 |
Today’s use of energy-based devices—specifically those that are light-based—to treat skin abnormalities can be traced back to ancient Greece, where the sun was revered for possessing healing qualities. However, there are significant differences among the conditions for which lasers and similar devices can and should be used.
“For high-risk skin cancers, such as lesions that are large, recurrent, or in aesthetically significant areas, Mohs surgery still has the highest cure rate and is the standard of care for that type of lesion. That’s more the preferred method,” says Anne Chapas, MD, a New York City dermatologist who specializes in Mohs surgery and laser surgery.
“Where I find that the laser and light devices come in is with people who have cancer syndromes—people who produce 100 skin cancers a year. It is just not feasible to have Mohs surgery on all of their skin cancers,” Chapas says.
Less-aggressive types of skin cancer, such as the superficial-spreading type of basal cell carcinoma, respond well to laser or light-based treatments. The slightly more aggressive or intermediate types of skin cancer, such as a squamous cell cancer, have more of a risk of metastasizing and are therefore more often treated surgically so that a specimen can be checked to see that the margins are clear.
“One of the things I like about the Mohs procedure is that as the cancer is being removed, you’re looking at it under the microscope to make sure you got all the cells,” says facial plastic surgeon Benjamin Bassichis, MD, FACS, of Dallas.
“I want to know that it’s all gone, and with the light-based treatments, you don’t know if you’ve cleared the cancer on the skin’s surface, but left little fingers of cancer that are now spreading underneath the skin. The top layer looks well healed, but now you have skin cancer underneath,” Bassichis says. “I can say that after the patient comes back from Mohs, we’ve done everything we can to know that the cancer is gone.”
Treating Precancers
Whereas surgical removal is the treatment of choice for active skin cancers, there is evidence to support that treating precancerous lesions or actinic keratoses with energy-based devices can be quite successful.
“With precancerous lesions we can get a little bit more lax in terms of trying to get out the lesion,” Bassichis says. “If you biopsy something that’s a precancerous lesion, use the laser. I definitely agree with that. Chemical peels, lasers, light-based devices, photodynamic therapy—all those are great options.”
One factor to consider in deciding which type of energy-based device to use is whether a spot treatment is required or whether the area to be treated encompasses more of a field effect of actinic damage.
“With the field treatments, you can treat them with certain pharmacological therapies, such as fluorouracil, imiquimod, or diclofenac—these are all modalities that are FDA-approved for the treatment of [precancerous lesions],” says Zakia Rahman, MD, FAAD, a board-certified dermatologist in Palo Alto, Calif. “Other destructive or surgical modalities include the use of cryotherapy and lasers.
 |
| Left to Right: 1) Benjamin Bassichis, MD, FACS, is board-certified in facial plastic and reconstructive surgery and otolaryngology. He is the medical director of the Advanced Facial Plastic Surgery Center in Dallas and a clinical assistant professor of the University of Texas– Southwestern Medical Center. 2) Anne Chapas, MD, is a board-certified dermatologist who specializes in Mohs micrographic surgery for treating skin cancers, laser surgery, and aesthetic procedures. She is an assistant professor at New York University School of Medicine and is in private practice at the Laser & Skin Surgery Center of New York. 3) Michelle Ehrlich, MD, FAACS, is a board-certified dermatologist and fellowship-trained cosmetic surgeon with Palos Verdes Dermatology Associates in Rolling Hills Estates, Calif, director of cosmetic dermatology for the Harbor–UCLA Medical Center residency program in Torrance, Calif, and clinical instructor of dermatology at the University of California, Los Angeles. 4) Zakia Rahman, MD, FAAD, is a board-certified dermatologist practicing in Palo Alto, Calif. She is also a clinical instructor of dermatology at Stanford University. For more information about the participants in this roundtable, including how to reach them, please contact [email protected]. |
“Traditionally, what people used in terms of laser and light therapy for the treatment of actinic keratoses or superficial squamous cell cancers, or even for the prevention of skin cancer formation, has been ablative laser resurfacing with a carbon dioxide laser as well as the erbium lasers,” Rahman says.
Energy-based treatments basically obliterate any lesion. “If you were doing an ablative type of laser treatment, such as a carbon dioxide laser or an Er:YAG laser, they actually vaporize the tissue, so there’s no specimen left behind,” says dermatologist Michelle Ehrlich, MD, FAACS, of Rolling Hills Estates, Calif. “What people tend to do more and more of, as opposed to that type of treatment, are these less-invasive lasers using a topical photosensitizer.”
ALA Mode
The most commonly used energy-based devices for treating actinic keratoses are the laser and light-based devices. With those, a photosensitizing chemical—usually 20% 5-aminolevulinic acid (ALA)—is applied topically and allowed to incubate before being treated with a blue or red laser, or light-based device in the blue or red spectrum, which activates the chemical wherever it has been absorbed. As the chemical activates, it destroys the cells that have absorbed it.
Chapas prefers to also inject the ALA directly into the tumor to penetrate the full thickness. “I put enough into the tumor to see blanching in the tumor,” says Chapas, who usually treats the sites with a noncoherent light, preferring a blue light therapy in the 430-nm wavelength region.
Chapas has a database of about 50 patients who were treated by injecting ALA into nonmelanoma tumors and receiving photodynamic treatment. Among those patients, 17 basal cell skin cancers were treated, with nine having clinical clearance; five lesions were biopsied, with four having no tumor—one had tumor remaining in the treated area; and six lesions were awaiting further follow-up. Chapas also treated some squamous cell carcinomas. Fourteen out of 17 lesions were deemed clinically clear; two were biopsied, but showed no evidence of squamous cells.
 |
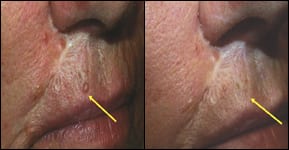 |
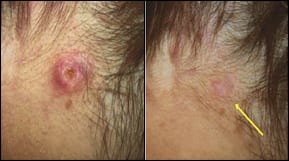
| This patient is a 53-year-old woman with basal-cell nevus syndrome. Both lesions are biopsy-proven basal-cell carcinomas that were treated with topical and intralesional 20% aminolevulinic acid. After a 1-hour incubation, they were illuminated with noncoherent blue light at 10 J/cm2. The lesion on the neck is shown 1 month after treatment; the one on the lip, 2 months afterward. These areas have been clinically free of tumors for more than 2 years. |
“I do have several patients whom I’ve seen for about 2 years out, and the ones who were clear with the treatment have remained clear,” Chapas says. “I haven’t had any long-term recurrences yet.
“The other aspect of this,” Chapas adds, “is that we have a group of patients with tumors in whom we treated not just their cancer but their surrounding skin as well. We feel that helped clear some of the lesions that had potential to become larger skin cancers before they even came out. So a lot of these patients who were getting 10 or 20 skin cancers a year, started getting only one or two.”
Besides blue light, there is also red light available in the 600- to 630-nm range to treat these precancers; red light is preferred in Europe. “Unfortunately, there aren’t too many available in the United States,” Chapas says. “People have also used pulsed-dye lasers to activate [the photosensitizing chemicals], but some studies have shown that this doesn’t have as great a photodynamic effect—that it doesn’t activate the medicine as strongly—as some of the brighter light sources.”
When treating actinic keratoses with light-based devices, Ehrlich tends to use the photosensitizing chemical with either a red-light base source or a red-wavelength laser. “I do a fair amount of ablative treatments with an Er:YAG-type laser, but I do that more to treat a full face for rejuvenation than to treat an individual skin cancer,” Ehrlich says.
“I almost never use LEDs for this type of treatment. I sometimes use IPL, but because it is a little bit of a spectrum, as opposed to a single wavelength of light, it tends to give you a little bit more of a reaction—occasionally a slight overreaction,” Ehrlich says, “which is not to say that it’s not useful under certain circumstances, but there’s always a little bit more risk of burning.”
Success Rates
Catching precancerous lesions and preventing them from becoming cancers is a major benefit that energy-based devices can offer when treating actinic keratoses.
“We have a huge amount of success with precancerous lesions or actinic keratoses,” Ehrlich says. “Each one of these has about a 10% chance of turning into a basal cell or a squamous cell cancer each year.”
Success rates of energy-based treatments have been reported with an average of 70% to 80% clearance; some studies have even found as high as a greater than 90% clearance rate.
There is much discussion in the field about photodynamic therapy improving patients’ overall skin texture and quality. The use of the topical photosensitizer during treatments has provided additional advantages such as controlling acne, shrinking pore size, improving scars, and removing or reducing redness and sun freckling.
A good aesthetic effect is important for patients and physicians. “What I like about these light-based devices is not only can you treat the sun damage and the precancers, and prevent the formation of nonmelanoma skin cancers, but you can also give them some cosmetic benefit. You can improve the appearance of their skin—the wrinkling, brown spots,” Rahman says.
Because of the additional aesthetic advantages, these precancerous superficial skin treatments are frequently performed along with full-facial rejuvenation procedures that use one or more of the available energy-based devices.
Complications, Contraindications
Some patients do require additional treatment, in particular if there is a lesion that is persistent or hyperkeratotic. In those instances, a biopsy should be considered to determine whether there is a malignancy.
Whereas complications from the treatments are rare, there are side effects to consider, including possible infections, scarring, erythema, hypopigmentation, and hypersensitivity to sun and light, resulting in potential burns.
“Any time you use a laser, you can get issues of lightening or darkening of the skin,” Bassichis says. “Using the laser on patients with skin darker than type III, you can certainly get color issues. Using chemical peels to below the jawline can lead to scarring of the neck.
“Any laser or light-based treatment used in the wrong area can lead to problems. A lot of those will end up in my office for reconstructive procedures,” Bassichis says.
As with any procedure, there are also contraindications to consider when treating someone with an energy-based device—the first and foremost is anything that is even suspected of being a melanoma, in which case surgical treatment is again the preferred option.
Other contraindications for energy-based treatments include patients who have an infection, those who are allergic to ALA, those who are on photosensitizing medications, and those who cannot avoid going outdoors. “I would definitely not treat them with photodynamic therapy,” Rahman says, “because they’re going to have a very brisk response if they don’t avoid the sun after putting on a photosensitizer.” Patients who are treated with the photosensitizing chemical used in the laser and light-based treatments are advised to avoid sun exposure for 48 hours after treatment.
Cost also can be an inhibitive factor with energy-based treatments using photosensitizing agents, which tend to be more expensive than using a topical regimen, such as a fluorouracil, which is relatively inexpensive.
Chapas says the major limitation of using energy-based devices to treat actinic keratoses is that they have only been used for such instances for a relatively short time.
“Because we’ve only been using it for 4 years, we can’t give people an idea of recurrence rate. For a lot of cancer studies, you need to have 5 years of data before you can say that something is an effective cure for this type of skin cancer,” Chapas says. “We’re telling people this is investigational; we need to see [them] and monitor the area that was treated regularly. If the patient’s not compliant with that, it really isn’t a good treatment for them.”
Patients who are treated for actinic damage will require follow-up, usually every 1 to 3 months, depending on the type and degree of damage, the treatment received, and their healing response.
Future Treatments
While the use of energy-based devices to treat precancers continues to increase, the photosensitizing chemicals and light-based devices are also continuing to develop.
“Currently, there is only one FDA-approved ALA. There are some other photosensitizing chemicals that are in the process of getting FDA approval,” Ehrlich says. Those chemicals would provide more options when using energy-based devices.
“In terms of the light-based sources themselves, the issue is always trying to fine-tune which wavelengths of light are the most specific for activating the chemicals,” Ehrlich says.
New red and blue light sources are under development, as well as some combination red- and blue-wavelength devices. “There are a multitude of light-based devices out on the market,” Rahman says. “I believe the next big trend will be FDA submission for nonaesthetic indications. These patients will still get aesthetic benefit, but the goal is to show that these can reverse photodamage and reduce the risk of nonmelanoma skin cancer formation. My hope is that the laser industry will continue to develop these light-based devices and make them less expensive and easier to use.”
Traditionally, blue-wavelength light has had more use in the United States. In Europe, however, red-wavelength lights are used more often. “What we tend to see from the European data is that the red lights are better,” Ehrlich says.
Chapas says Europe is far ahead of the United States in using lasers and light sources for treating nonmelanoma skin cancers. “In a lot of countries, such as Norway, this is the standard of care to remove a lot of these cancers,” Chapas says. “What’s nice about the red light is when you get into the longer wavelengths—when you move from a blue light that’s 400 nm to a red light that’s 600 nm—the larger the number, the deeper the penetration of the light. In theory, you would think you would get a better result for the tumor if the light can penetrate deeper.”
Beyond the use of red light, Europe is also leading the way in how the photosensitizing chemicals are applied for the treatments. “The Europeans, instead of using a solution for the levulinic acid, use it in a cream-based levulin that is supposed to penetrate better. There’s been a lot of studies with this cream-based levulin, which is still awaiting FDA approval,” Chapas says.
There may be other treatment options in the future as well.
Fractional Advantages
Rahman cites a study being published by dermatologist G. Scott Herron, MD, of Palo Alto, Calif, on the use of 1550-nm nonablative fractional resurfacing for the treatment of actinic keratoses. Through the treatment, a 1550-nm erbium fiber laser is used to target water in the skin. Instead of ablating the tissue, the laser coagulates it and lets the body naturally remove it.
This differs from other nonablative modalities that do not cause immediate tissue ablation in that it is fractional. Fractional resurfacing works by sparing tissue. The normal tissue that surrounds these microthermal zones—the tissue injury—quickly repair and extrude the damaged tissue. “Herron found that the cure rates on average were about 74%,” Rahman says. “The cure rates are approaching those of traditional modalities such as topical medications and photodynamic therapy.”
 |
| See also “Rejuvenation Without Ablation” by Catherine Maley, MBA, in the April 2007 issue of PSP and “Skin Cancer and Your Patients” by Andrew T. Cohen, MD, in the September 2006 issue of PSP. |
Rahman, who conducts research on treatments with fractional technology, says dermatologists have been looking at the use of fractional ablative resurfacing. “So instead of using something like a 1550-nm [laser], we’re going back to the CO2 laser, but trying to make it safer than the traditional CO2 lasers,” Rahman says. “Ablative fractional resurfacing is currently being studied for improvement of photodamage and skin laxity, but the goal is to see if it can treat actinic keratoses and prevent nonmelanoma skin cancer formation like traditional CO2 lasers. It’s the same idea as using a traditional CO2 laser, but because you’re sparing some tissue, your body heals much more rapidly.”
For now, and perhaps the foreseeable future, the scalpel remains the preferred treatment choice.
“It still has the highest cure rate [and] the best cosmetic outcome,” Chapas says. “[These other devices are] something that I think is going to complement Mohs surgery, but I don’t think it’s ever something that’s going to replace it.”
Danielle Cohen is a contributing writer for Plastic Surgery Products. For additional information, please contact [email protected].





