Plastic surgeons discuss current thinking about the common complication | Plastic Surgery Practice June 2014
By Louise Gagnon
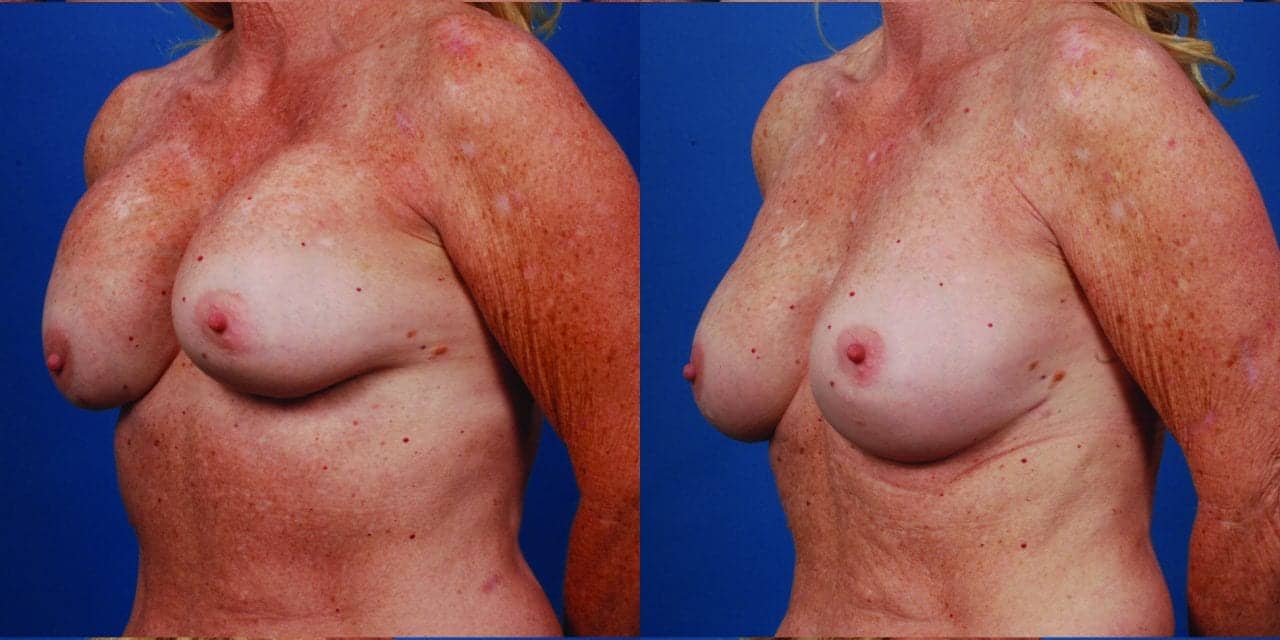
Capsular contracture is one of the most common yet vexing complications to follow augmentation mammoplasty, largely because there is no consensus on exactly what causes it or how to best prevent or treat it.
Regardless of the cause, an aggressive surgical approach is warranted to address capsular contracture, says Louis Strock, MD, a plastic surgeon in private practice in Fort Worth, Texas, and staff surgeon at Texas Harris Methodist Hospital Fort Worth and Fort Worth Surgery Center.
Strock and others discussed current thinking about capsular contracture at the Toronto Breast Surgery Meeting and Aesthetic Plastic Surgery Meeting held this past spring.
One revisionary surgical approach is to create a neopectoral pocket. A study published in a 2009 issue of the Aesthetic Surgery Journal found just three of 198 patients required subsequent reoperations after this approach. “The idea is to make a new pocket for a new implant,” Strock tells Plastic Surgery Practice. “It entails a site change. If a surgeon previously placed the implant subglandurally, then the surgeon should go subpectorally.”
Removing the capsule depends on the degree of inflammation and calcification that is present, among other factors, Strock says. Some surgeons advocate using acellular dermal matrix skin products to curb further inflammation, but these can be costly, he says.
William P. Adams, Jr, MD, a plastic surgeon in private practice in Dallas and an associate clinical professor of plastic surgery at the University of Texas Southwestern Medical Center, treats capsular contracture with total capsulectomy with site change when appropriate and an implant exchange.
“You want to try to avoid multiple surgeries, and taking these steps goes a long way to minimizing reoperation for capsular contracture,” Adams says. “In our published studies, the reoperation rates are less than 3%.”
Incision choice and its role in the development of capsular contracture has been hotly debated. Most surgeons opt to make an inframammary incision, but a transaxillary incision is also a viable option.
“I would suggest that it is more technique-related than incision-related in the case of the inframammary fold versus the transaxillary approach,” Strock says.
In using the transaxillary approach, eliminating dead space is important, he explains. “Our postoperative care is about obliterating the dead space as much as possible and preventing malpositions or fluid collection.”
Implant choice, whether textured or smooth, does not significantly alter the risk of capsular contracture, Adams says. “There is some current data showing a lower capsular contracture rate with form-stable cohesive gel implants, but many argue that it’s not the implant but the other good techniques that are actually producing the benefit,” he says.
PREVENTING INFECTION
To date, much research points to subclinical infection with biofilm as an instigating factor in capsular contracture.
“There is a big groundswell around bacteria and biofilm implicated in capsular contracture,” Adams says. “People are aware of it and taking measures such as using triple antibiotic breast pocket irrigation, dissecting the pocket without that much blood loss, and using nipple shields.” Devices such as the Keller Funnel, which employs a no-touch technique, may reduce the risk of bacteria contaminating the surface of the implant shell.
Surgeons are also taking precautions like prescribing antibiotics to patients who are undergoing dental procedures to minimize the potential for capsular contracture, Adams says.
“Dental procedures are recognized as causing bacteremia,” Adams explains. “New bacteria can be introduced around the breast implant that could cause a problem. Sometimes you will see a patient who has a new capsular contracture, and there is a reasonable time relationship when they started noticing the problem and having had a dental procedure.”
Louise Gagnon is a Canadian journalist, writer, and editor. She can be reached at [email protected].
Original citation for this article: Gagnon, L. Closing in on capsular contracture: Plastic surgeons discuss current thinking about the common complication. Plastic Surgery Practice. 2014; June, 28.