Inverted nipples are a source of health concerns and emotional stress for both men and women. They may be congenital, defined as hypoplasia of the lactiferous ducts, or are acquired due to carcinoma, ductal mastitis, macromastia, or breast surgery. The incidence ranges from 1.8% to 3.1%.
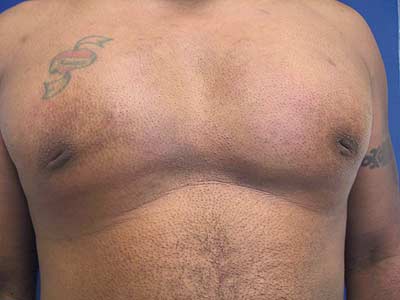
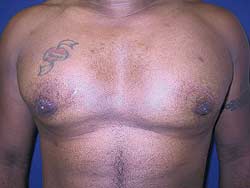
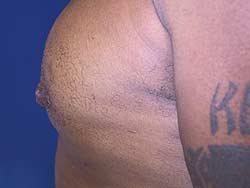
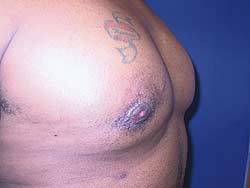
Preoperative view
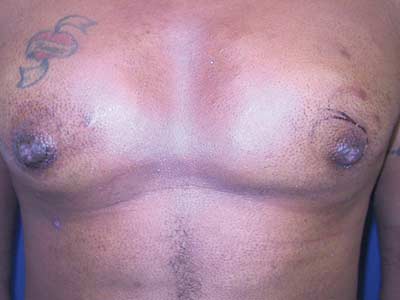
Postoperative view, 2 weeks after correction
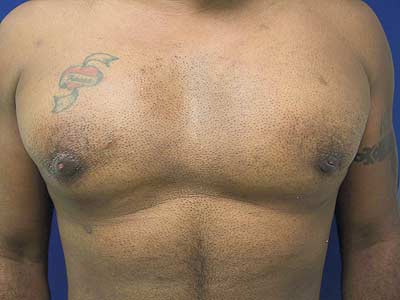
Postoperative view, 12 weeks after correction
In this article, we discuss acquisition of inverted nipples due to surgical treatment of gynecomastia in a young male. Gynecomastia is hypertrophy of breast tissue in a male. This should be differentiated from pseudogynecomastia, or breast enlargement secondary to excess subcutaneous fat seen with weight gain and obesity. Medications, anabolic steroids, androgen receptor antagonist monotherapy, marijuana use, or cosmetic products containing lavender and tea tree oil may cause gynecomastia. Any condition that results in decreased testosterone, increased conversion of testosterone to estrogen, or increased estrogen in the male can cause hypertrophy of the mammary glands.
GYNECOMASTIA TREATMENT BACKGROUND
Gynecomastia is characterized by an increase in areolar diameter, swelling of the breast, formation of an inframammary fold with nipple-areola complex (NAC) sliding and ptosis, and asymmetry. Incidence of gynecomastia is around 65% among 14-year-old boys but levels off to 30% to 50% among adult men.
Simon et al describe four categories of gynecomastia. Grade I and grade IIa mammary glands are mildly and moderately enlarged, respectively, without excess skin. Grade IIb and grade III glands are moderately and severely enlarged, respectively, with considerable excess skin. Grade I and II gynecomastia may be treated by suction-assisted lipectomy alone or in combination with glandular excision to treat moderate enlargement. Grade III gynecomastia may be treated by liposuction in combination with skin excision or reduction mammoplasty. Complications of surgical gynecomastia treatment include hematoma, seroma, infection, breast asymmetry, sensory changes, and nipple or areola necrosis or inversion.
During the treatment of gynecomastia, excessive resection of the glandular tissue may lead to loss of support of the NAC. This can lead to inversion of the nipple as well as scarring to the underlying musculature.
CASE STUDY
This is a 38-year-old male who presented with concern and embarrassment of his inverted nipples. This deformity was exaggerated with contraction of his pectoralis major muscle. He describes a history of glandular excision under the nipples as a young teenager.
On examination, he had a well-healed inferior periareolar scar as well as irreducible inversion of both nipples. While there was tight adhesion of the NAC to the underlying muscle, no saucer deformity, masses, or lymphadenopathy were present.
The patient was brought into the operating room and given IV sedation with a board-certified anesthesiologist present in an accredited office-based surgical suite. During this procedure, he also elected to undergo standard abdominal liposuction using the super-wet technique. Tumescent solution was placed in the area to be liposuctioned. Using a 60-cubic-centimeter (cc) Tumi syringe and a 3-millimeter (mm) cannula, 120 cc of aspirate was obtained. This was transferred to 60 cc luer lock cannulas and allowed to decant on the back table. The rest of the abdominal liposuction was performed with vacuum assistance.
Through a 3-mm stab incision in the lateral inframammary fold, a pickle fork was used to release scar adhesion around the NAC and approximately 5 cm of surrounding skin. Upon complete release, the inverted nipples were easily reduced. Once the oil and serum were removed from the aspirate, the fat was transferred using a 2-mm bucket handle infiltration cannula. Specifically, 15 cc was placed directly under the NAC, and another 30 cc was feathered circumferentially in a pyramidal fashion under the rest of the undermined skin.
The nipple was then stented in the everted position using the technique described by Stevens. A 2-0 nylon was passed through the nipple, then through two perforations at 180° apart on a 30-cc plastic specimen cup, and then tied over the top. This stent was left in place for 2 weeks.
At 4 months follow-up, the patient healed uneventfully with full correction of the inverted nipple deformity as well as resolution of the dynamic component of deformity with muscle contraction.
SIMPLE AND SAFE TECHNIQUE FOR TREATING INVERTED NIPPLES
Nipples are a source of great concern in terms of body image and sexuality for both genders. As such, most patients opt to correct the inversion deformity, and the first surgical correction was completed by Kehrer in the 1880s. Various methods of inverted nipple correction have been described, most of which include the use of areolar dermal or breast parenchymal flaps; release of the fibrous bands; and sutures, skin hooks, or body jewelry to maintain nipple projection.
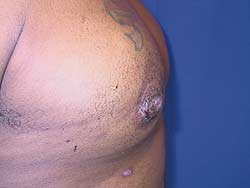
Postoperative view of right nipple, 2 weeks after correction
Postoperative view, 4 weeks after correction
Postoperative view of left nipple, 2 weeks after correction
Postoperative view of right nipple, 4 weeks after correction
Our technique to correct the acquired inverted nipple involves release of scar adhesion through the use of a pickle fork, replacing the missing tissue under the NAC with an autologous fat transfer, and maintenance of nipple projection through the use of a Stevens stent. Release of the scar adhesion allows for easy eversion of the nipple, and the fat transfer resolves the issue of tissue deficiency. The postoperative suture and stent help preserve eversion and provide additional support through the early healing phases. All aspects of the inverted nipple deformity are thus addressed and fully corrected. This method is safe and minimally invasive, and should be considered by the surgeon for any patient considering inverted nipple correction surgery, both acquired and congenital.
The technique described here fully corrects the acquired inverted nipple deformity, with no recurrence of inversion. This technique may also be applied to the correction of the congenital inverted nipple. It is simple to perform, safe, and provides aesthetically pleasing results.
Magdalena Dumin, MD, is a pediatric resident at Loyola University Medical Center in Chicago.
Irvin M. Wiesman, MD, FACS, is a board-certified plastic surgeon at the Wiesman Cosmetic Surgery and Wellness Institute in Chicago. Both can be reached via [email protected].
RECOMMENDED READING
Bembo SA, Carlson HE. Gynecomastia: its features, and when and how to treat it. Cleveland Clin J Med. 2004;71(6):511-517.
Burm JS, Kim YW. Correction of inverted nipples by strong suspension with areola-based dermal flaps. Plast Reconstr Surg. 2007;120(6):1483-1486.
Cordova A, Moschella F. Algorithm for clinical evaluation and surgical treatment of gynaecomastia. J Plast Reconstr Aesthetic Surg. 2007;61:41-49.
Huang W. A new method for correction of inverted nipple with three periductal dermofibrous flaps. Aesthetic Plast Surg. 2003;27(4):301-304.
Kim DY, Jeong EC, Eo SR, Kim KS, Lee SY, Cho BH. Correction of the inverted nipple: an alternative method using two triangular areolar dermal flaps. Ann Plast Surg. 2003;51(6):636-640.
Lee MJ, DePoll PA, Casas LA. Aesthetic and predictable correction of the inverted nipple. Aesthetic Surg J. 2003;23(5):353-356.
Niewoehner CB, Schorer AE. Gynecomastia and breast cancer in men. BMJ. 2008;336(7646):709-713.
Ritz M, Silfen R, Morgan D, Southwick G. Simple technique for inverted nipple correction. Aesthetic Plast Surg. 2005;29:24-27.
Scholten E. A Contemporary correction of inverted nipples. Plast Reconstr Surg. 2001;107(2):511-513.
Schwager RG, Smith JW, Gray GF, Goulian D Jr. Inversion of the human female nipple, with a simple method of treatment. Plast Reconstr Surg. 1974;54:564-569.
Simon BE, Hoffman S, Kahn S. Classification and surgical correction for gynecomastia. Plast Reconstr Surg. 1973;51:48.
Stevens WG, Fellows DR, Vath SD, Stoker DA. An integrated approach to the repair of inverted nipples. Aesthetic Surg J. 2004;24:211-215.
Wiesman IM, Lehman JA Jr, Parker MG, Tantri MDP, Wagner DS, Pederson JC. Gynecomastia: an outcome analysis. Ann Plast Surg. 2004;53(2):97-101.


