by Schae Kane
Steven R. Cohen, MD, FACS, on the use of stem cells in fat grafting procedures
No one can accuse Steven R. Cohen, MD, FACS, of being a slouch. He is known worldwide for his contributions to the treatment of children with facial deformities, such as cleft lip and serious craniofacial skeletal malformations. Cohen is the inventor of one of the leading internal distraction systems, the MID system, and holds a patent on the Macropore biodegradable distraction device, which is the first of its kind in the world.
In addition to helping to develop surgical techniques, Cohen has been involved in fat grafting for most of the 21 years he has been in practice. As an early clinical researcher in an IRB-approved study, he was involved in adipocyte-derived stem and regenerative cells in 2003, when he and Ralph Holmes, MD, performed the first series of injections for facial rejuvenation.
Cohen currently serves as executive director of the Cell Society, a nonprofit international organization dedicated to the advancement of the clinical applications of adult stem cell regenerative therapies. If that weren’t enough, Cohen is also an acclaimed painter and sculptor.
Unlike many physicians who have worked with stem cells in very limited applications, Cohen endeavors to incorporate new technologies in as many procedures as he can muster from his private practice—from facelift surgery to rhinoplasty to breast augmentation and tummy tucks.
PSP sat down with Cohen to gain insight into his use of fat grafting using stem cell technology.
PSP: What was it that attracted you to investigating and eventually working with stem cells in the cosmetic surgery field?
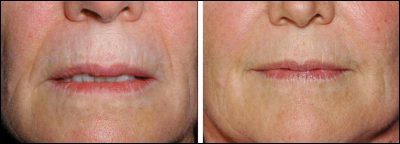
Before and 6 years After CEFT to Nasolabial Folds and Radial Lip Lines
Cohen: I first became familiar with the use of fat-derived stem and regenerative cells in the early 2000s. There appeared to be significant promise that these cells would work well to reconstruct missing tissues and address aesthetic goals. We know that the body has the natural ability to repair itself in limited circumstances, such as wound healing, and as physicians and scientists it is exciting for us to find a way to harness those mechanisms, concentrate them, and use them in many ways to regenerate tissue and repair injury from a variety of diseases. There really is a lot of potential for the use of stem cells in medicine overall.
The use of the body’s own cells is theoretically appealing, and since experimentally and from preliminary clinical experience, the live cells seem to enhance the overall survival rate of fat grafts. This should increase the success of these procedures. I expect more widespread adoption to be forthcoming.
PSP: How easy or difficult is it to “sell” patients on a procedure that uses their own stem cells?
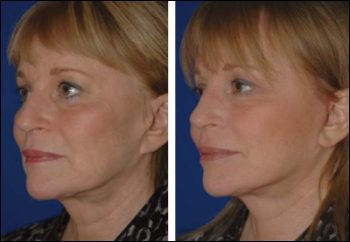
63 Year Old Female Before (left) and 3 Months After Mini-facelift and CEFT to Cheeks, Perioral Region, Marionette Basins, Temporal Regions and Nasojugal folds (30 ml)
Cohen: I am not in the business of “selling” one procedure or another to my patients. As a physician, I inform the patient on the variety of available options, answer their questions, and help them come to the best decision given their personal objectives.
For example, if a patient comes to me for a facelift, usually it entails more than just repositioning of the skin and muscle and removal of tissue. To get the best result, one must address all aspects of aging—loss of elasticity, soft tissue and bony volume loss, and photoaging. To address loss of soft-tissue volume, there is usually a need to increase tissue volume in various areas of the face. So, when I present the option to increase tissue volume to a patient, I also present the available treatment techniques—fillers, conventional fat grafting, or using the patient’s fat combined with the regenerative and stem cells already in their adipose tissue.
As another example, when a patient comes to me for a liposuction procedure, they are asked if they would like to discard the fat, donate the fat for scientific study, or use the fat elsewhere. It is explained that their own fat cells can be used to augment tissue in a variety of procedures, from facelifts to buttock augmentation, body shaping, or recontouring. In younger patients, they may consider a lip augmentation, cheek enhancement, or breast enhancement using their own fat tissue.
If they express interest in fat-derived stem and regenerative cells, they are provided with a document that details the FDA’s regulations regarding the off-label use of cell-enriched autologous fat transfers.
Once the patient has the opportunity to review this document, the patient asks questions—typically, they ask why there is a difference between traditional fat grafting and fat grafts using stem and regenerative cells. Many patients already know about the use of stem cells and like the idea of using their own cells and their body’s regenerative mechanisms to help with healing.
Patients seem to be pretty educated, and are very excited about the potential. However, it is still a new area and data are being gathered. Also, it is somewhat unfortunate that the “sex appeal” is the stem cells, when really the stem cells are a small proportion of the regenerative cells that are being re-introduced. I let the patients know that enhancement of fat graft survival has been shown in pre-clinical studies, but the clinical experience is still small. And although we are seeing some amazing outcomes in radiation injuries, breast reconstruction, and breast augmentation, the clinical results are still preliminary. As a scientist and a physician, I am watching these study results closely but I am excited about the potential, as well.
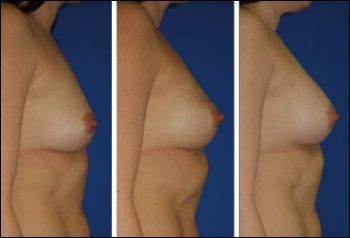
Left to right: From preop to 6 weeks after augmentation using 150 mL with CEFT.
PSP: In what procedures have you used the stem cell approach?
Cohen: Stem cells are applicable and appropriate in a wide range of procedures: breast augmentation, lumpectomies with radiation where some reconstruction is desired, especially in the treatment of radiation injuries where cells have died. Buttock augmentation, facial rejuvenation procedures and reconstruction, and basically any surgery where soft tissue needs to be replaced.
It is a great option for patients who may have adverse reactions to implants, such as capsular contraction. The approach can also help smooth and shape the breast in conjunction with the use of implants. When fat or fat with stem and regenerative cells is used correctly, it can give a better, more natural shape than an implant alone.
Conceivably, there are so many indications where stem and regenerative cells could be a viable option that I expect there may come a day where there is equipment for harvesting and using stem cells in every operating room in every major hospital.
PSP: Is this approach truly appropriate for all these procedures?
Cohen: Stem cells are definitely appropriate for all of these treatments you mention. In the aesthetic world, stem and regenerative cells make sense in reconstructive procedures.
Fat is considered to be a desirable reconstructive and aesthetic filler by physicians worldwide, but in some cases the fat cells aren’t able to thrive in a new environment. There are studies under way comparing the use of stem cell-augmented fat versus conventional fat grafting, and that data gathering is ongoing. Preliminary results imply that cell-enhanced fat increases the longevity of the life of the fat cells, and when used as a cell-enhanced filler their effectiveness seems to be more predictable.
It seems intuitive to me that there would be tremendous benefits from the use of stem and regenerative cells. In my experience, the fat grafts last to a greater extent and the skin appears to reap benefits, as well. However, I do not have enough data yet to fully document this impression. The skin just seems to look better.
The use of stem cells may also be indicated in procedures designed to address reduced vascularity—stem and regenerative cells can be used to improve tissue viability. For example, with pressure ulcers, diabetic wounds, or even ischemic coronary disease, stem cells may be an appropriate treatment mechanism.
PSP: Where do you see this technology and approach heading?
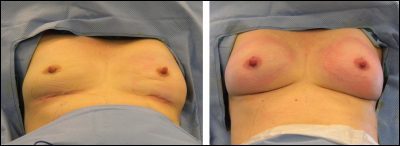
This patient’s breat implants were removed (not complete collapse), followed by 220mL of CEFT (right).
Cohen: There are really two fronts of development. First is fat grafting in general. How is it extracted? What is the best processing procedure? How do we know if the cells are viable? More research is under way to address these questions.
Second, how do we consistently deliver viable stem and regenerative cells, and what techniques and technology work the best? The scientific community is working on ways to standardize the process so that it is safe and effective, no matter what the application. And there are delivery systems in development that look promising for the future.
Comprehensive patient screening is also an important consideration. For example, when we consider that one in seven women will get breast cancer at some point in their life, it becomes apparent that every patient undergoing a breast-related procedure should be screened to ensure there are no pre-existing issues to address. In my practice, I screen patients using mammograms and preferably MRI.
The majority of studies in animals and humans have shown no significant statistical correlation between autogenous fat grafts with and without stem and regenerative cells and an increased risk of cancer. In fact, there is some evidence that fat might bind to estrogen receptors and reduce tumor growth in estrogen-positive breast cancer. Preliminary studies in humans with fat and with cell-enhanced fat grafting have not demonstrated an increase in breast cancer. It is critical that this information be collected, since researchers estimate that a population of 100,000 to 200,000 women will be needed to determine if the frequency of breast cancer is decreased, increased, or unchanged. Somehow, I personally think it is hard to imagine how the frequency of breast cancer will be changed using the body’s own tissues, but it is necessary to have a frank discussion with patients so they thoroughly understand that we do not have definitive information at this point. I am extremely candid with these points.
The main reason regenerative cell therapy is trending so strongly in cosmetic surgery, in particular, is that the process is all completed at the point of care. Nothing needs to be sent off to a lab or processed outside of the treatment facility at the time of the procedure itself. It is easy for the patient, and the materials are part of the patient’s own body. There is less chemistry and more transfer of natural body materials to achieve a particular result. This is appealing to a wide variety of patients.
PSP: What do you think has to happen before the approach is adopted more widely?
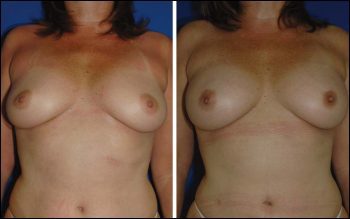
Left to right: Before and 4 weeks after 370-mL breat augmentation with patient’s own and ADRCs.
Cohen: The FDA is currently evaluating the use of fat-derived stem cells, and once their guidelines are completed then physicians will have clear direction on their appropriate use using stem cell technology.
For now, adipocyte-derived stem and regenerative cells are being utilized in an off-label environment by a number of surgeons, but that limits their availability on a more comprehensive basis. Unfortunately, there isn’t a real way to know when those guidelines will be finalized. The FDA looks at regenerative medicine as a promising new frontier, and they are managing its investigation appropriately. They are responsible for making sure patients aren’t duped into getting expensive “cure-all” treatments that don’t produce any real results.
As physicians, we need to continuously learn more about the conditions required to treat patients effectively using stem and regenerative cell technology. I foresee a time when this equipment will be a mainstream instrument in all hospitals. Its potential for use in such a wide range of treatments makes it something we can’t ignore. Everything from breast augmentation, facial reconstruction, body contouring to wound healing and even possibly in the treatment of myocardial infarction, chronic myocardial ischemia to conditions such as urinary incontinence and shock. The limits have yet to be defined.
Schae Kane is a contributing writer for PSP. She can be reached at [email protected].





