytes.4
Depigmenting relies on the following three basic steps:
- Regulating the transcription and activity of tyrosinase, tyrosinase-related protein-1 (TRP-1), tyrosinase-related protein-2 (TRP-2), and/or peroxidase;
- Regulating the uptake and distribution of melanosomes in recipient keratinocytes; and,
- Melanin and melanosome degradation and turnover of “pigmented” Keratinocytes.2
Above all, however, the main goal of hyperpigmentation treatment, especially PIH, is to reduce inflammation regardless of etiology.
INCLUSIVE HEALTH APPROACH
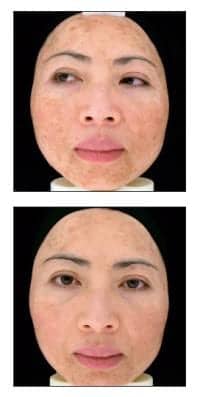
Baseline (top) through endpoint (bottom) pigment evenness
As many of you have probably experienced, hyperpigmentation may have not only a topical component, but also an internal one and even an emotional aspect. The reality is that therapy is obviously a lot more complex than the simple application of hydroquinone. In fact, to be successful in treating hyperpigmentation, a comprehensive method, possibly multidisciplinary, is required to target the source, remove the discoloration, and prevent further pigmentation problems.
I call this comprehensive method an “inclusive health” approach. It includes a formulaic, three-pillar protocol that I apply to every one of my patients. Generally, it breaks down the treatment strategy into topical, internal, and emotional categories, and helps create a road map to the treatment goal.
Through a series of standard checks and evaluations, an inclusive program is initiated targeting each patient’s specific needs. While no protocol is exactly the same, the three-step approach offers a complete strategy toward removing any source and presentation of hyperpigmentation, and has the added benefit of placing a patient on the track toward total wellness.
GETTING STARTED
The initial consultation with any patient begins with a quid pro quo session on what the patient has experienced, what I have experienced, what the patient knows about hyperpigmentation, and what I can teach him or her. Education is the first step in any treatment protocol.
Realistic expectations must be expressed clearly. Otherwise, you will have very unhappy patients. I always explain that it will take at least 30 days for improvements to be seen because of the nature of how skin sloughs. I also explain that treatment must be ongoing to completely resolve hyperpigmentation and prevent it from recurring, and I ensure that they understand that any underlying issue must be followed and treated for optimum results.
During the initial skin examination, I look for the presence of uneven skin tone or freckles, which indicate that there is a lower amount of melanin in the skin, thus a reduced capacity for DNA repair. In other words, the patient is at increased risk for photocarcinogenesis, and great care must be taken to prevent further skin damage with sun protection.
Simple tips on prevention with appropriate application of SPF and sun avoidance, at this meeting, are imperative as subsequent treatment depends on the patient’s commitment to the inclusive program. While second nature to those of us in the clinical setting, most patients do not know what SPF to use or that it is necessary for every Fitzpatrick skin type. Beyond that, most patients are remiss in their application of sun-protection creams, so it is useful to pair retail with instruction at this initial consultation.
Home care for daily exfoliation and skin treatment is also essential. I provide patients with a combination of ingredients such as AHAs and BHAs to reduce excess skin cell buildup, as well as vitamin C products because they are also beneficial for brightening the complexion.
Because we are definitely comprised of the elements that we eat, I also begin my patients on a nutritional program that includes supplements to flush the body with the nutrients needed to fortify cellular health, immunity, and to increase intracellular water.5,6

Same patient: Baseline (left) through endpoint (right) pore size
When cell membranes are fortified and intracellular water is maintained or increased, cells function at the highest levels to correct ROS-induced damage on the outside and inside of the cell.7-10 This protects the nuclear membrane, the mitochondria, and DNA transcription processes. Cell water transfer is flawless, bathing structures with nutrients and removing cytoplastic accumulations of waste materials.11 It also halts inflammatory cascades in tissues.12
It has been well documented in scientific literature that nutrition can play a key role in skin health.13 Poor nutrition can also accelerate skin degeneration. I have seen, firsthand, how a healthful diet complete with optimal nutrition can help forestall, prevent, and even reverse skin conditions and improve overall health.14
Because the standard American diet is subpar, supplements are given to every patient at this initial meeting, as well. The following illustrates the inclusive health program’s three areas:
AREA 1) TOPICAL CARE
Topical care is used to enhance cutaneous immunity, reduce inflammation, and treat epidermal conditions. This includes topical treatments, such as aesthetic facials, appropriate skin care regimens, and cosmetic medical services.
Because the release of melanin begins in the basal layer—the deepest layer of the epidermis—it can be difficult to treat existing hyperpigmentation with aesthetic treatments. Additionally, treatments will take at least a month to work as basal cells move up through the layers of skin to the outermost stratum corneum and become sloughed off with exfoliation.
With regard to any hyperpigmentation, excluding melanoma and no matter the Fitzpatrick skin type, the topical portion of my inclusive health formula always remains the same for every patient.
I use a gentle combination of peels, including salicylic acid, glycolic acid, retinol, and niacinamide. I have found combination therapies to be more successful than single agents used alone. In the plastic surgeon’s office, IPL, vitamin C peels, topical infusions, and lasers may also be used. Aggressive techniques may cause inflammation, more hyperpigmentation, and may be more trouble than they are worth.
My standard protocol begins with a combination of peels performed in-office once every 2 to 4 weeks (depending on how it is tolerated by patients). Paired with any needed internal care and home care, which prepares the skin and enhances the in-office peel combination, most hyperpigmentation issues will begin to fade by 30 to 45 days.
Salicylic acid. Superficial salicylic acid peels have shown to be both safe and effective at treating PIH even on darker skin tones. Salicylic acid is a keratolytic and comedolytic agent that helps stimulate rapid cell turnover and quash macule formation postacne.
Glycolic acid. A workhorse in the dermatologist’s office, glycolic acid can be used on even the darkest skin tones. It effectively loosens cell-binding lipids between keratinocytes to exfoliate the stratum corneum.15
Retinol. The precise mechanism for why retinoids work with hyperpigmentation is unclear. However, they are thought to inhibit the induction of melanogenesis while also stimulating rapid skin cell turnover and promoting new cell growth.
Niacinamide. Also known as niacin, vitamin B3, or nicotinic acid, niacinamide has shown to inhibit melanosome transfer from the melanocytes to the keratinocytes. It is also anti-inflammatory.16
BOTANICAL AND ANTI-INFLAMMATORY INGREDIENTS
The study of botanical ingredients is one area that has garnered significant attention from the cosmetics community. Specifically, many early studies have suggested that there are quite a few natural fruit, vegetable, and herbal ingredients that offer anti-inflammatory and sun-protection-boosting capabilities.17 With regard to hyperpigmentation, cell fortification, immunity, and cellular water, the ones that stand out include those highest in antioxidants, essential fatty acids, and polyphenols.
For decades, the medical field and aesthetics industry has highlighted inflammation as the greatest villain to body health and skin rejuvenation. And this is true if the inflammation is chronic, an overreaction, or cannot be repaired. It is important to note, however, that inflammation does not cause disease. Rather, it is disease that causes inflammation. The best way to forestall disease is to make the body more resilient to it, which means the immune system and nutrition play very important roles.
Healing slows when inflammation is present. Skin texture may be rough and dry with discoloration from PIH. On the inside, there may be underlying problems or inflammatory diseases, such as Crohn’s disease, ulcerative colitis, nephritis, and systemic lupus erythematosus. In addition, diabetes, heart disease, arthritis, and cancer can cause inflammatory responses in the body. The simple truth is that any overreaction or chronic inflammation within the body will likely exhibit effects on the skin, as well, and make hyperpigmentation treatment harder.
AREA 2) INTERNAL CARE
Internal care is used to support all aspects of a healthy lifestyle. This includes nutrition, supplements, and prescription medication. Medical history will tell you if your patient has any internal disorders, that may be the causative factor for his or her hyperpigmentation. If no internal disorders are known, blood tests may be useful.
A nutritional food plan, which includes high amounts of antioxidant, anti-inflammatory foods, is recommended, as well as a daily supplement regimen including the following:
- Multivitamin and mineral supplement. Select a comprehensive and balanced formula containing all the major vitamins, minerals, and trace minerals; select an iron-free formula for patients who are postmenopausal.
- Sleep-promoting supplements, including those featuring up to 1 mg of melatonin and gama aminobutyric acid (GABA).
- Antioxidant supplement formula.
- High-potency B complex supplement providing all eight essential B vitamins: thiamine (B1), riboflavin (B2), niacin (B3), pantothenic acid (B5), pyridoxine (B6), folic acid (B9), cyanocobalamin (B12), and biotin (B7).
- An essential fatty acid supplement providing omega-3 fatty acids. This may be in the form of fish oil, flaxseed oil, or ground flaxseeds added to food or in capsule form. Vegetarians or those not eating fish or taking fish oil supplements should add a micro-algae-derived DHA supplement.
- Lecithin supplement. Recommend soy lecithin granules sprinkled on or added to foods or a liquid soy lecithin in capsule form.
- Glucosamine.
- Calcium supplement for bone health. Most women should take 1,000 mg to 1,500 mg of calcium with vitamin D daily, depending on their dietary intake of calcium.
AREA 3) EMOTIONAL CARE
Emotional care will help patients achieve psychological and social balance. Significant negative psychological issues result from hyperpigmentation. In my patients, it is often noted as a source for social stress. Literature suggests that hyperpigmentation problems have the power to reduce productivity at the office and in school as the skin condition erodes self-esteem.
Hyperpigmentation is a considerable “quality of life” issue for its sufferers. As such, I recommend patients partake in stress-reduction spa services, exercise, or even receive some emotional self care to cope.
As far as diseases and internal conditions are concerned, skin cancer, diabetes, and obesity seem to contribute the most hyperpigmentation problems. This is perhaps symptomatic of the rising statistics of these health epidemics, but they still only account for a smaller percentage of patients. The majority of patients I see exhibit what I term “polka-dot syndrome.” I also see a large amount of melasma and lentigines.
Polka-Dot Syndrome
This includes PIH, acne macules, and freckles. Because of the amount of pigment in dark skin, discoloration problems are very common and their visual effects can be similar to a polka-dot pattern.
PIH is more of a problem in those with Fitzpatrick IV to VI skin types and can be the result of either exogenous or endogenous inflammation, which may be the result of skin conditions or mechanical trauma, radiation, phototoxicity, laser procedures, or even temperature. In general, sunscreen is useful, and anti-inflammatory services and retail products have shown to be effective in my patients.
Regardless of sun exposure, hyperpigmentation can develop at the site of an injury or after a blemish has healed. I have found that endogenous porphyrins, which cause acne macules, can be removed through the use of light-emitting diode treatments. Porphyrins released by P. acnes attract certain wavelengths of light. Targeting the porphyrins alone has offered my patients promising results.
At a microscopic level, light excites these P. acnes porphyrins, which release singlet oxygen when they are excited. This oxygen, in turn, kills P. acnes. Porphyrins absorb the most light at 415 nm (blue light) and 630 nm (red light). Thus, both red and blue light are effective at circumventing PIH and macules. Red light has been purported to stimulate healing and reduce inflammation. So, red and blue light work well together on inflamed acne and to prevent hyperpigmentation.
Melasma
Melasma is characterized by darkened pigmentation, usually down the center of the face. Typically, it involves the nose, cheeks, upper lip, and sometimes the forehead. I almost never see melasma in men. It seems to be caused by the combination of pregnancy or birth control pills and exposure to sunlight. It is especially difficult to cure melasma on black skin.
Perfumes and even some cosmetics can cause allergic reactions with symptoms similar to melasma. If a patient who appears to have melasma is taking birth control pills, I suggest that she try taking her usual dose at night rather than in the morning in order to minimize the amount of estrogen in the bloodstream during sunlight hours. A pill with a lower dose of estrogen may be useful, as well.
Hydroquinone 2% to 4% or azelaic acid 20% will suppress and gradually lighten epidermal hyperpigmentation from melasma. Vitamin A (tretinoin/retinol) and/or glycolic, lactic, or salicylic acids allow for improved penetration of hydroquinone. Laser treatments specific for pigment disorders are often helpful alone or in combination with topical therapy. High levels of vitamin C with glycolic peels and IPL (intense pulsed light) can also provide results. Sun exposure should be avoided, and daily application of a broad-spectrum sunscreen is recommended.
Lentigines
Lentigines (or solar lentigos), commonly referred to as liver spots, are found on sun-exposed skin among middle-aged and elderly adults. They are flat, evenly pigmented (tan or brown) spots with well-defined borders and range between 2 mm to 30 mm in size. Chronic sun exposure and genetic predisposition are causative factors for solar lentigos, which lead to local proliferation of melanocytes.
While there is no potential for malignancy with solar lentigos, the appearance of lentigines indicates a degree of ultraviolet skin damage. Patients should avoid sun exposure and use a high-SPF, broad-spectrum sunscreen daily. Epidermal peeling, lasers, and cryotherapy help remove abnormal melanocytes and reduce the appearance of dark spots. Hydroquinone and tretinoin may gradually decrease the darkness associated with lentigines over months.
CASE PRESENTATION
As illustrated in this article’s accompanying photos and graphs, a 43-year-old female Asian patient with lupus and severe melasma is shown at her baseline, initial consultation, and then about 11 months later.
The patient consultation revealed that as a dentist, she experiences regular psychological stress. She admitted that her nutrition lacked a good amount of fruits and vegetables, and that she has a hard time “unplugging” from technology. This patient followed a complete inclusive health plan that included only the standard topical peel combination (salicylic acid, glycolic acid, retinol, and niacinamide) for treatment of her melasma.
With just the standard peel combination, at the end of the 11 months, her pigmentation presentation was reduced and looked more even, localized, and overall redness was reduced. Hyperpigmentation was reduced to small localized patches, her pore size was reduced, and she felt more confident about her skin.
The patient noted that the most dramatic results came because of the whole-body approach, exercise, and nutrition. She noted that she had more energy consistently throughout the day and felt more positive. She also disclosed that she now makes time for self care, and this has made a big difference in her mental state.
All subjects enrolled in an inclusive health program undergo a baseline and end point Bioelectrical Impedance Analysis and Body Composition Analysis. I used Quantum II (RJL Systems, Clinton Township, Mich) and Cyprus 2.7 (RJL Systems) software to calculate intracellular water values. I determined that this patient went from 28% intracellular water to 30% intracellular at 10 weeks.
TOTAL WELLNESS, LASTING BEAUTY
I have merged thinking on cellular health and immunity with treatments that work topically, internally, and emotionally to produce the best results possible for my patients. Through the use of home care, gentle in-office peel combinations, nutrition, prescription medications, modern technology, and tried-and-true complementary therapies, it is possible for patients to be cured of hyperpigmentation and experience a better overall quality of life.
Scientific study has brought us to where we are today. Consumers have pushed the industry to honor their requests for better and longer-lasting results. Currently, the inclusive health care environment aims at being noninvasive but is ever more thorough at removing the underlying problem. Collectively, the result is optimum health and beauty that lasts.
Howard Murad, MD, is a board-certified dermatologist, pharmacist, author, and associate clinical professor of medicine (dermatology) at UCLA. His practice is based in El Segundo, Calif. Murad has a financial interest in vitamin C, glycolic acid, and nutraceutical products distributed and marketed under the brand name Murad. He can be reached at (310) 335-1700.
References
- Murad H. Thoughts on the process of aging. Cosmet Dermatol. 2009;22(2):74-78.
- Briganti S, Camera E, Picardo M. Chemical and instrumental approaches to treat hyperpigmentation. Pigment Cell Research. 2003;16(2):101-110.
- Murad H. Look again, what did you miss…? Dermascope. 2008;33:87-92.
- Stulberg D, Clark N, Tovey D. Common hyperpigmentation disorders in adults: Part I. Diagnostic approach, Café au Lait macules, diffuse hyperpigmentation, sun exposure, and phototoxic reactions. Am Fam Physician. 2003;68(10):1955-1961.
- H Murad, J Jankicevic. Dietary supplementation as a nutrition intervention strategy to increase intracellular water and phase angle. Paper presented at: American College of Nutrition 48th Annual Meeting and Conference; 2007; Orlando, Fla.
- Murad H, Tabibian M. The effect of an oral supplement containing glucosamine, aminoacids, mineral, and antioxidants on cutaneous aging. J Dermatol Treat. 2001;12:47-51.
- Nagy IZs. The Membrane Hypothesis of Aging. Boca Raton, Fla: CRC Press; 1994:3-10.
- Nagy IZs. The frustrating decades of biological aging theories and the hopes for the future. Anti-Aging Bulletin. 2003;4(16):22-31.
- Nagy IZs. The membrane hypothesis of aging: its relevance to recent progress in genetic research. J Mol Med. 1997;75:703-714.
- Nagy IZs. Enzyme activities in the light of the membrane hypothesis of aging. Mech Aging Dev. 2001;122:811- 821.
- Ritz P. Chronic cellular dehydration. J Gerontol. 2001;56A(6):349-352.
- Murad H. Skin immunity, the next generation of skin. Les Nouvelles Esthetiques & Spa. 2008;7:130-136.
- Murad H. Antioxidants: nutritive effects on the skin. Paper presented at: Noah Worcester Meeting; January 2004; Maui, Hi.
- Gupta D, Lammersfeld CA, Burrows JL, et al. Bioelectrical impedance phase angle in clinical practice: implications for prognosis of advanced colorectal cancer. Am J Clin Nutr. 2004;80:1634-1638.
- Murad H, Shamban AT, Premo PS. The use of glycolic acid as a peeling agent. Cosmet Dermatol. 1995;13(2):285-307.
- Ortonne JP, Bissett D. Latest Insights into skin hyperpigmentation. J Investig Dermatol Symp Proc. 2008;13(1):10-14
- Murad H, Shellow W. Pomegranate extract both orally ingested and topically applied to augment the SPF of sunscreens. Cosmet Derm. 2001;14(10):43-45.



