|
Though occasionally unpredictable in terms of its outcome, fat transplantation (or fat grafting) is no longer considered investigational.
It is an accepted and increasingly more frequently undertaken surgical procedure, one that is fast becoming a staple in the average aesthetic surgeon’s surgical armamentarium.
As is the case with any new treatment modality, not only is fat transplantation being applied to progressively more diverse clinical problems, but the limits of the surgical procedure are expanding as well, especially in terms of the volume of fat transplanted at any one time.
This article presents the results of bilateral buttock augmentation employing large-volume fat transplantation, which is also known as the “Brazilian Butt Lift.”
In addition, I shall review the surgical principles and precautions that I believe enhance the probability that the procedure will produce favorable results.
The patient in question, a woman 52.9 years old at the time of surgery, was bothered by flat buttocks and sought fuller, more shapely buttocks or, to quote her, “J-Lo” buttocks.
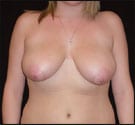
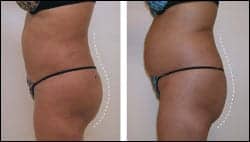
Figure 1 depicts her preoperative and postoperative appearance exactly 102 days (14-plus weeks) later, following transplantation of 400 cc of fat into each of her buttocks, specifically the upper half or so of each buttock—and skewed to some extent to the upper outer quadrant of each buttock.
As of the writing of this article, more than 8 months postoperatively, the patient’s buttocks have not lost any postoperative fullness and, in fact, have increased minimally in size. This is most likely due to a slight weight gain on the part of the patient since surgery.
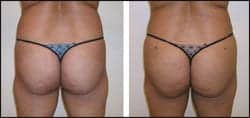
The photo of her postop backside (Figure 1) demonstrates the points of entry of the transplanted fat (note two “dots,” one in the upper outer quadrant of each buttock). As the photos demonstrate, there was a very obvious favorable change in the contour of the patient’s lower back and buttocks.
Needless to say, the patient has been delighted with the results of surgery. Based upon my experience with this and other patients, I have reached a number of conclusions about the factors that contribute to successful fat transplantation.
GOOD CANDIDATES
 |
|
 |
|
 |
|
 |
|
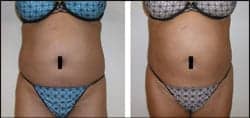
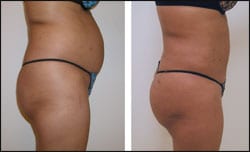
| Figure 1. Female patient (52.9 years old) sought fuller, more shapely buttocks. Top row, left to right: Her back, both preoperative and postoperative. Middle row: Preoperative and postoperative front. Bottom row: Preoperative and postoperative right lateral. Her postoperative photos were taken 102 days after surgery, following transplantation of 400 cc of fat into each of her buttocks. | |
First and foremost, appropriate patient selection is essential to a satisfactory surgical result.
The patient in question is someone who enjoys excellent health, other than extra weight, which, given the nature of the surgery she underwent, proved to be to her advantage. Probably because of her maturity combined with a comfort level with me, she related to her previous use of my services, understood the sometimes unpredictable nature of fat transplantation, and accepted the possibility of an inadequate or even failed surgical result.
In addition, her excellent truncal skin tone/turgor and absence of significant buttock skin laxity/ptosis, consistent with that of a younger woman and which is apparent by her preoperative photographs, is conducive to a satisfactory surgical result, not just with regard to fat transplantation but with regard to the liposuction necessary to harvest the transplanted fat.
Doing a thorough and proper job of preparing the patient for surgery is very important as well.
Given the blood loss associated with large-volume liposuction and fat transportation, I encourage all patients undergoing such surgery to take iron supplements orally, ideally for a month or so prior to surgery. It is most easily available in the form of an over-the-counter iron-containing multivitamin. They should continue taking the iron for a period of several weeks postoperatively.
In addition, I encourage patients to consume more than normal quantities of nourishing liquids (fruit juices, etc) during the first several days to 1 week postsurgery in order to counter the hypovolemia that can follow such surgery.
As I am able to undertake such surgery in an ambulatory surgery facility on an outpatient basis—with the patient almost always under general anesthesia to ensure total patient cooperation—I never had to transfuse patients undergoing such surgery. However, I know that without attention to the foregoing, many patients may experience light-headedness and/or dizziness postoperatively, owing to anemia and/or hypovolemia.
During surgery, I routinely monitor urine output with a Foley urinary catheter which, if necessary, can be left in place for a day or so, particularly if postoperative physical activity must be severely minimized.
The patient in question, whose Foley catheter was removed very shortly after completion of her surgery, was permitted to visit the bathroom as necessary but was cautioned against sitting down for a week after surgery.
SITE PREPARATION
Proper surgical site preparation involves “wetting” the fat destined for liposuction.
I prefer to use warmed (but certainly not hot) Lactated Ringer’s solution. Of all the wetting solutions that can be employed in conjunction with liposuction, I believe that Lactated Ringer’s solution is the most physiologic and, therefore, least noxious to fat.
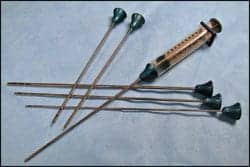 |
| Figure 2. The syringe-based liposuction system that employs cannulae with diameters of 3 to 4 millimeters. |
I do not adhere to a specific ratio between fluid in and fat out. Instead, I prefer to instill enough Lactated Ringer’s solution to slightly distend but not overly tense the area(s) being subjected to liposuction.
Generally speaking, though, the ratio between fluid in and fat out usually proves to be in the neighborhood of 1-to-1.
Gentle fat removal, I believe, is facilitated by a syringe-based liposuction system, employing cannulae with diameters of 3 to 4 millimeters, such as that depicted in Figure 2 (page 28).
Such a system forces me to undertake liposuction in a methodical, paced way, that ensures removal of minimally traumatized fat.
The use of cannulae in the 3- to 4-millimeter-diameter range allows the removal of more intact fat or less “blenderized” fat; which, in turn, is more prone to survival after transplantation.
In the case of the patient in question, I removed a total of 1090 cc of lipoaspirate from various areas of her trunk, primarily from her abdomen.
In my experience, the abdomen yields the most reliable source of transplantable fat and, when compared to other areas of the anatomy, fat that is more prone to survival after being transplanted.
In a similar manner, abdominal skin/fat, in my hands, is the best source of derma-fat grafts employed for soft-tissue augmentation (lips, nasolabial folds, etc).
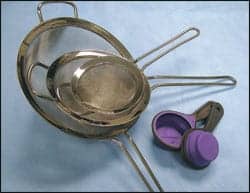 |
| Figure 3. A simple, inexpensive set of collapsible kitchen-quality strainers that can be sterilized and used to strain the flushed fat. |
Abdominal fat, whether transplanted alone or in combination with overlying dermis and assuming that it survives transplantation, is inclined to act like abdominal fat—as is illustrated by the patient in question.
Her postoperative weight gain, while minimal, did translate to a very slight increase in the size of the augmented areas of her buttocks.
Cleansing of the fat—usually done by repeated warm Lactated Ringer’s solution flushes, which removes blood and related particulate matter—ensures that what is transplanted is reasonably viable and stands a good chance of surviving.
Figure 3 (page 28) depicts a very simple, inexpensive set of kitchen-quality strainers that can be sterilized and used to strain the flushed fat.
The measuring cups shown are made of silicone rubber and, consequently, can also be sterilized and are effective during the gentle transfer of the cleansed fat from strainer to a syringe.
A similar but “clean” syringe-based liposuction system is employed to introduce fat into the area(s) in need of augmentation, again ensuring methodical, paced introduction of fat.
I believe that use of “larger” cannulae—again, in the 3- to 4-millimeter-diameter range—minimizes the trauma to the transplanted fat as it passes from syringe through cannula to its ultimate destination.
In the case of the patient in question, I attempted to position the transplanted fat into the upper halves of her buttocks, with the hope of not only augmenting her upper buttocks but also distending the skin of her upper buttocks, thereby providing a “lift” to her lower buttocks.
By the way, the ability to selectively augment with fat—that is, augmenting here but not there—which cannot be done as easily as with silicone implants, is a great “selling point” to fat transplantation.
|
See also “Does the Human Face Age Uniformly?” by Rima Bedevian in the November 2007 issue of PSP. |
 |
The areas into which the fat was transplanted were not pretreated with any wetting solution. This avoids distortion of those areas, which might lead to operator misjudgment of the volume of fat necessary to achieve the desired surgical result.
Finally, you must apply a snug, virtually immovable compressive dressing to the patient, postsurgery. This garment is replaced 48 to 72 hours later by an appropriate elastic undergarment, which is worn constantly for 7 to 10 days.
Limited physical activity (again, no sitting for a week or so) minimizes displacement of the transplanted fat and contributes to patient comfort postoperatively.
CONCLUSION
As I conceded earlier in this article, the results of fat transplantation or grafting are not always predictable. However, as with any plastic/cosmetic surgical procedure, when undertaken in the right patient with appropriate attention to detail, the results can prove very gratifying to patient and surgeon alike.
Richard T. Vagley, MD, FACS, is a board-certified plastic surgeon and owner of the Pittsburgh Institute of Plastic Surgery. He can be reached at (412) 681-2854.