By Adam D. Schaffner, MD, FACS
Tackling challenging revision breast augmentation cases
Breast augmentation with implants consistently ranks as one of the most popular cosmetic surgery procedures performed in the United States, but many patients will undergo subsequent surgeries to solve problems caused by the primary augmentation. Such problems include, but are not limited to, capsular contracture, implant malposition, fold malposition, double bubble deformity, symmastia, rippling, deflation of saline breast implants, ruptured implants, desire for a different implant size (larger or smaller), and the need for a breast lift.
 |
| Careful preoperative consultations can reduce the need for revision breast surgery. |
All plastic surgeons aspire to have the lowest reoperation rate possible, yet reoperation rates of approximately 20% in sequential postmarket approval studies have remained relatively constant. Failure to improve this rate should serve as a motivating factor for all plastic surgeons who perform breast augmentation.
Careful preoperative consultation, frank discussion of expectations, and use of 3D imaging can all help reduce the need for any revision breast surgery, but there are still times when revision surgery is necessary.
Revision breast augmentation is more difficult, complex, and less predictable than primary breast augmentation. Tissues may been thinned due to the weight of the breast implants, anatomic planes may have been violated, anatomic landmarks may be distorted, and scar tissue will make dissection more difficult. There may be more bleeding, especially if the scar tissue is extensive and if the capsule has to be removed due to capsular contracture.
Reoperation Versus Revision
There is a difference between reoperations and revisions. To paraphrase Scott Spear, MD, professor and chairman of plastic surgery at Georgetown University Hospital in Washington, DC, reoperations include any event that transpires in the vicinity of the patient’s breast augmentation. This may include breast biopsies and scar revisions. It may also include change of implant size and/or subsequent mastopexy. The reason for reoperation may be out of the control of the surgeon or patient. While it is important to reduce the rate of reoperation, it is of paramount importance to reduce the rate of revisions due to capsular contracture, implant or fold malposition, infection, extrusion, double bubble deformity, symmastia, or implant deflation or rupture.
 |
|
| Before | After |
 |
|
| Before | After |
| Figure 1. Patient shown after fourth augmentation and after revision augmentation using neosubpectoral pocket with ADM. | |
As with all surgical procedures, the best results come from critical preoperative analysis. The patient’sdesires and preferences must be discussed and honored to the extent they are realistic and reasonable. Unfortunately, some patients desire implants of a certain size, which may not be in their best long-term interest. They may also desire more cleavage than is possible given their intermammary distance. It is incumbent upon the plastic surgeon to educate the patient about the risks and benefits of breast augmentation to set appropriate expectations and minimize the risk of complications. The optimal implant volume will fill the stretched envelope and the existing breast parenchyma. The optimal implant dimensions for a given patient should be determined after assessing base width, anterior pull skin stretch, nipple to inframammary fold distance, sternal notch to nipple distance, and pinch thickness. While a patient may be a candidate for a range of implant sizes and styles, having an implant which is too large or too wide may cause problems that are difficult to correct and result in long-term dissatisfaction. It may also result in the need for revision surgery to correct rippling, atrophy, skin stretch, and visible edges of the implant.
In short, plastic surgeons must recognize that implant volume is not the most important factor in implant selection. Breast implants should be selected based on proportions and dimensions. The final appearance of the augmented breast is related to the initial amount of breast tissue, its dimensions, and the size of the chest wall. Biodimensional planning with precise measurements will lead to greater success in breast augmentation. Three-dimensional computer imaging and simulation programs now allow surgeons to better visualize and plan for breast augmentation surgery. Such programs also help to communicate possible results with given implants to a patient during the consultation. Chest wall asymmetries may be better detected and shown. This technology may reduce the likelihood of operations for implant size change. Still, it should be clear that the images simulated are not an implied guarantee of the result.
Currently, plastic surgeons in the United States have the option of using saline or silicone breast implants which are smooth or textured. With the recent approval by the FDA, all plastic surgeons now have unrestricted access to highly cohesive, form-stable gel breast implants. This will further advance our ability to provide implants with minimal risk of wrinkling or rippling or capsular contracture while providing shape to the breast.
Choice of incision is critical. The choices include inframammary fold, periareolar, transaxillary, and periumbilical. The incidence of complications such as infection, altered sensation, and risks of capsular contracture are lowest with the inframammary fold incision. This incision provides direct access to the subglandular and subpectoral planes without violating the breast parenchyma. However, if the incision will not fall into the inframammary fold after augmentation or if the breast has a constricted lower pole, other options may be considered. The periareolar incision provides central access and enables one to lower the inframammary fold. The transaxillary incision avoids placing a scar on the breast. However, it requires one to operate on tissue other than the breast and is associated with a higher rate of complications. The same is true of the transumbilical approach. The key is to understand the advantages and disadvantages of each of the incisions and choose the most appropriate incision for each patient.
The plane where the implant is placed is also critical. Placing the implant in the subglandular plane in the absence of adequate soft tissue coverage may result in thinning of the tissues, rippling, and palpable implants. There is a higher incidence of capsular contracture with implants placed in the subglandular plane. However, textured implants in this plane may have a lower incidence of capsular contracture. All implants placed in this plane make mammograms more challenging to interpret compared to implants placed under the pectoralis major muscle. In practice, the majority of “subpectoral” implants are placed in the “dual plane” position, whereby the superior pole of the implant is under the muscle and the lower pole of the implant is in the subglandular plane. The placement of implants in the dual plane will minimize the risks of developing complications associated with implants placed in the subglandular plane.
Of course, meticulous surgical technique with precise pocket dissection is key. Obtaining hemostasis throughout the case, observing strict sterile technique, avoiding the use of gloves with powder, using antibiotic solution, and employing technologies such as the Keller funnel™ allow the implant to enter the breast without touching the surgeon’s gloves or the patient’s skin. These are all points to consider to minimize the risk of postoperative complications.
Concepts in Practice: Revision Case Studies
Consider these two cases. Both of these patients were previously operated on by experienced plastic surgeons who are certified by the American Board of Plastic Surgery.
The first patient is a 29-year-old female who desired cosmetic breast augmentation. She underwent four previous breast surgeries. At the age of 25, she had a primary breast augmentation using a Mentor Moderate Plus Profile 300-cc saline implant filled to 360 cc. It was placed in the dual plane position using an inframammary fold incision. Her original bra size was 32B. She was 5 feet 4 inches tall and weighed 103 pounds.
Nine months after the original augmentation, she went to another plastic surgeon to exchange the saline for silicone implants, increase the size to 500 cc, and address rippling and bottoming out. The plastic surgeon exchanged the implant to a Mentor 500-cc high-profile smooth round silicone gel implant. Strattice, an acellular dermal matrix (ADM), was used to reinforce the inframammary fold after a capsulorraphy was performed.
The patient experienced symmastia following this procedure. The same plastic surgeon attempted repair via capsulorraphy and placement of Strattice. The implants were exchanged from 500-cc to 550-cc high profile. The patient states she was advised by the surgeon that he had to replace the implants and did not have any 500-cc implants available at that time.
Unfortunately, the symmastia repair was not successful. The same plastic surgeon operated on her again to repair the symmastia. External scars occurred in the superomedial pole of the left breast as a result of marionette sutures. The patient was dissatisfied with the repair and sought consultation from multiple plastic surgeons. She subsequently elected to have a fifth procedure on her breasts to repair symmastia. She declined to have any additional incisions placed on her breasts and refused implants smaller than 475 cc.
A neosubpectoral pocket technique was used supported by Strattice Contour 3. The 550-cc implants were replaced with 475-cc Mentor smooth round high-profile silicone gel implants (Figure 1). She also had triamcinolone injections and subsequent pulsed dye laser treatment to treat scars in the superomedial pole of the left breast. Her current bra size is a 32DD. She is happy with the results.
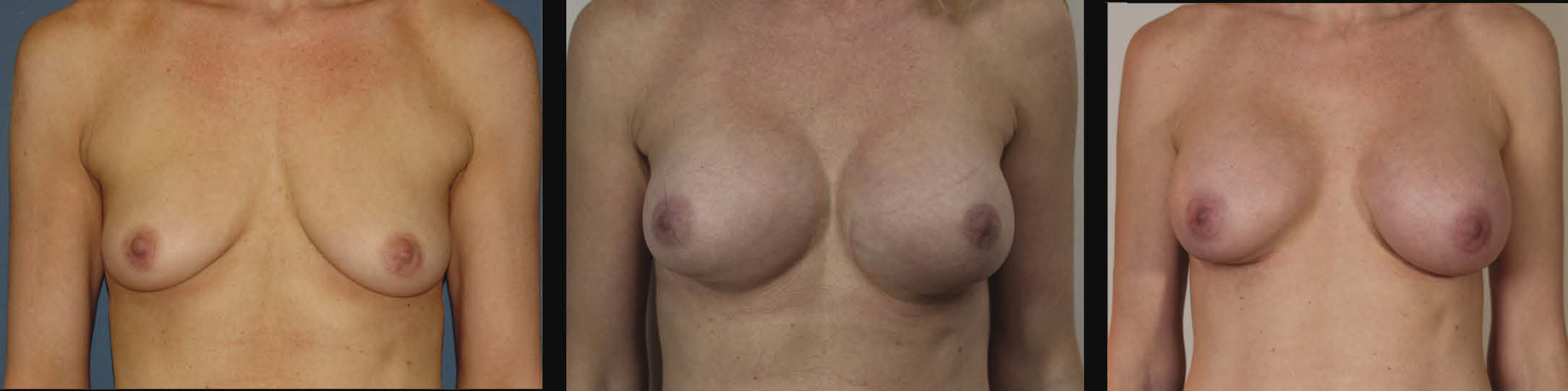
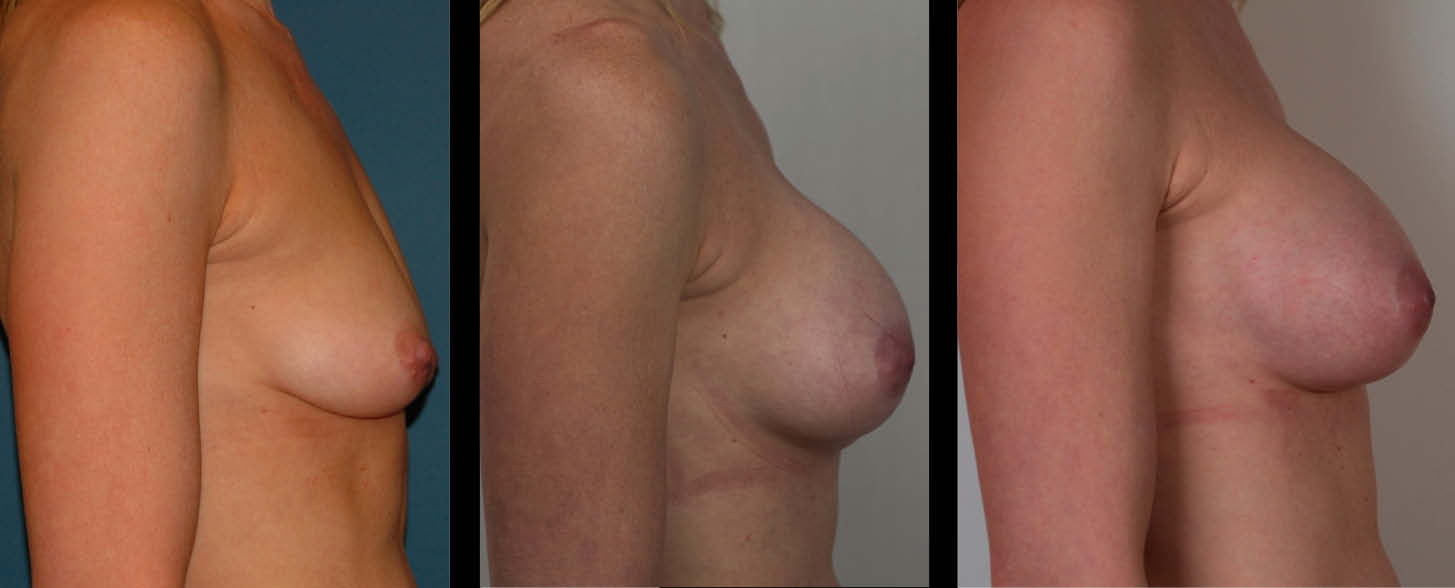
The second patient is a 40-year-old female who underwent primary breast augmentation to restore breast volume lost after having breastfed two children. She is 5 feet 6 inches tall and weighs 123 pounds. She had Allergan Style 15 339-cc smooth round silicone gel implants placed. She was a 32C before the augmentation and a 32DD after the augmentation. She experienced fold malposition, bottoming out, and symmastia, and desired correction. One year after her primary procedure, revision breast augmentation was performed using the neosubpectoral pocket technique supported by Strattice Contour 2. The implants were exchanged for new identical implants as bubbles were noted within the gel of the original implants (Figure 2).
 |
 |
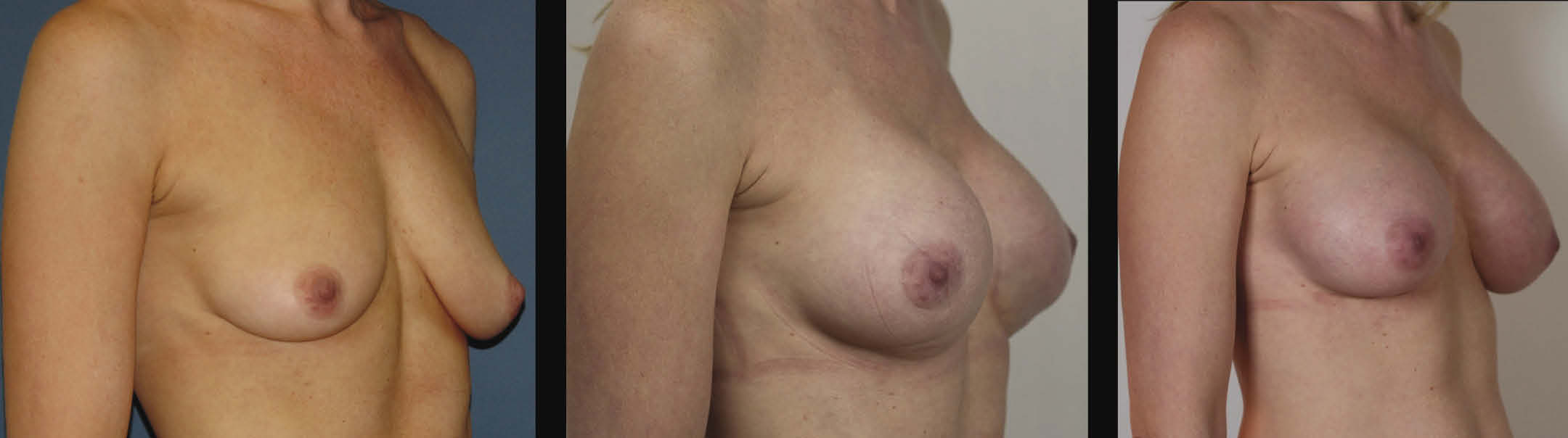 |
| Figure 2. Patient shown before augmentation, after primary augmentation, and after revision augmentation using neosubpectoral pocket with ADM. (Click images to enlarge) |
Acellular dermal matrices have enabled plastic surgeons to address complex problems in revision breast augmentation such as thinned tissues, fold malposition, and capsular contracture. It provides additional thickness and coverage to minimize implant palpability and supports the implant to prevent bottoming out or rippling. ADMs also prevent the implant from migrating into a previous pocket when changing the implant from the subpectoral position to the subglandular position, or visa versa. Lastly, ADM has also been shown to reduce the rate of capsular contracture.
The concepts raised in this article should motivate all plastic surgeons to continue to strive to reduce the rate of revision breast augmentation.
| Additional Reading |
|
Adams WP, Rios JL, Smith SJ. Enhancing patient outcomes in aesthetic and reconstructive breast surgery using triple antibiotic breast irrigation: Six-year prospective clinical study. Plast Reconstr Surg. 2006;117(1):30-36. Bengston BP. The highly cohesive, style 410 form-stable gel implant for primary breast augmentation. in: Scott L. Spear, ed. Surgery of the Breast: Principles and Art. 3rd ed. Wolters; 2011:116;1346-1365. Hedén P. Breast augmentation with anatomic high-cohesiveness silicone gel implants (European experience). in: Scott L. Spear, ed. Surgery of the Breast: Principles and Art. 3rd ed. Wolters; 2011;115:1322-1345. Jacobson JM, Gatti ME, Schaffner AD, Hill LM, Spear SL. Effect of incision choice on outcomes in primary breast augmentation. Aesth Surg J. 2012;32(4):456-462. Maxwell GP, Gabriel A. Use of the acellular dermal matrix in revisionary aesthetic breast surgery. Aesth Surg J. 2009;29(6):485-493. Spear SL, Bogue DP, Thomassen JM. Synmastia after breast augmentation. Plast Reconstr Surg. 2006; 118(7S):168S-171S. Spear SL, Bulan EJ, Venturi ML. Breast augmentation. Plast Reconstr Surg. 2004;114(5):73e-81e. Spear SL, Dayan JH, Bogue D, et al. The “neosubpectoral” pocket for the correction of symmastia. Plast Reconstr Surg. 2009;124(3):695-703. Tebbetts JB. Dual plane breast augmentation: Optimizing implant–soft-tissue relationships in a wide range of breast types. Plast Reconstr Surg. 2001;107(5):1255. |
Adam D. Schaffner, MD, FACS, is in private practice in New York City. He can be reached via [email protected]. The author wishes to thank Scott Spear, MD, who provided him with the knowledge, training, and skill during his fellowship to help treat challenging revision cases.




