
Although Julie Ann Woodward, MD’s resume is as long as it is impressive, she is more often recognized for her frequent appearances on the national speaker circuit and pivotal work in designing coursework at scientific meetings. Her stature among cosmetic surgeons will be realized in early 2011, when she will be a keynote speaker at the American Academy of Cosmetic Surgery (AACS) meeting.
She is currently a fellow of the American Society of Ophthalmic Plastic and Reconstructive Surgery, the AACS, and the Women’s Dermatologic Society.
As Chief of the Oculoplastic and Reconstructive Surgery Service, she directs the oculofacial fellowship program for oculofacial surgery at Duke University Medical Center in Durham, NC, where she has trained about 10 fellows.
“One of my favorite things of the year is calling the newly accepted fellow to tell him he’s been accepted to the program,” she says. “I know the impact that this has on his life. When you accept someone into your fellowship, you’re changing that person’s life. You’re changing their whole career and the rest of their life. Think about it. If they didn’t get accepted into that fellowship or into oculofacial surgery at all, they could be leading a completely different life.”
Woodward’s career bears witness to the truth of her statement. When she was doing her own fellowship, she trained under Sterling Baker, MD, FAACS, who pioneered the use of the carbon dioxide (CO2) laser for blepharoplasty procedures.
When Baker and a few other dermatologists began looking at laser skin resurfacing, he discovered while using the laser to treat actinic chelatis that it just happened to improve the rhytids around the mouth.
PRACTICE AT A GLANCE
- Practice: Duke University Medical Center
- Location: Durham, NC
- Specialty: Oculofacial surgery
- Years in practice: 12
- New patients per year: Approx 350
- Patients seen per day: 10-15
- Days worked per week: 5
- Days surgery performed per week: 3-4
- Number of employees: 7
- Office square footage: 4,000 (shared)
Her fellowship with him and his laser work changed her life, and today, Woodward specializes in cosmetic laser surgery of the skin. She is the director of the aesthetic laser surgery course at both the American Academy of Ophthalmology and the American Society of Ophthalmic Plastic and Reconstructive Surgery, and has written numerous textbook chapters on techniques of incisional laser surgery.
Her involvement with lasers under Baker’s tutelage is what brought her to work in a university setting. “I was in private practice for almost 2 years in Houston, and then I moved to Duke University,” she says, because of a cosmetic laser surgeon who had left the university. The university owned several lasers. She was interested in putting lasers to use in research and in actual cases, so it was a good match, she says 10 years later.
It was an easy move to make, in some ways. “If you’re starting out in private practice and your interest is in lasers, it’s really costly to start up a laser practice,” Woodward explains. “The machines are just so expensive. One laser can cost up to $100,000, so to have multiple machines can be cost prohibitive. In that type of setting, I either had to join a group that had an interest in building that specialty or go to Duke University, where I filled a niche left by another physician who left the university.”
Another reason for Woodward and family to move to North Carolina: Her parents left Dallas 8 years earlier and moved to Winston-Salem. “Once we arrived in North Carolina we figured out that I was pregnant with my first child, so it was nice to be close to parents,” she adds.

Woodward loves to teach, and wants to see the university fellows have the careers they want and become successful.
LIFE AT UNIVERSITY
For Woodward, there are many advantages and disadvantages to working at Duke.
“Lack of control of your practice can be frustrating at a university,” she says. “I cannot purchase new equipment on a whim. Finally, about a year and a half ago, I started working with a laser company [that] recognized my skills and has loaned me a laser to do research with.”
She relies on laser-based devices from Lutronic Inc, Princeton Junction, NJ, and has been very happy with them. “It has completely revamped my practice, because the results are amazing and the patient’s downtime is minimal,” she says. “There probably was an advantage being at Duke to have [Lutronic] ask me to work with their equipment.

As chief, oculoplastic and reconstructive surgery service, Woodward directs the fellowship program for oculofacial surgery at Duke University Medical Center.
“Recently, Duke is making new commitments to supporting a cutting-edge aesthetic program. I am very happy that Duke is realizing that having a state-of-the-art aesthetic program is a necessity, because in some respects this is a reflection on the rest of the university. So, there is value in supporting it.”
She highlights the advantages to working in the university setting. “The quality of the other physicians and students is amazingly high,” she says. “It’s so comforting to know that you are taking top-notch care of your patients. I completely trust all the other physicians on the faculty. It’s just an extremely collegial group of people that I just love to work with, and that is a huge plus. If I ever left, I would really miss my colleagues, because we do such an amazing job of taking care of patients together.”
Were she to go into private practice, she would miss the high energy at Duke. “It’s just fun to be in a stimulating environment where you’re surrounded by so many young trainees that are so enthusiastic about learning. I have residents and fellows trailing around behind me. I’m teaching them about these patients, and they’re so eager to learn. They’re so eager to get involved, and that’s really exciting.”
Along with students who bring a fresh vibrancy to Duke, Woodward gets some relief from having to work odd hours one would find in a private practice.
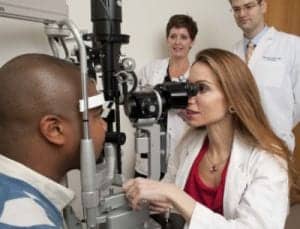
Woodward specializes in cosmetic laser surgery of the skin, and is the director of the aesthetic laser surgery course at the American Academy of Ophthalmology.
“When I was in private practice, I had to take a lot of calls from the private hospitals,” she says. “One of the advantages of being at the university is that I don’t have to take as many calls, because I am the backup to those that are first answered by the residents and fellows. I have three little kids; I prefer not to have to come to the hospital in the middle of the night and on my weekends. It’s really wonderful to have that kind of support. I always do remain available, however, to see a patient if necessary. Although faculty do not have to work as many odd hours, we do work many long days because we have administrative meetings and educational activities after hours.
“Academics involves certain trade-offs of lifestyle and money, and is not for everyone. It’s all a balance. It’s all about lifestyle. I grew up in an environment with my father as an academic professor in neuroscience, with his national and international colleagues. His students all took tenured academic positions, so that is the community that I know and enjoy which comes with being at Duke. My dad is my greatest mentor and, of course, my mom is the greatest supporter of my creative energy.
“What do I find intriguing? I know some people in private practice who absolutely hate working with residents. They think they’re pests. I actually like having the residents around. I think it’s fun to teach and it’s fun to pass on knowledge … and make sure that these people turn out to be well-educated physicians.”
A most certain advantage of being at the university is that you have a huge patient base. People come just because it has a great reputation. How different is the experience for the patient? Are they all willing to have the students learn on them?
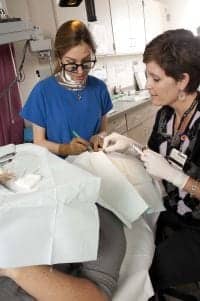
Woodward praises the extremely high level of quality and patient safety at Duke University.
“Duke is a private university,” she says. “But we also do take care of all indigent patients in Durham County—gratis. It’s nice to take care of a certain amount of patients at no cost and be able to give back to the community. But all in all, it is a private university that accepts private insurance, so we have to be sensitive to the patients’ wishes when we’re training.
“I always give the patient the option to have only me do the surgery,” she continues, adding that some patients will “be OK with” the fellow participating in the surgery.
“It is a teaching institute, and patients at Duke understand that. Most patients are expecting to see trainees around. Many of the patients enjoy having the trainees around because they understand they’re getting extra points of view. An oculofacial fellow is a fully trained ophthalmologist, so sometimes they bring extra education from their own background knowledge, as well.”
Although a large patient base is drawn to the university based on its reputation, the university needs to maintain that excellent reputation as part of its brand, Woodward says. This limits the marketing capacities of individual careers. “They discourage personal branding since they need to brand the university. The university will not support individual physician Web sites. Web sites at the University are often not as dynamic as the Web sites of the private practitioners. Some of the physicians at Duke have created their own, and I may consider doing the same.”
Whereas this could be a major career deterrent for some, for Woodward it all works out. “All in all, because I have such a strong reputation in the area and I have so many referring doctors that I’ve worked with for 10 years, I really get an amazing amount of referrals. I don’t really have the need to advertise very much. We barely spend any money in local advertising—just a very small amount.”
Her office is always hopping. “I do about 50% cosmetic surgery and about 50% reconstructive functional. My aesthetic surgery has about a 3-month wait list. Basically, it’s just word-of-mouth referrals from within the university and also outside, within the state of North Carolina, Virginia, Tennessee, and South Carolina,” she says.
How does she balance this work against her duties as a teacher? A fellow who works with her daily assists her. “He works clinically with me 80% of the time, and 20% of the time he has to do research and works independently at the VA [Department of Veterans Affairs]. I teach regular lectures to residents to help them prepare for their in-service exams. All the incoming residents get a series of basic lectures. I also do other lectures around the university, teaching other departments.”
For her, one thing that is especially fun about being at Duke is her joint appointment with the school’s dermatology department. “The dermatology residents rotate with me in addition to the ophthalmology residents,” she explains. “I also work very closely with neurosurgery, otolaryngology, and general plastic surgery. One way to look at it is that I have two jobs. I have one job that takes care of functional patients, and another job for taking care of cosmetic patients. This is great because I never get bored. They each provide different feelings of reward, and I need to do both to feel good about helping patients in different ways. I have a special passion for taking care of patients that are functionally blinded by benign essential blepharospasm. I enjoy doing both jobs in a way that simultaneously educates young physicians.”
THE CADAVER LAB
Duke University presents both advantages and disadvantages in the world of research, as well. Woodward is upbeat, though, about her access to a cadaver dissection lab. Most people in private practice just don’t have that, she says. “We have the ability to inject our cadavers with latex, so we can differentiate arteries from veins. We’re submitting a grant right now to do some academic dissections of certain areas on the face. We’ve also done some studies in the lab to try to track how Botox causes ptosis.
“A funny [aside] is the man who runs the dissection lab. Before he ran the dissection lab, he was a butcher. He’s very good at what he does.”
A disadvantage? How about the very stringent institutional review board (IRB) process, she says. Any paper that’s published out of Duke can take up to 6 months to be passed through the institution’s IRB committee, she notes.
FUTURE WORLD
Universities are slow to understand how to support aesthetic practices, as evidenced in minimal advertising and a lack of dynamic Web sites.
“Convincing universities to stay current with new technology can be challenging, but I believe that Duke is realizing the importance of doing this in order to be perceived as ‘cutting edge’ by the community,” she says.
For Woodward, newer laser-, radio-frequency-, and ultrasound-based devices hold promise, as they can provide increasingly popular nonablative skin-tightening treatments on the face and neck— although the term “skin tightening” is not officially recognized by the FDA. New treatment plans will combine technologies, she adds, such as ablative with nonablative treatments.
Woodward asks that all who read this keep in mind and appreciate where their training came from. “The fact that there are physicians at universities that are willing to take the time and effort to teach is the reason why we all have our careers in medicine today,” she says. “Some physicians who just get out [of school] are so interested in making money that they forget to give back to their training programs.
“At some point, all physicians had to train at a residency or fellowship program that was university-based,” she adds. “They wouldn’t even be where they are today unless a university supported them. There are people who are working at universities who accept less money, but they’re doing it because they love to teach and want to see people have the careers they are hoping for. We want to see them be successful.”
Sarah Russel is a contributing writer for PSP. She can be reached at [email protected].






